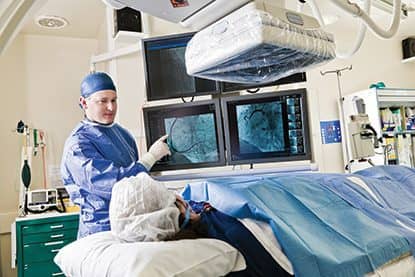
 HD video imaging and conferencing has already made its way into ORs, and as HD flat panel monitors become more prevalent in patient rooms, this technology may soon enable physicians to make their rounds via HD-videoconferencing.
HD video imaging and conferencing has already made its way into ORs, and as HD flat panel monitors become more prevalent in patient rooms, this technology may soon enable physicians to make their rounds via HD-videoconferencing.
From telemetry to infection control, understanding the important trends in health care can aid biomeds in controlling costs and improving patient care
By C. Wayne Hibbs
When we think about technology in health care, the first thoughts are often similar to NASA landing on Mars. People start discussions about multiple million-dollar projects for hybrid operating rooms, robotic surgery, fully automated laboratories, or the oncology treatment needed for all cancers. These are all important and expensive considerations in health care today. Hospital administrators and medical equipment planners stay up nights wondering what will be the next must-have medical technology, how much it will cost, and how much revenue it will generate. Then they start working on how to be the first in their region to get one and recruit more physicians to admit more patients to their hospital because of this new multi-million-dollar investment. There are many less exciting, but still important trends in health care that we need to understand to do our part in controlling health care costs and improving patient care.
The HD-MD
With new affordable patient vital signs devices and the high definition (HD) flat panel monitors that we have put in every patient room, how long will it be until physician rounds are just a videoconference? The physician can spend an hour or two making HD-video rounds to free up more time to spend with critical patients that really need bedside care. In a “rounding room,” like a dictation room, the physician can review the chart from the electronic medical record and talk to the patient using technology that was too expensive for even the e-ICU concept 10 years ago. Today, it can be an app on your iPad or Android phone. A dedicated iRobot is also in use in a number of hospitals developed by the maker of the Roomba vacuum cleaner.1,2
The e-ICU concept was developed to provide 24/7/365 advanced nursing and ICU physician monitoring to critical patients through videoconferencing. The systems of 2003 were standard resolution, one-way communication where the e-ICU monitoring specialist had to call the attending staff by “red phone” to discuss trends and recommendations for better medical outcomes. The remote connections to limited electronic medical records and the cost for the videoconference capabilities made the e-ICU a very limited application.
Now in 2013, the availability of electronic patient record information, the improvements in consumer and commercial videoconferencing and multitasking, and multifunctional PC workstations have made remote patient care both much better and much more affordable. The premium e-ICU monitoring studios now routinely monitor 35 to 50 patients per staff member with HD bidirectional video communications. The technology of high-resolution pan-tilt-zoom cameras in the patient rooms allow everything from reading the setting on the bedside infusion pump to assessing pupil dilation on the patient.
| Most hospital labs now have a benchtop analyzer with DNA probe testing methods for 1-hour identification of powerful and resistant bacteria. |
Telemetry monitoring suites (often called war rooms or grand central station) can monitor 64 patients per workstation with direct communication back to the primary care provider with trend, arrhythmia, and response to medication information at a much lower cost than the original central station monitoring at every nursing station for 16 patients on the unit.3
Super-Telemetry for All
As health care is seeing the application for telemetry and continuous patient monitoring expanding, the clinical utilization has not changed much since its introduction. In the world of biomed equipment service and repair, we have been dealing with the function of telemetry monitoring since the 1970s. We have been through frequency changes brought about by the need for more bandwidth in HDTV transmission, the shifts from analog to digital signals, and the ever-increasing number of other wireless technologies in the hospital and outside world from powerful analog cell phones to Wi-Fi hot spots for digital smartphones.
Initially, all the physicians wanted was to admit their patients to the telemetry floor. Their patient might not have needed telemetry, but they knew that was where the best nurses worked. Today, most hospitals have expanded telemetry coverage in all patient and public areas with as many as 50% of the patients monitored by telemetry. Since Wi-Fi is already available throughout the house, some facilities are looking for a simple wearable Wi-Fi monitor that will provide a patient’s location, heart rate, and a nurse call button from admission to discharge.
Most of the current patient monitoring companies have been designing such a device for years with bits and pieces of their existing high-tech monitoring systems. These devices have always been too big, too expensive, and too easy to damage or lose. Just as the video gaming industry has developed super PCs with HD graphics cards and monitors that now are being delivered in our MRI, CT, and nuclear medicine equipment, the smartphones could do the same for patient monitoring.4
We have seen the initial moves from consumer electronics to patient care applications in the Bluetooth-connected insulin-infusion smart pumps with blood glucometers. The next step could be an app for your patient’s smartphone that connects by Bluetooth to the patient ID bracelet, which has radio frequency identification (or, RFID) for identification and location, then a pulse oximeter for O2 saturation. The pulse oximeter would not only provide O2 saturation, it would provide heart rate, respiration, and simple arrhythmia determination. The smartphone would provide the Wi-Fi connection, the patient location, and data memory, and could become a data processor for trend analysis. Several algorithms have been developed to predict clinical events from acute myocardial infarctions to seizures. This analysis power is now available in smartphone processors when given the necessary data from the ID smart band.
There should be a time in the near future where simple low-technology devices can make vital signs monitoring affordable both at home and from admission to discharge in the hospital. This basic information could also be summarized and linked to the patient record and medication history.
