You reap what you sow” is an ancient adage (it originally stems from the Bible)—and it is fairly commonsensical. Yet, with the pressures of time and everyday living, it can still be difficult to always act with an eye toward the end goal. Not so for Karen Waninger, MBA, CBET, director of clinical engineering for Community Health Network in Indiana. This year’s recipient of the Association for the Advancement of Medical Instrumentation or AAMI’s HTM [Healthcare Technology Management] Leader of the Year Award was raised in an environment where the old axiom is a way of life.
“My years growing up on a farm taught me that one will only harvest the fruit of whatever seeds were planted,” Waninger tells 24×7. And so she has taken that philosophy into her professional life, where elevating the role of the biomed is a major focus.
“It’s true that many people do not even know we exist, let alone understand the value we can add as members of the health care team. We are often invisible, to the general public as well as the administrative teams within our own organizations. It is up to us to change that: not by demanding it, but by earning it,” Waninger says.
A major challenge and benefit for the industry is the ever-expanding—and constantly changing—scope of service. Clinical engineering departments not only service and maintain biomedical equipment, but also often participate in acquisition decisions, capital planning, and quality control efforts. Today, many biomeds spend more time on the floors interacting with clinicians and more time in meetings consulting with administration and leadership than in the past. In addition, the type of equipment they manage has expanded: Many have added specialties like scopes and radiology; some departments are experimenting with new types of service, such as work on home care equipment or revenue-generating efforts in the community; and everyone in the field is faced with learning a lot more about technology and networks.
“The expansion of our scope of service, and how we adapt to that, is something I believe is going to define how we are viewed by health care administrators. We need to look for and embrace new opportunities, invest in the training and professional development of our employees, and encourage creative problem-solving. The traditional service role is only going to be a small part of what we should be able to offer to help improve the bottom line for our organizations,” Waninger says.
On Future Trends
Each department must find its own way based on its particular needs and resources, and Waninger encourages intelligent experimentation and targeted initiatives, suggesting others be willing to try something different if existing solutions will not work. “Each organization has to define what service-related activities will add the most value, and focus on those,” Waninger says.
She sees some departments now tackling home-use medical equipment and expects the trend to increase as the population continues to age. “It is another potential drain on resources but also a potential cost avoidance. Currently, we are paying the durable medical equipment vendor to do that work, but it is something that we have the resources and knowledge to take on ourselves,” Waninger says.
In addition, clinical engineering departments are seeing inventories, particularly of technologically advanced equipment, expand in nonhospital settings, such as outpatient surgery centers, imaging centers, and rapid response clinics. “Because the biomedical technicians are often employees of the hospital, it’s been difficult to determine the scope of service in these areas,” Waninger says.

Kelly Robinson, Matt Smith, and Karen Waninger (left to right) plan the initial inventory sweep at a new site of service.
On Evidence-Based Management
With a need to provide value—and a desire to help where needed—departments often absorb these new responsibilities. As inventories grow (but resources remain restricted), new approaches have been mandatory, and department managers everywhere have learned to maximize existing tools and technicians to maintain quality and service.
Having become indispensable to clinical engineering teams, clinical equipment management systems (CEMSs) are now being leveraged by administrators in new ways to compile data useful for decision-making, from equipment history to technician performance to budgetary reports. The increase in information has enabled innovative approaches to traditional challenges.
Many in the industry have embraced the use of analyses to help determine when to replace equipment as well as when to service it; such reports may even provide a hint as to which vendor to select in the future. (For instance, a poor performance history would not support a duplicate purchase.) Busy departments have found they can improve efficiency and expense through evidence-based maintenance strategies that illustrate no negative impact on patient safety or quality of care.
Waninger notes that data from equipment histories has been used to make good decisions about the work that actually has to be done so that value is added. This can take the form of extended device life or improvement in the device applications through the education of its users.
“Achieving these aims on new equipment has more impact on patient outcomes than time spent on electrical safety tests simply because that is what has always been done,” Waninger notes.
On the CMS Clarification Memo
It is this passion for acting in the best interests of the industry—and the patient—that led Waninger to a leadership role in the discussions between representatives of the field and the Centers for Medicare and Medicaid Services (CMS) regarding the government organization’s December 2011 “clarification” memo on preventive maintenance scheduling and subsequent impact on evidence-based management.
