?
By Michael Bassett | Service Solutions November 2012
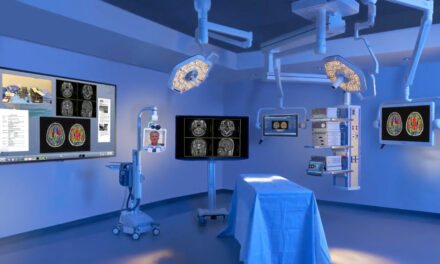
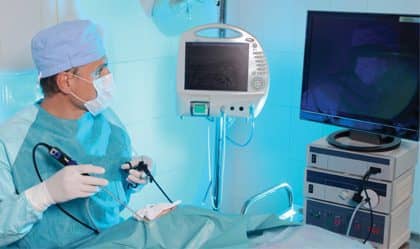
Go into any operating room today and you are bound to see a video system in place. In fact, video imaging is used throughout any health care department with “ology at the end,” says Farid Eslami, CCE, CBET, president of American Biomedical Consultant Group, Orange County, Calif.
In the operating room, surgeons use it to help them visualize procedures to either treat or diagnose medical conditions. In addition, the ability to capture and record a surgical procedure is valuable in a number of other ways, such as to teach and train, document the use of new techniques, or record interesting pathologies.
Michael Cohen, director of multimedia services for Ciné-Med, Woodbury, Conn, a medical communications and marketing company specializing in video production, has spent hundreds of hours in surgical suites watching biomedical/clinical engineers—and surgeons—deal with crotchety video systems.
“Video quality is going to be something the surgeon is immediately concerned with if there’s a problem,” Cohen says. “So the tech needs to be able to answer some important questions: Why is there no image on the monitor? Is the color an accurate representation? This has to do with understanding the white balance controls of the camera or adjusting the monitor.”
And the biomedical/clinical engineer needs to be able to troubleshoot. “If there’s a problem with the image, what’s the reason?” Cohen asks. “There are a number of reasons why there are image problems, and it could be something simple, like fog on the camera lens due to the temperature variation between the inside of the patient and the operating room. Anything can cause a picture interruption, so these are things the tech needs to know.”
Defining a Better Image
According to Eslami, slowly but surely high definition (HD) is capturing the market of imaging in surgery centers and operating rooms, particularly when it comes to cardiology or critical care. “That saves a lot of grief and heartache because physicians now get much more defined viewing,” he says. “So HD is pretty much becoming the standard as old monitors burn out and are being replaced. The minimum that anyone purchases is HDMI.”
Surgeons use video to help them visualize procedures and to record procedures to teach, train, and document the use of new techniques. |
Bryan Rhoades, FSS II, clinical engineer at Porter Adventist Hospital in Denver, works with a Storz OR1 system in 12 of the hospital’s operating rooms, two of which have HD.
Why two rooms? “We have Intuitive Surgical robots that are used in those two rooms, so we made them HD viewing so that the HD robot and the doctor can get the best signal for image quality,” Rhoades says. If images from those rooms are transferred to another room, they are downscaled.
The other rooms have video graphics array (VGA) display resolution, Rhoades says, although the hospital does have HD towers that can be taken in and out of rooms for procedures that require the insertion of scopes into patients. The towers also have a high-definition slave monitor that allows a second physician in the room to use HD, according to Rhoades.
Joseph Rittenberry, CBET, BMET III, lead tech at the St Clare Health Center in Fenton, Mo, says his hospital has Steris systems in each of its eight operating rooms, all of which are HD.
The system’s interface is DVI, which supports an extended graphics array (XGA) resolution of 720p, or 1280 x 768 pixels. It is not the highest HD resolution, but Rittenberry says it is good for the hospital’s physicians’ needs.
“They love the picture right now,” Rittenberry says. “So it’s really not necessary to get a higher resolution. We have 24-inch monitors, and when you are viewing that picture on that screen from 24 to 30 inches away, your eyes can only resolve pixels that are so small. Once they get smaller than a certain point, you really can’t tell the difference. So if I upgraded to a 1080p resolution (which will support video of up to 1920 pixels wide by 1080 pixels tall), it would be a higher resolution, but you really wouldn’t be able to discern the difference looking at the monitor.”
