Today’s hospitals face challenges to maintain and replace equipment on dwindling budgets and in a difficult economy, yet biomedical departments can help by creating a strategic replacement plan
By John McCarthy
In today’s world of increasing mergers and acquisitions, uncertainty in health care policy, a struggling economy, and dwindling budgets, hospitals have been faced with their own version of the perfect storm. Instead of extreme weather patterns, they are faced with an overwhelming demand for equipment replacement with limited funding.
While working to meet the large-scale challenges of today’s health care landscape, many hospitals overlook equipment strategy. Cyclically, executives review requests from the various departments within their hospital and health care system, and it is typical that the demand for replacement equipment far exceeds what is available within their replacement budget.
However, there is a way to meet these requests and clinical needs while still meeting budgetary limits—through a thorough, vetted understanding of what equipment currently exists, what condition it is in, and how it is being used. Biomedical/clinical engineering departments can be a valuable, front-lines resource in this process, helping executive teams make smart purchasing decisions.
The Technology Revolution
The truth is that many hospitals are filled with underused and underserviced equipment. Despite the clear financial investment all organizations make in purchasing and maintaining equipment, a hospital’s average utilization of mobile devices is only 42%. That translates to over half of the fleet being idle, which costs the hospital by locking up capital and driving up service costs.
By leveraging a few initial strategies, hospitals can effectively and cost-consciously replace outdated equipment and better use the equipment they do have. |
This is the norm and not the exception. According to a study conducted by GE Healthcare, the number of devices acquired for patient bedside use has exploded by 62% in the last 15 years. The increase in the number of necessary technologies for excellent patient care places great pressure on hospitals to buy technology, as well as increased pressure on in-house health care technology management departments to manage and maintain a constantly evolving and growing inventory.
Most hospitals conduct purchasing decisions on a request basis, meaning that, for example, based on feedback from nurses or staff that there are not enough IV pumps, a hospital’s executive team will purchase more of that equipment to fill the perceived need. Unfortunately, perception can vary from true need. Since many organizations do not have a way to tag and track assets in real time to understand what equipment is actually on hand or how it is being used, inventories can vary from what is actually in-house. Oftentimes, there are 50% more IV pumps than needed, either because the pumps are simply not following any prescribed journey through the hospital, are being left in places where they remain out of use for long periods of time, or are not being used to their full and efficient potential.
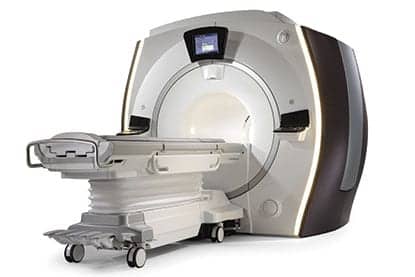
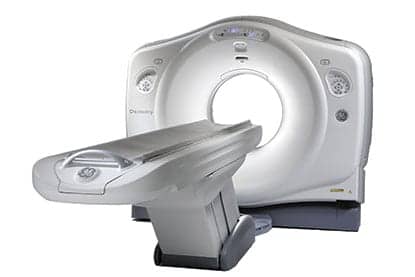 In today’s world of uncertainty in health care, hospitals are faced with an overwhelming demand for equipment replacement with limited funding. Photos courtesy of GE.
In today’s world of uncertainty in health care, hospitals are faced with an overwhelming demand for equipment replacement with limited funding. Photos courtesy of GE.
Alongside the issue of having too many devices and an unclear inventory, hospitals also face the related issues of replacement timing and service of its equipment. Under pressure to contain costs, hospitals are more and more frequently deferring equipment service and upgrades, only to find it must spend more money down the road to purchase an entirely new piece of equipment. In part, this is due to a lack of a defined asset-management program. Without knowing the state and utilization of an MR system, for example, hospitals may unnecessarily purchase a new system when, in fact, reordering workflows to improve utilization or updating the system could extend the life of the unit.
Bringing Purchasing and Spending Under Control
With the best intentions, many hospitals spend money and resources to replace what is perceived as outdated or end-of-life equipment, but have been doing so without a data-driven assessment of the equipment they already have.
By leveraging a few initial strategies, hospitals can effectively and cost-consciously replace outdated equipment and better use the equipment they do have, all while also serving their patients in the best way possible. Biomedical departments, as the vanguard of equipment maintenance and repair, can provide deep insights at each of these steps.
Step 1) Examine All Service Contracts
First and foremost, it is important to understand the state of an organization’s service contracts. A hospital may be paying for more than it needs, so looking closely at a service contract can help uncover significant opportunities for savings. For example, a hospital may have a CT scanner reserved for biopsy procedures. If the hospital is paying for round-the-clock service coverage on the biopsy unit—even though the unit is only used for a limited time during the day—coverage could be reduced and money saved.
A hospital’s clinical/biomedical department represents an invaluable resource in assessing contracts, since, as engineers, they are on the front lines and in touch with vendors and original equipment manufacturers every day. They can help assess the kind of coverage needed and advise on switching to a shared services model, where the in-house biomedical department assumes more responsibilities for equipment service but has flexible, customized coverage, training, and remote support from a vendor.