The document was perceived by the field as having reversed the existing practice, calling on hospitals to follow the preventive maintenance schedules set forth by the manufacturers; limiting alternate schedules to certain, noncritical equipment; and effectively extinguishing most evidence-based efforts. Naturally, the move raised some concern, and two of the industry’s largest associations, AAMI and the American Society for Healthcare Engineering (ASHE), pulled together with The Joint Commission to engage CMS in a discussion on the decision.
The group tasked with presenting to CMS compiled more than 200 pages of supporting documentation that was submitted by AAMI, and although the government institution has not yet rendered a new decision, it is reconsidering the original clarification memo.
“It is my understanding that some allowances have been authorized. For example, The Joint Commission continues to utilize their survey approach that embraces evidence-based maintenance strategies,” Waninger says. But the industry awaits the decision with great anticipation.
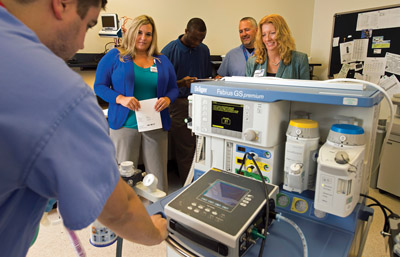
Jared Graff passes along insights from a recent anesthesia service training course to Kelly Robinson, Julius Obazee, Matt Smith, and Karen Waninger.
On Industry Standardization
However CMS rules, the incident has served to highlight HTM’s need to address guidelines. “In addition to equipment management standards, it is important for our future success and recognition that we adopt some minimum standards on things like position descriptions, employee qualifications, credentialing, and performance expectations,” Waninger says.
In the past year, progress toward this end has been made. An updated version of EQ56 (ANSI/AAMI EQ56: 2013, Recommended practice for a medical equipment management program) was released a few months ago “in alignment with the direction the profession is moving,” Waninger says. In addition, the EQ89 Standards Committee has made great strides toward the development of an equipment management standard that will bring the various methods used by departments more in line with one another. (The group met most recently in June at AAMI’s annual convention.)
“It is the intent of this standard [EQ89] to address processes that are applicable to the management of all types of medical equipment. The final result should serve to demonstrate to CMS and to manufacturers that a consistent and logical approach for service decisions, based on collected historical data, after the equipment has been in the clinical care environment, is the best approach for establishing appropriate maintenance activities,” Waninger says.
On Associating with Associations
Of course, for such a broad effort to be successful, it must integrate a lot of perspectives, and so the current EQ89 committee has brought together AAMI, ASHE, and the ECRI Institute as well as representatives from accountable care organizations and other interested professional groups. Though it is often associations that lead large-scale efforts to produce or respond to change in the industry, they do rely on the work and opinion of its professionals.
“In recent years, there has been renewed effort by AAMI to represent the interests of our front-line service professionals when there are any major areas of concern that affect us all,” Waninger says, citing the CMS memo and standards development as just two examples.
A long-term volunteer herself, Waninger encourages others to get involved with regional societies and organizations. “It’s good to exchange ideas, whether through presentations, roundtable discussions, or articles. Anything to share knowledge across this profession will help us become more unified and standardized,” Waninger says.
In addition to her work on the CMS committee, Waninger is also a member of the AAMI Technology Management Council. “It has been a great experience, allowing me to get more directly involved with addressing some of the significant issues that are of concern to the members of this profession,” Waninger says.
Her experience as part of the follow-up to Future Forum I (FF I), a special-purpose meeting convened by AAMI in April 2011, brought her to the various corners of the country explaining the results of the initiative. The work increased her understanding of the questions, reservations, and concerns surrounding the selection at FF I of the term Healthcare Technology Management (HTM) as a new identity for the field.
“All of those conversations and interactions made it even more obvious that we must become unified if we are to be recognized and respected by the general public, the students who will become the future professionals, and the administrators who will ultimately decide the outcome of those of us who are in the profession now,” Waninger says.
On Tackling Technology
Some of the more pressing issues were addressed in the Future Forum II, or FF II, which followed FF I in June 2012. It developed a broad series of steps to further advance the field that included the need for uniform job titles and descriptions. Agreement was not achieved on all specifics, but participants did concur that a lack of consistency can undermine efforts to win broader recognition for HTM professionals.