Superbugs, DNA, and Infection Control
Another important low-tech function that we need to implement is the understanding and handling of the growing problems in infectious disease. Most of the hospitals in service today were designed when a hospital had 80% semi-private rooms and 20% private rooms. In that design, there was an isolation room on each floor or unit. The isolation room had an anteroom that had negative or positive air pressure controls. An isolation room is for patients who have airborne infections or are very susceptible to infections from others. The isolation rooms were a large component of the 20% of private rooms. VIP patients were often admitted to isolation rooms for extra privacy.
Today, hospitals are converting semi-private rooms to private rooms and building new bed towers to maintain the same number of patients, but now in all private rooms. This modernization process keeps the patient census and license bed count the same, but it doubles the size of the facility and the distance a nurse will walk every day. It also doubles the number of clean supply, medication, and nutrition rooms needed that are filled with expensive inventory and equipment. However, it addresses the growing problem of hospital-based infections and patients who require isolation rooms.
| The availability of electronic patient information and improvements in videoconferencing and workstations have made remote patient care much better. |
Hospital microbiology labs have had 48- to 72-hour procedures for testing incoming patients for infective diseases for years, but some of the newer infections have become harder to detect by routine methods. When a patient has been in the hospital 72 hours before being diagnosed with an infective disease, a huge amount of cross contamination has already occurred. Treating every new admission as a carrier of an infective disease and keeping them in isolation for 3 days has often been proposed but has not been feasible because of limited isolation rooms, the increased staffing required, and cost.
In the last 5 years, molecular biology has had a major effect on incoming patient screening. Now, most hospital labs have a benchtop analyzer with DNA probe testing methods for 1-hour identification of MRSA, VRE, C-Diff, and a host of other powerful and resistant bacteria. Because of this early and easy screening of new patients, as many as one-third of the rooms on many med/surg floors now have personal protection equipment (PPE or isolation) carts parked in the hallways, hanging from the doors, or screwed to the wall just inside the door next to the hand disinfectant. The pharmacology of new and improved antibiotics and the DNA identification of new and improved bugs have made contact isolation rampant in health care.
The latest of the growing number of “superbugs” is a bacteria strain of Klebsiella pneumonia, with the common name of CRE. While the number of cases is still small, there is little to no sensitivity to the most effective antibiotics currently available. That makes control and containment of this infection a major problem in every hospital, clinic, and skilled nursing home.5
The new strain of bacteria is calling for a new level of technology for the care and maintenance of all the equipment that is used to treat these patients. Hospitals are training patient care staff on how they must work with the patients to prevent contracting it themselves or transferring it to other patients in the facility. Environmental services, central supply, and biomedical engineering staff must also develop the procedures to care for all the rooms and to transport the equipment that patients are exposed to in today’s high-tech health care.
The staffs of infection control departments are working on patient care training to reduce the number of these hospital-based infections due to staff members moving from room to room. They are also champions for new single-patient rooms, where each have their own vital signs monitor, rather than moving the rolling units from room to room as has been the common procedure for years. Infusion pumps should also be carefully cleaned between each patient use to minimize cross-contamination. The same is true on a much more frequent scale for the vital signs monitors, portable x-ray machines, EKG carts, ultrasound machines, portable endoscopy systems, and phlebotomy carts that move throughout the facility. These equipment travels are common ways the bacteria moves from patient to patient.
| To prevent the spread of infections, we need to develop our own “soiled/decontamination” rooms for bringing anything into our work areas. |
Then there are the ways the bacteria moves from hospital to hospital. If a patient in a nursing home develops a problem in the middle of the night and is rushed to the hospital by an ambulance, the ambulance, the patient stretcher, and the EMT staff all become new modes of transport from the existing facility to new facilities that may not know for hours that a patient is infected with a superbug.
In the biomed service performance, we need to treat every piece of equipment as if it is now contaminated. There are cleaners, disinfectants, UV-C lights, and other methods to pretreat and handle equipment that cannot be used directly on patients. We need to develop our own “soiled/decontamination” rooms for bringing anything into our work areas, just as central sterile processing handles contaminated surgical instruments. Once a contaminated item reaches our workbench, it becomes a breeding location for more contamination, just like a patient room. We do not want to work in a contaminated area or be forced to wear PPE at our workbench. We do not want to take these new superbugs home to our families. If we do not practice the same handling methods that central sterile processing has developed and proven, we become part of the problem of low-tech equipment causing high-tech infections throughout the facility.
As we evaluate the new high-technology, high-cost medical equipment, we cannot forget that the low-technology items that we already have are developing new applications and problems that must be addressed in our service support and maintenance functions, or they will become high-cost items also. 24×7
C. Wayne Hibbs is president of LifeStructures Technology Planning, Indianapolis, and a member of 24×7’s editorial advisory board. For more information, contact [email protected].
References
Read more about topics highlighted in the article.
1. Find out how telemedicine is changing health care: www.intouchhealth.com
2. Discover the iRobot mobile robotics platform: www.irobot.com/ava/
3. Learn more about the eICU: http://www.healthcare.philips.com/main/products/patient_monitoring/products/eicu/
4. Learn more about wireless vital signs devices: http://www.gereports.com/vital-signs-to-go-wireless-with-ges-body-sensors/
5. The Centers for Disease Control and Prevention discusses CRE: http://www.cdc.gov/hai/organisms/cre/cre-clinicians.html