
James Jernigan
Determining the right staffing model for a hospital’s clinical engineering department is a difficult undertaking, but it is crucial for maintaining the integrity of your biomedical, radiology, laboratory, and IT equipment. Plus, it may save your organization thousands of dollars.
The most common method of determining clinical engineering full-time equivalents (FTEs) involves an estimate of the number of FTEs needed per licensed bed. This method falters when applied to the various clinical engineering environments and service levels at health care facilities. For example, two sites with the same number of licensed beds, but with a very different scope of emergency or specialty services, will have very different needs. Organizations have tried improving this method by expanding the number of FTEs-per-bed estimate by applying a weighted factor based on the type of department serviced. For example, ICU beds require more attention than med/surg beds, so additional FTEs should be required in a department that supports ICU beds compared to a department that supports only med/surg beds.
Another traditional method estimates that one FTE is needed for every 1,500 low-end biomedical devices—little use to a department that services high-end devices. Just as clinical engineering departments vary in scope and size, so do the other departments that clinical engineering supports. This is why FTE estimates based on beds and department type are far too inaccurate to be used effectively. The key to a successful FTE staffing model is to characterize the scope and size of a clinical engineering department in an accurate manner using the information found in most computerized maintenance management systems (CMMS). Since accreditation standards require a full inventory of medical equipment and a history of service for that equipment, this data can form the basis of an improved staffing model. The inventory size will reflect both the size of the hospital and the type of patient services offered. Many CMMS databases contain multiple classifications of equipment, such as a risk factor or equipment modality, that can be used to improve the accuracy and usefulness of an FTE model. This clinical engineering database of medical devices and work orders is the key to building a useful FTE model. Using the CMMS database to create a new FTE model based on actual medical devices serviced enables the earlier estimates for number of FTEs per bed, or total number of medical devices per FTE, to be expanded into more useful categories.
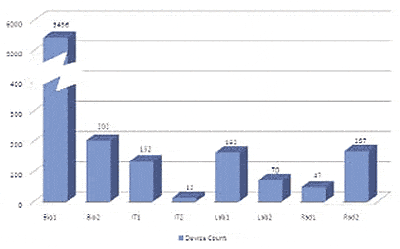
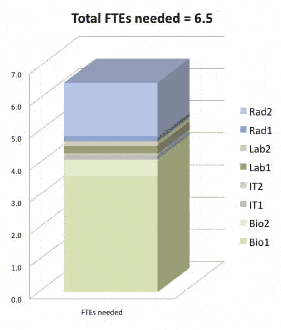
For the purposes of this article, we’ll assume the inventoried medical equipment can be categorized into four groups: biomedical (Bio), radiology (Rad), laboratory (Lab), and IT devices. We’ll further assume that additional device detail is available to subcategorize each of these groups into high-end or low-end groups in accordance with the complexity of its service needs. This method results in eight categories, which can be abbreviated Bio1, Bio2, Rad1, Rad2, Lab1, Lab2, IT1, and IT2. While many CMMS can easily break out an inventory by the radiology and biomed modalities, you may need additional customization or input to classify all devices into those eight modality and complexity-specific categories. For improved accuracy, the new FTE model should adjust for or exclude devices with full service contracts and should also include travel hours required between facilities. Through evaluating the best practices of specific technicians or sites, you may add efficiency-level expectations based on prior performance data (such as average hours per PM or repair by device). You can then set targets indicating how many devices one FTE can be expected to service at your desired level of efficiency. For example, a rough estimate could be 1,500 low-end biomed (Bio1) devices per FTE, 400 high-end biomed (Bio2) devices, 300 Rad1, 100 Rad2, 700 Lab1, 500 Lab2, etc. Multiplying the device counts in each category from the inventory by the device targets per FTE will yield a total number of FTEs needed for the facility.
A slightly more complex version of this new FTE model has been tested and verified at the facilities managed by my employer, TriMedx, and has yielded actionable information for sites with departments ranging in size from one to more than 30 technicians.
After you complete a full analysis, you’ll find that significant savings are possible for both overstaffed and understaffed sites. For overstaffed sites, recalibrating the expectations for the department’s efficiency and decreasing overhead costs will drive savings directly to the bottom line. Savings are also possible for understaffed sites when the root cause for having too few FTEs turns out to be an over-reliance on full service contracts and expensive hourly rates paid to bring additional support on-site temporarily. You will likely find that having this data and process to show and quantify the need for additional staff will make the justification of new positions much easier. This new FTE model will allow you to scale the department to an appropriate size to meet your organization’s specific service requirements, while still driving for efficiency and savings.
James Jernigan has more than 15 years of experience in clinical engineering and is the director of national field service, training and technology for TriMedx, Indianapolis, a medical equipment management company and consulting firm. For more information, contact .
What’s on Your Mind?Got a gripe? A recommendation? Does someone or something deserve praise? Share your opinions and insights with your peers. Soapbox columns should be 850 to 900 words in length and can be e-mailed to . |




