 |
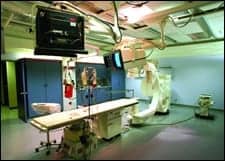
| Integrated ORs offer a streamlined and controlled environment with more space by eliminating the cart, removing equipment from the floors, and consolidating and reducing the amount of cables and wires in the room. |
Here’s the problem with downtime on video systems: You have brought a patient into the OR, put him or her to sleep, and now something doesn’t work. That’s not good,” says Duane Mariotti, BSEE, clinical systems engineer, clinical technology, Kaiser Permanente Southern California. Mariotti proposes that the only sure way to prevent downtime is through redundancy, and most other biomeds agree.
Some hospitals exercise extreme caution when it comes to their inventories by purchasing doubles of equipment whenever their budgets allow, to cover instances when the equipment goes down. For instance, Mariotti says if he needs four endoscopes, he will buy eight. Others are limited by finances and incorporate just a few extras, buying one or two extra endoscopes to back up four devices. In either case, biomeds strive to avoid downtime through preventive maintenance and regular service. Mariotti recommends that the proper test equipment, procedures, and knowledge can help to avoid or solve problems.
Exactly how much service a biomed performs varies with the institution. Some facilities employ more vendor or third-party repair providers, while others will handle as many responsibilities as possible in-house. Some combination usually exists, particularly since some video service is often restricted by the availability of parts, tools, or expertise.
“There are many pieces to a surgical video system, and you must deal with each individual piece,” says Charles Tyree, AAS, BSET, imaging specialist at Summa Health System, Akron City Hospital, Akron, Ohio. “At what level depends on how much your hands are tied by the manufacturer in obtaining parts and documentation. We have had equipment we had to send in because we could not obtain parts. In some instances, I’ve had to sign proprietary agreements to purchase certain parts.”
The Pieces
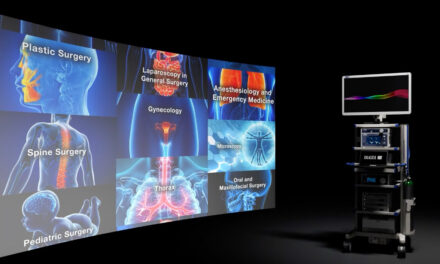
A light source; an insufflator; the camera control unit (CCU) and camera (such as on an endoscope or arthroscope); a monitor; and a recording device, which could be a VCR, DVD, or printer, typically comprise surgical video systems. Cables, connectors, and carts or integrated units hold it all together. Additional system options include hospital connectivity, LCD and wide-screen monitors, video switches and routers, high-definition video, C-Arms, the DaVinci robot, PACS, telemedicine, telestration (an annotation tool), and voice activation.
All of them typically fall under the biomed purview, and some require more attention than others. Joseph Flammang, CBET, senior biomed, CHI clinical engineering, Mercy Medical Center, Roseburg, Ore, notes that the insufflators and CRT monitors are the highest leakage offenders. Camera optics undergo a lot of damage as well. “We hope to upgrade to LCD monitors after our construction project is complete,” he says.
The Problems
Flammang avoids OR downtime by arranging for loaners when repairs to surgical video equipment need to be made, or by pulling the equipment from a spare cart. “I can usually get around anything being down,” Flammang says.
“Don’t be afraid to buy extras the first time around,” Mariotti advises. If the items are within budget, he recommends buying double what is needed. For more expensive parts, a redundancy plan is enough. “You don’t need to buy two video towers for ENT surgery, but you do need to know where you will pull a tower from should the ENT tower go down. The doctors and the patients expect the equipment to work,” he says.
“As far as the surgery staff is concerned, downtime is minimal because I just swap equipment out, get it up and running, and deal with the repair later, which could be a few hours, weeks, or even a month or more,” Tyree says.
