Every year, when I speak with biomedical technicians who have recently taken the CBET exam, I am always amazed at how many anesthesia questions they tell me they had on the exam. Personally, I believe anesthesia is a specialty rather than general biomed, so many examinees may not service this type of device. However, the CBET exam tests on general knowledge of the entire field, and anesthesia is definitely a part of that. So, with anesthesia questions on the exam, we need to look at some basic information about anesthesia and possible questions you may see on the exam. This article will take a closer look at some of the more fundamental aspects of anesthesia and the personnel who operate this type of medical device, along with some possible areas that the test may cover.
Personnel who operate the anesthesia machines are, of course, the anesthesiologist, who is a medical doctor, or MD, and the nurse anesthetist. You may still hear people refer to the nurse anesthetist as a CNA, but in actuality, the proper term is CRNA. CRNA stands for a certified registered nurse anesthetist. The newer term for CNA refers to a certified nurse’s aide. I mention this because some of the newer types of questions set up small scenarios about equipment problems, and you must understand these nomenclatures to understand the questions.
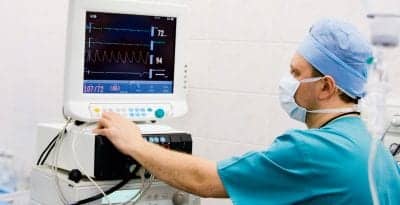
Anesthesia machines contain monitoring and alarm devices such as a pulse oximeter; an airway pressure monitor; and ventilator controls for setting ventilator volumes, rates, and I:E ratios.
The word “anesthesia” actually means loss of bodily sensation, but you may hear medical personnel refer to two types of anesthesia: local anesthesia and general anesthesia. Local anesthesia—sometimes referred to as regional—is when the patient is conscious but nerve impulses are temporarily blocked from transmission so there is no sensation of pain. You may refer to this type of anesthesia as numbing, such as what your dentist may perform while doing routine dental work. General anesthesia is what we usually associate with surgery and the operating room environment.
There are four stages of anesthesia, which are stages I through IV. Stage I in medical terms is analgesia, or the induction to unconsciousness. Stage II is REM stage, or excitement; and stage III is considered surgical anesthesia and is the proper depth of unconsciousness suited for surgery. The level IV of anesthesia is overdose and death, referred to as medullary paralysis in medical terms.
In the simplest terms, an anesthesia machine is a ventilator that has the ability to mix anesthetic agents into the gas, which is introduced to the patient. There are several types of anesthetic agents on the market today, but all anesthetic gasses should have certain attributes. These attributes would be nonflammable, lipid soluble, have low blood gas solubility, no organ toxicity, no side effects, not metabolized, and it should not irritate the patient’s airway. Some of the agents in use today are halothane, enflurane, desflurane, isoflurane, sevoflurane, and nitrous oxide. Each of the agents has slightly different properties from the attributes mentioned above, and the choice for use is determined by the needs of the particular patient’s condition and the anesthesiologist’s professional judgment. As an example, if a patient has cirrhosis of the liver, the anesthesiologist would more than likely not use the anesthetic agent halothane as it is toxic to the liver. The type of anesthetic agent the MDs would choose will likely be administered by the CRNA.
Anesthetic agents are administered through vaporizers, which are unique to the type of agent used. The vaporizers may use different methods to actually obtain the agent to administer to the patient. For example, with desflurane, this type of agent and vaporizer uses current to heat a heating coil, which is used to turn the liquid anesthetic agent into a gas, which is then blended with other gases for the desired anesthetic effect. Most vaporizers do not use electricity to create the gas, and it is recommended that all anesthesia vaporizers be serviced by the OEM as there are no serviceable parts for the in-house or ISO biomeds.