On other hand, Rittenberry notes that if his hospital ever decided to go with 32-inch monitors, then, because of the viewing distance in the operating room, a 1080p system would make sense. Interestingly, Rittenberry says he has some equipment that does not put out a high definition. For example, the hospital’s cardiac surgeon has his own video system that he has been using for several years. “It’s on S-video, and he’s really comfortable with it,” Rittenberry says. “He owns his own camera and head unit and has used it for 6 years, and he doesn’t complain about the resolution—he knows the only way he’s going to increase the resolution is by changing the system, and he doesn’t want to do that.
It is a good practice to know how to work with video in real time and know what to do with it after the procedure is over. |
Any system needs a backup in case the primary system has a problem. “Doctors don’t like to stop in the middle of a case,” Rittenberry says. St Clare Health Center’s system uses S-video, which carries standard-definition video, as its backup. However, this can be a problem because when the Digital Visual Interface (DVI) system goes down, “users never seem to remember how to use the backup system—and it’s really just one button on a control screen.” The DVI—a video display interface developed by the Digital Display Working Group—connects a video source to a display device, such as the viewing monitor.
In addition, once the DVI system goes down, the picture quality does degrade with S-video. “It’s an OK picture, but it’s not as sharply defined,” Rittenberry says. “You can watch it, but it’s like watching standard-definition television on a large HD screen—you can see the quarterback make a pass, but you can’t read his name or see his number while he’s doing it.”
Troubleshooting Video
“Our system is great—when it works,” Rhoades says, who adds that the system has so many components that troubleshooting can be “horrendous” and take hours to complete.
One problem, according to Rhoades, is that the facility’s system was customized when it was installed, so the documentation is not as thorough as it may have been for a system that comes “right out of the box.”
“You have to think of the system as a giant network,” he says. “You have a control tower in each room that controls functions, inputs, and outputs, and that’s connected via cable to a central control that can take that information and send it to any other room.”
However, without specific diagrams for each room, troubleshooting can be an adventure. “Every time I go in there I’m learning something new,” Rhoades says. “I like fixing things, but it can get frustrating.”
At St Clare Health Center, if there’s a troubleshooting issue Rittenberry will start with the image on the monitor. Experience tells him that if it is a monitor issue it is because it is losing its internal power supply or it is losing a color. If there is noise on the system (what was called “snow” back in the analog days), then he knows he has a converter problem.
Rittenberry runs into that issue because the range that he has to send his video signals (75 feet) is just too far for a DVI signal. He has to convert the signal from DVI to fiber optic—at multiple points—in order to extend the DVI source. “And the biggest problem we run into is when the converters fail,” he says.
Rittenberry then tracks down the problem—is it a switcher, converter, fiber optic line, or something else? The first thing he does is bring in a good known source—his own signal generator—and hook it up into the boom, plug it into a regular HD monitor, and look at the signal. If it is good, he has eliminated two of the converters. He continues with this process through the system. Once he finds out where the problem lies, he will replace both converters—the one converting the signal from DVI to fiber optic and the other converting it from fiber optic to DVI.
Biomeds need to know how to troubleshoot to address questions about image quality or why there isn’t an image on the screen. |
“I’ve probably had to replace about 3% of my converters,” Rittenberry says.
Eslami says that problems can occur at the viewing end with a monitor, or a PC with a monitor, or at the camera end with its configuration control system, where a user can run into trouble with something like the capture button function.
However, in Rittenberry’s experience, the problem usually does not lie with a monitor or camera. “With the cameras, the only problem is when you’re getting no video at all,” Rittenberry says. The cause of that is usually a broken seal on the camera head itself, which, when cleaned, could get some water intruding into the system. The surgical team knows that when it does not have a picture, someone needs to check whether there is a signal from the camera controller. If they do not detect a camera, they will change cameras. St Clare Health Center stays well supplied with cameras and has 14 on hand. It also keeps extra converters, but no backups of other components on hand, because, according to Rittenberry, there are just too many. If an emergency arises, he knows where to go to get a part overnight to have the next morning.