Regular maintenance can help to avoid unexpected problems. The Joint Commission requires inspections within reasonable periods, and many biomeds perform routine surgical video equipment PMs annually, such as at Mercy Medical Center and Akron City Hospital. According to Tyree, nothing on the cart is extremely difficult to support or PM, although a couple of items, such as an insufflator and possibly an electrosurgical unit, if present, actually do need some higher level of PM, calibration, and repair than the other items, and would take longer to support than a printer, for example.
“It’s all routine. We perform PM once a year and do normal safety and function checks on all of the equipment. The insufflator PM and calibration is probably the biggest challenge. The rest takes care of itself,” Tyree says.
The Routine
One of the tasks during a PM is to check the cables and connections, which can also be an immediate solution on a service call. “An OR doctor or surgical technician will try to move something out of the way and yank out a video connection,” says Scott Reardon, medical and international account manager with Sencore Inc, Sioux Falls, SD.
“People abuse cables: They trip over them or forget to unplug them when moving equipment. Turnover is quick, there is a lot of equipment, and some things will get damaged,” Tyree says.
Integrated ORs have helped by reducing the amount of exposed cabling. “Any type of video or audio signal that you want can be ported to these systems,” Tyree says, noting that one doctor has even connected his iPod.
Flammang suggests that cables and connectors are not areas for scrimping. “If you have cheap cables and connectors, you will have a cheap signal or video. Use high-end cable,” Flammang advises. He also uses color coordination to match cables and inputs. “I like to organize the system as much as possible so that users are less likely to cause damage.”
The Light
In some facilities, biomeds train users to fix problems themselves, such as entrusting the surgical staff with changing the light component. “We have bought spare housings from the manufacturers and replacement lamps from third parties, and keep the extras in the OR. Users can then switch the lamp, reducing downtime,” Tyree says. He notes that this method also saves money—approximately $600 to $1,000 a lamp.
Occasionally, however, a problem with the light source is not visible to the human eye. Because the light is so bright, reduced output can sometimes be detected only through testing. This, according to Mariotti, requires a special test device. “This same meter can be used to test the fiber optic bundle,” he says.
The fiber optic bundle will break down over time, and the lamp will dim, so testing is necessary to find reduced output due to the fiber optics and/or the lamp. Mariotti even tests new bulbs. “Something as simple as changing a light bulb requires a high level of commitment to quality. I have seen a new bulb, out of the box, just put into a light source that is already shot,” Mariotti says. To ensure the best quality, Mariotti will use the same meter to test the light source as the vendor, once refusing to buy an entire system unless he could also get the light meter.
The Scope
Scopes are more complicated to service and tend to need more repair due to their fragility and susceptibility to abuse. The camera head is handled a lot while undergoing preparation, the procedure, and sterilization. The fiber optics and the coupling mechanisms (which attach the camera head to the scope) are prone to breakage.
“If I can buy the parts from the manufacturer, I can do these repairs in-house for less than $100. If I have to send the equipment to the manufacturer, it will cost three times that for the same repair—as much as $3,000—and be out of service for 2 to 3 weeks,” Tyree says, adding that a month-long wait is not unusual for one vendor.
He tackles the problem with user training, suggesting competencies annually. “We had some camera heads damaged because one of the people responsible for sterilizing them changed the process to save time and didn’t realize it was damaging the cameras. So we review the handling and cleaning processes periodically with employees,” Tyree says. He adds that Akron City Hospital also chose to purchase special metal cases in which to store and sterilize every camera.
The Picture
Monitors do not suffer from breakage like the cameras do, but they do require vigilant maintenance. Tyree found that housekeeping’s diligence in cleaning monitors was damaging them. Certain chemicals degrade the plastic, producing a physical interference with the image quality. “Follow the manufacturer’s recommendations for cleaning—often mild soap and water,” Tyree says.
Video standards range from basic image quality to high definition and include composite, RGB, S-Video, SDI, DVI, and 1080P HD. The systems are complex and can have a number of different sources for signal interference, including damaged cables, long cable runs, loose connections, computer equipment, electrosurgical units, ground loops, poor power quality, and surgical lights.