Understanding Anesthesia Machines
With some general information about anesthesia covered, let us take a little closer look into the anesthesia machine itself. Anesthesia machines can be broken down into a block diagram. The first block is the gas supply and flow-control section. In this section, you will usually find three gasses—oxygen, air, and nitrous oxide—along with regulators and pressure gauges for bulk and tank pressures. These gases are administered to the machine at a pressure of about 50 psi. If the oxygen pressure falls below a predetermined pressure, usually around 25 psi, alarms will sound and other gases may be reduced or terminated.
You should be familiar with the color codes of all these gases, which are green for oxygen, yellow for air, and blue for nitrous oxide. Within the oxygen pneumatic circuitry, you should be aware of a few items, such as the oxygen flush valve. When depressed, this valve will flush the patient’s lungs with oxygen when deemed medically necessary by the CRNA or MD. Oxygen, or a mixture of oxygen and air, is used to supply a gas stream for the vaporizer. Of course, this is dependent on which anesthetic agent and vaporizer are being employed.
The other item you must be familiar with in the oxygen circuitry is the mechanical linkage to the nitrous oxide. This device ensures the patient receives enough oxygen when nitrous oxide is being introduced to the patient. This linkage will ensure proper ratios of oxygen and nitrous oxide are delivered to the patient so lethal amounts of nitrous oxide can never be delivered to the patient. The last part of this portion of the machine is the flow rate indicators. These are calibrated in liters or milliliters per minute and are controlled by needle valves. Floating bobbins in a vertical cylinder indicate the flow of gas. These gases, along with the vaporizer anesthetic agent, are combined and introduced into the patient breathing circuit.
In the patient breathing circuit and ventilation portion of the machine, you should be aware of the two types of patient breathing circuits; these are the circle type and the T type. Each of these circuits has its own advantages. The circle type design uses less anesthetic agent, as the exhaled gasses are reused. In addition, this design also retains heat and moisture from the patient’s body. However, a CO2 absorber must be used to scrub the carbon dioxide from the recalculated gas. This absorber/scrubber is usually filled with soda lime crystals to accomplish this action and will change colors when needing to be replaced. This information has typically found its way into a test question on the exam, so make sure you are familiar with CO2 absorbers/scrubbers and the soda lime crystals. The T type circuit is easier to sterilize and has a simpler design, which requires fewer valves and no carbon dioxide absorber. In this section of the machine, you will find some type of mechanical ventilator, much like devices found in certain types of critical care areas. All modern anesthesia machines will also have a hand-squeezed reservoir bag to perform ventilation if a malfunction were to occur in the ventilator, and a switch to determine which type of ventilation will be performed—either mechanical or manual.
The last part of this section of the machine is known as the scavenging system. This portion of the machine is critical because it scavenges any exhaled anesthetic agent and takes it away from the operating environment so medical personnel will not be exposed to the anesthetizing agents during long surgery times. This information has also classically found its way onto the exam.
The last block of this device contains the monitoring and alarm devices. You will find devices such as a pulse oximeter measuring saturated oxygen levels, an airway pressure monitor, ventilator controls for setting ventilator volumes, rates, and I:E ratios, ECGs, and NIBPs. You may also see devices such as end tidal carbon dioxide monitors. For more information about anesthesia machines, I would suggest you check out the Web site for Virtual Anesthesia Machines at www.simanest.org/FabiusGS.html and www.anest.ufl.edu/.
John Noblitt, MAEd, CBET, is the BMET program director at Caldwell Community College and Technical Institute, Hudson, NC. For more information, contact .
REVIEW Q&A
- CO2 absorbers are employed with which type of patient breathing circuits?
- Circle breathing circuits
- T piece breathing circuits
- Anesthesia machines will alarm when incoming oxygen pressure falls to approximately what psi?
- 50
- 10
- 25
- 2.5
- Anesthesia machines can be manually set to deliver any amount of oxygen and nitrous oxide the operator desires.
- True
- False
- Typical anesthesia gas supply lines are what colors?
- Green, red, blue
- Black, brown, green
- Black, white, green
- Blue, yellow, green
See the answer
See the answer
See the answer
See the answer