Despite the time it takes to gather and analyze data to create an asset-management program, it will pay significant dividends. |
It is true that by removing coverage from machines, hospitals start to assume more risk. Once coverage is removed, hospitals do run the risk of having a large invoice for time and materials if the equipment suffers a significant failure. Also, it may see a delay in response time by the service provider if the equipment is not covered under a contract. However, the math holds out. In noncritical areas of the hospital, even a one-time, big-ticket expense for an unexpected problem is likely to be far less than the cost of 24/7 coverage on a lightly used unit for a year. Finding opportunities for savings and ensuring appropriate coverage is a balance. While reducing unnecessary costs is vital, it is even more important to take only well-informed, smart risks.
Step 2) Consider Redeploying Your Inventory
When it comes to managing, replacing, and using equipment efficiently and effectively, it is important for hospitals to know what and where their inventory is at any given time. Real-time knowledge on equipment location can help health systems leverage resources throughout their system to ensure that hospitals have the right equipment in cost-effective ways that support clinical excellence. As biomedical departments know all too well, finding a specific piece of equipment can be a frustrating search process.
Redeploying an asset is almost always less expensive than buying a new one. For example, if a small hospital is in need of a new MR system—a significant investment—rather than purchasing a new one, hospital managers can look and see if a larger institution in their health system has an underutilized MR system. Could they, by increasing the efficient use of other MR systems in that facility, do without that specific unit? If so, the larger hospital’s MR system could be transferred to the smaller hospital at a fraction of the cost of an entirely new unit.
In addition to redeploying inventory across hospitals, it is also possible to redeploy assets to different floors within the same facility. Standardization makes it much easier to fix or replace a device when all of the other devices on the floor are alike and can easily be switched out without the need for new training. More importantly, maintaining consistency across certain devices ensures that each staff member on that floor is well-versed in the technology for timely, safe patient care.
Step 3) Profile Your Installed Base
One of the more frustrating things for a hospital manager is when they are unable to find necessary data in order to make asset-management and purchasing decisions. While time-consuming in the beginning, if managers create easy access to data about the utilization, age, software version, hardware version, current condition, service history, and replacement strategy of any given device in the organization, the organization will see benefits. Digging deep into the details about the life cycles of each and every one of their systems, managers can create a concrete technology plan with a 5-year capital budget. Knowing the status of equipment life cycles can help hospitals anticipate potential issues before they arise and more easily address those problems as they happen.
Walk the Walk: A Practical Case Study Example
Obviously, it is easy to tell someone the right things to do in order to save money when it comes to replacing and utilizing equipment, but showing them in practice is better. Take the example of a multi-hospital regional health system that needed help determining the best course of action for replacing its MR imaging assets.
Breaking out data by device, site, and year can help an organization see important data that is rolled up into the larger numbers. |
Using data from the health plan’s billing system, volume over a 3-year period, volume by site, and volume by device were analyzed. The data showed significant variations in the volume of breast and spine/pelvis procedures across different hospitals in the system. Utilization of equipment was also analyzed, finding that while some equipment was used 24/7, most utilization clustered in 8-, 10, or 12-hour increments, offering insights into how to best manage service coverage and assess the possibility of redeployment.
The data also found that despite instituting specific programs for women’s health and orthopedics across multiple hospitals, the volume at some hospitals for those program areas had declined—a finding that would not have come to fruition if the hospital had not analyzed volume by device in order to measure the impact of marketing.
In addition, accustomed to looking at data in a different way, the hospital leaders did not realize that outside competition was significantly affecting the volume of patients using their MR system. By not breaking out data by device, by site, and by year, the organization’s leaders were missing important data that was rolled up into the larger numbers, such as month by month and year by year total volume analysis.
After the analysis and realizing that they were underutilizing many imaging assets, the hospital decided to stop acquiring new MR systems. Instead, the organization took steps to redeploy existing units across various facilities to better meet site-by-site demand and increase utilization.
Staying the Course
Hospitals face multiple challenges each day from dealing with new reform policies to budget cuts. It can be overwhelming to look at equipment replacement and demand. However, it is more strategic in the long run to attack any equipment replacement and utilization issues head on, rather than to let them fester until they become more financially burdensome and urgent.
While it is time-consuming to gather and analyze service contracts, utilization, and other data in order to create an asset-management program, the ultimate savings in time and resources over the years will pay significant dividends. Managers will feel as if they have a better handle and understanding on the equipment that is vital to the care of their patients, as well as be able to run their hospitals as efficiently, effectively, and predictively as possible. Biomedical departments will have an easier time looking after the life-saving technologies used every day by physicians and nurses. And, most importantly, at the end of the day, patients will receive timelier and better-quality care by having well-maintained, easily accessible technology at clinicians’ fingertips. 24×7 Feature March 2013
John McCarthy is the general manager of asset management professional services for GE Healthcare.