Initial testing and use will reveal these problems, but Tyree notes that any time something new is brought into the OR, new problems can be introduced. “It’s an ongoing issue,” he says.
Reardon notes that intermittent troubles can be the most frustrating, since it can be difficult to pinpoint something like a loose connection. “Tugging at the connector level can be hard to troubleshoot unless you stumble upon it,” Reardon says.
High-definition video is compounding the problem. As more devices are added to the system, everything interacts, meaning that one setting somewhere could override a corrective setting somewhere else. “You need to know how things are controlled,” Tyree says. He maintains control by turning off the auto-adjust function so that no connections are introduced that are a lower resolution. For instance, he describes the case of a high-definition monitor, with a primary fiber optic or DVI connection, and a composite, lower-resolution backup line. “If it is set to auto-adjust or self-calibrate, then depending on which connections are made first, as things are turned on, the monitor might adjust to the composite line rather than DVI, delivering lower resolution and lower image quality.”
Other equipment may also have resolution limitations. “It’s possible that a ‘digital’ endoscope does not have a high-resolution pickup device but is relying on scaling to show the image on a high-resolution feed,” Reardon says. He explains that scaling works well when transferring images from high-resolution to low-resolution images, but is not an ideal solution in reverse. “It’s not as high quality because the imaging process is making stuff up,” he says.
Testing image quality in high definition could potentially require new test equipment, Mariotti says, “at least for video and maybe monitors.” Standardized test procedures for output and resolution within an institution can help to establish processes that will accurately check image quality, but this becomes more challenging the more systems there are.
“Most hospitals have several different video systems and manufacturers, and it takes a long time to figure out how to accurately test all of those video boxes to make sure they are working correctly,” Mariotti says.
Lee W. Founds, an x-ray service engineer at CHI clinical engineering, Mercy Medical Center, describes a standardized process that begins with monitor calibration and is followed by tests using the appropriate signal generator, color sensor, measurement software engine, and color filters. Biomeds calibrate color balance, saturation, and tint, as well as proper contrast and brightness settings for ambient light conditions. “Our systems are on a 6-month calibration schedule, although we are evaluating a 3-month rotation on systems with CRT monitors,” Founds says.
Self-calibrating monitors are seen more frequently on PACS and other radiology systems than in surgical video units, but even for equipment with this feature, most biomeds feel manual testing is still needed. “Self-calibrating is perfect to start in the morning but doesn’t release biomeds from the responsibility they have to test the whole system,” Mariotti says.
Founds professes a similar philosophy. “We manually verify that the self-calibration feature is maintaining proper contrast, brightness, and gamma settings. The monitors on our PACS system appear to be very accurate at maintaining calibration, so we will continue to trust, but verify,” he says.
Monitors will need adjustments as they age, and eventually will need replacement. Tyree notes that after an initial adjustment, the hospital’s monitors have performed well for 2 years. “We’ve heard 2 to 3 years for a flat-panel life cycle,” Tyree says.
Biomeds will adjust the monitors to reference standards, but this does not necessarily mean all users will be happy. “The standard has not changed in 55 years, but doctors like to look at things differently,” Reardon says.
|
Find out more about the latest video management systems used in the OR in 24×7’s April article, “The Integrated OR.” |
 |
Some institutions will tweak the systems for individual doctors; others have found the doctors work with the referenced standard. “Image quality has to be defined, but it has a personal component to it. Some doctors want the cartilage to be perfectly white; others like a touch of gray,” Mariotti says.
In some facilities, a biomed is employed full time in the OR to tweak the equipment for each physician and procedure. Flammang notes that final adjustments are often done with the assistance of operating personnel.
Tyree says all of the physicians in his facility work with the same settings. “We set to bloodred with no deviation from one doctor to another. If that doesn’t look right, they will let us know.”
Renee DiIulio is a contributing writer for 24×7. For more information, contact .