With the kind of budget restraints that most hospitals now work under, “they try not to stock parts unless there is a repetitive problem based on past service history,” Eslami says. “Then the biomedical tech can justify having the spare in hand.”
Rittenberry says the lack of spare parts on hand usually does not present a problem for operating room schedules. “If I can’t replace a component for a day, I’ll get together with the director and he’ll shift cases around,” he says. “Everyone doesn’t use video, so they’ll put cases in the room that’s down. And once I get the equipment I can usually replace it in around 15 or 20 minutes.”
Eslami agrees that most hospitals respond reactively to video system problems, which means they will take the time to troubleshoot, then order spare parts. How quickly a system needs repair depends on the type of medical procedure involved. “A gastrointestinal lab or a catheterization lab can’t afford to have downtime,” he says. “But, if they’re just videoing a surgery for training interns, then they can proceed while the system is down.”
As far as larger pieces of hardware, such as monitors and cameras, replacement usually is not an issue. “I’ve had to repair cameras, but not replace them,” Rittenberry says. “And I actually do have a spare monitor on hand.” He suggests a good practice to implement is to negotiate for extras. He says that when the hospital installed its system an agreement was reached to store one monitor in the hospital. This agreement allows the installing company to retrieve the monitor if needed, but in the meantime the hospital can use it.
For Rittenberry’s purposes, he has found this beneficial when it has taken 2 weeks or more for a monitor repair.
Preventive Maintenance
As far as preventive video maintenance is concerned, Rittenberry advises there is only so much a biomed can do. “I don’t look at the camera heads because they either work or they don’t,” he says. “I have to let the user let me know when it breaks.”
As for other parts of the system, Rittenberry says he does a full check twice a year by hooking up a signal generator to the system and “basically sticking my nose right on top of the monitor to see if I can see any small kind of sparklies in the system—one or two lines that may not be visible if you are standing three or four feet away. If I see a problem, I’ll start troubleshooting.”
“Most video imaging devices have cooling fans that should be cleaned once a year,” Eslami says. “And, color definition or white balance should be checked and calibrated as required by the manufacturer’s specification.”
In addition, Eslami points out that any electromechanical system in a critical patient care area should undergo functional, as well as quality control and electrical safety testing.
For the most part, Rittenberry says, there is no warning when something goes down. “And if the doctors even think there’s a problem, they’ll call me up and let me know before a case even begins.”
He will replace monitors regularly, however. “The monitors are just like those that you use at your house,” he says. “They’re on constantly, so after about 3 years it’s time to think about replacing them.”
Video Editing
While techs need to know about working with video as it is used in real time, it is also a good practice to know what to do with it after the procedure is over. For example, know what to do if a physician wants a 1-minute clip of a surgical procedure to use in a presentation. “It may seem simple, but it’s more challenging than it sounds,” Cohen says. “If you’ve recorded a three-gigabyte procedure, then it can be a challenge to get that clip. I know there are a lot more people who can edit video than there used to be, but there’s still no guarantee that the format that was used to record [the procedure] will go into iMovie or whatever you are using without some kind of conversion. And that could be beyond the scope of what the tech is capable of doing.”
That said, Cohen adds that most everyone who edits video is self-taught, and that the best way to learn programs like iMovie is by doing it. “Assuming a computer and software are provided, the tech should be able to learn the basics over the course of one project,” Cohen says. He advises that there are free online tutorials, as well as course books about specific software, but the major learning curves involve video software, since operating room recording systems can use different video formats.
“Mp4 should be usable natively in most editing software, whereas proprietary formats may need converting into a standard format,” Cohen says. “So some trial and error is to be expected. Likewise, video resolution can also differ. Broadcast HD is either 1920 x 1080 or 1280 x 720, while operating room video can be one of those or something different and nonstandard. So when trying to edit any resolution video, especially full HD, the specifications of your computer will make a difference.” 24×7 Service Solutions, November 2012
Michael Bassett is a contributing writer for 24×7. For more information, contact the editor.
Briefly DefinedWith the many variations in video today, it is helpful to understand some basic terms:
|