The group also readily agreed that clinical engineering departments—or HTM departments, to use the new advocated terminology—should embrace collaboration with information technology (IT) counterparts. Tools suggested included service agreements defining each partner’s scope of service for converging technologies as well as standards to help define specific responsibilities.
Ultimately, biomedical technicians will need to acquire some IT skills, but they do not necessarily need to be IT technicians. Many have expanded their scope of network knowledge, and the percentage accumulating related certification continues to grow. Currently, a core curriculum team, with several participants from FF I and FF II, is working on standardization of education programs for people who will enter the profession in the future.
Today, technology education remains a personal decision for every engineer and technician in the field. “I don’t believe formal schooling is a requirement, but I am a strong proponent of continuing education, whether [pursued] formally or informally. People know how they learn, and if they’re able to learn by being engaged in projects and tackling new challenges, new equipment, and new technology as presented within their facilities, then formal schooling on these topics could be unnecessary,” Waninger says.
On Leadership and Experience
Whether in a seminar or on the job, Waninger is always learning, joking that if she finds herself done with learning, it had better be because she is dead. At the same time, she enjoys sharing what knowledge or experience she can offer with others, stating, “If we help those around us improve their individual skills, the collective skills of our profession will grow at the same time.”
Waninger offers thanks to one of her mentors, Professor Glenn Blackwell, who helped direct her to an internship with the clinical engineering team at St Elizabeth Hospital in Lafayette, Indiana, while completing her BS degree in Electrical Technology at Purdue University (also in Lafayette). “I was fascinated with everything about this profession and immediately chose to make it my career,” Waninger says.
Her internship became a part-time position, then a full-time job as a technician followed by promotion to a supervisor role. From there, she changed organizations to be able to continue to grow in her career and eventually began volunteering with professional associations, such as AAMI and the Indiana Biomedical Society. She also found time to complete an MBA.
“I believe my background as a technician, combined with the education and the broad range of experiences over the years, gives me an advantage as a leader. I can still relate to most of the day-to-day service challenges our profession experiences. At the same time, I can understand the broader challenges that health care organizations are facing,” Waninger says.
Others agree. Carol Davis-Smith, vice president of clinical technology at Kaiser Foundation Health Plan in Oakland, Calif, praised Waninger in a release regarding her recent AAMI recognition, stating, “Over the years, we’ve watched Karen demonstrate not just great HTM leadership but great leadership in general.”

Taking advantage of the system being opened up for a tube replacement, the team gets to see inside the CT Scanner. Front Row (L-R): Nathan Matthews, Matt Smith, Jared Graff Standing (L-R): Brent Milam, Kelly Robinson, Jennifer Nickels, Julius Obazee, Karen Waninger Inside the Gantry (L-R): Mike Smith, Russell Snow, David Sanders.
On Reaping What You Sow
AAMI made it official by honoring Waninger as its 2013 HTM Leader of the Year. Formally announced at the association’s annual convention held earlier this summer, the award is intended to recognize individual excellence, achievement, and leadership in the HTM profession.
Criteria include an extensive record of accomplishment, significant contributions to industry-relevant issues, evidence of commitment (through publication, presentations, or participation on committees), industry promotion, involvement in a standards-development process (whether institution- or facility-based), contributions to AAMI, and (no surprise here) leadership roles.
Her lifetime of work in the field as well as with AAMI, particularly her efforts taking the reins to successfully reopen discussion on the CMS’ clarification memo, garnered attention in a year filled with change. For her part, Waninger was honored to speak on the profession’s behalf.
“I am committed to continue to work on this [CMS] issue until it is resolved in a way that allows our health care service professionals to spend their limited resources—money, time, and energy—in ways that add value to their organizations and contribute to positive outcomes for the patients we serve,” Waninger says.
In general, she is always willing to speak for the field and the value it brings to the health care environment. At the same time, she advocates that people within the profession continue to be open-minded, with an eye toward what is needed rather than what has always been done in the past.
She particularly encourages greater unity through standardization “as opposed to the idea that every organization is different so every individual can do things in his or her own way.” In this way, HTM professionals can help to shape their future, Waninger believes, aptly stating, “We are still a young profession within the realm of health care. We have the opportunity to begin now to plant the seeds that will result in the next generation.” 24×7 September 2013
Renee Diiulio is a contributing writer for 24×7. For more information, contact [email protected].






