
By Renee Diiulio
Beloved author Dr Seuss wrote, “A person’s a person, no matter how small.” Were Dr Seuss a real doctor, he may have instead penned, “A patient’s a patient, no matter how small.” It’s an unspoken motto at children’s hospitals everywhere, and Arkansas Children’s Hospital in Little Rock is no different.
At ACH, many of the patients are, naturally, small. The 370-bed facility offers tertiary and regional referral care to children from every county in the state (and those in some nearby states as well).
Pediatric patient care offers some unique rewards and challenges, including the special focus and determination that pulls together the medical community when asked to save a child. So it goes without saying that patient health care is the first concern of the entire staff of ACH. But in an interesting twist, the clinical engineering department has found that a focus on some cold, hard numbers has helped to “warm up” patient care—through improvements in performance, customer service, and spend.
Some of those numbers are designed to be specific quality metrics, providing a picture of performance; and some are calculations meant to get the most value from the dollars the facility and the department spend, identifying areas where money has been or could be saved (such as in the area of acquisitions and contracting).
 |
|
Kevin Haralson, director of clinical engineering at Arkansas Children’s Hospital. |
“Our industry has been at a loss to pick one unit of measure that can judge the quality of the work we do, so we incorporate financial measures, productivity metrics, and other factors into our scoring,” says Kevin Haralson, director of the department.
There is a lot of number crunching, but much is handled within the clinical engineering’s database. In an effort to expand analytical and functional capabilities, the department is preparing for an upgrade to the system. Installed in 2003, it now seems “antiquated,” but the new software will offer greater flexibility in creating more useful reports.
The step follows a revision of clinical engineering’s workflow process—again based on numbers—and is expected to continue to streamline workflow. The results of the first phase of the initiative garnered the department an Association for the Advancement of Medical Instrumentation (AAMI) Best Practices Award for its in-house quality management program.
Industry recognition, however, has not been the only reward. Since the department has started doing the math, it has found that combining the right numbers also yields significant “dollars and sense.”
How Do You Measure That?
The inspiration to measure came from the organization’s previous CEO, who, during a meeting years ago, asked the department heads, “What types of metrics do you use to judge your department’s performance?” Few had an answer, but many started thinking about it. That was when the ACH team discovered the gap existing in metrics for clinical engineering.
Their AAMI honor, awarded in 2010, was based on the industry association’s process of dividing total budget by assets to arrive at a cost for maintenance. The national average is 4.7%; ACH operates at roughly 4.1%, an impressive number for a 13-member team that manages 11,765 devices (valued at roughly $90 million).
By looking at how much budget is spent to maintain asset value, the measure makes for an excellent productivity metric and is used by ACH for its own quality management program as well. “But we also want to specifically capture quality to be sure it doesn’t suffer in an effort to drive productivity or financial performance, so we incorporate other factors into the entire score,” Haralson says.
The measures are familiar to most biomeds, consisting of metrics such as turnaround time, bench maintenance, repeat repairs, average age of work orders, PM statistics, and training. “We looked at what we did and how we could put value to it so that it could be scored to indicate performance,” says Bob Crider, CBET, biomed/radiology technician III.
Leaner and Nicer
Once metrics were in place, the team found it had a way to measure the results of quality initiatives and began setting about boosting its performance across the board. Inspired by the improvements achieved in the clinical laboratories, clinical engineering took a look at its own workflow through a Lean and Six Sigma lens.
 |
| Kevin Haralson confers with Lance Woods. |
Working with the same approach, the labs had transitioned to single-piece flow from batch-flow testing, which they had found led to long turnaround times and difficulty finding samples midflow, states Boyd Hutchins, CBET, biomed/radiology technician III. Clinical engineering had been operating with a similar batch system, acquiring, opening work orders for, repairing, and delivering equipment in batches—and the system had similar issues.
“The last customer or customers to give us a device were thrilled with the service, but the first customers generally had to wait much longer to get their equipment back,” Hutchins says. Batching of work orders also made it difficult to define turnaround time or downtime since it was unknown how much earlier the first pieces had been delivered.
Following in the laboratories’ footsteps, clinical engineering also switched to single-piece workflow. Today, a piece of equipment comes in, is assigned to a staff member, and is repaired, documented, and delivered before the technician begins work on another device. “So every customer gets the same turnaround time,” Hutchins says.
The result has been, not surprisingly, more satisfied clients. In the past, a department could send an electronic thermometer in for repair and have it sit on a shelf until five or six others had been collected so they could be processed at all once. “Now we’ll receive an item and turn it around within a day, and customers are happy,” Hutchins says.
The change in workflow was not a difficult adjustment for the team, but they do walk around more. And while the travel is not always the most convenient, it offers the benefit of relationship building with customers (along with a little exercise).
Number Crunching
The stronger relationships have been helpful in gaining the trust of departments as clinical engineering has taken on a bigger role in acquisitions, and those relationships will be helpful as that role continues to grow moving forward. Administration has found that including the biomed team early in the procurement process can lead to savings, not only in the immediate transaction but also down the road.
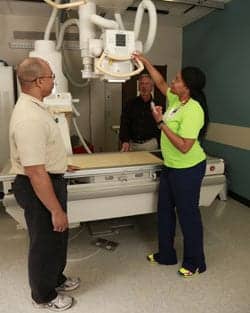 |
| Radiology technologist Kendra Christian explains a table brake issue to technicians Vince Partman and Wally Davis. |
There are the usual savings that come from biomed participation. “We’ll make sure the service manual is included and can often get training incorporated at no additional cost—if we get involved while negotiations are still under way,” Haralson says.
The team, however, also strives to make contracting decisions that maximize the organization’s resources. Vendor service does not necessarily need to be all or nothing, and many clinical engineering departments already implement shared-service agreements in some equipment areas, but Haralson believes (and has shown) that other “in-between” options can lead to extreme savings.
The way to maximize these savings is, of course, by doing the math—and knowing some history. The team tracks service calls in its database as if they were billable from the moment the equipment arrives at the hospital, whether the service is warranty, contract, or time and materials.
“If the equipment is covered under warranty or the vendor is performing all of the work [through a full-service contract], we still document the monetary value provided by the service report so we can evaluate how well that piece of equipment performs and what it would have cost us [for service and maintenance] if the device had not been under contract or covered by warranty—which gives us real numbers to work with,” Crider says.
So if a contract will cost $100,000, but the math shows that actual service delivered runs at about $8,000, $20,000, or even $80,000, ACH can save money by dropping the contract. “The analysis helps us to decide whether to cover something with a contract or not, and if not, we can predict, to an extent, what service will cost us and how much wiggle room we have for unexpected repairs,” Crider says.
It also puts the facility in a better negotiating position. “Vendors are more willing to offer a discount—or maybe give up the expected percentage increase—when you don’t want to sign a contract,” Haralson says.
Competition also helps with negotiations, although Hutchins notes any vendor’s biggest competitor is the ACH clinical engineering team itself. “We make it clear that manufacturers are competing against us because we can do what they can do—even if, behind the scenes, we might not be so sure,” Hutchins says.
Of course, there are other factors to consider outside of cost, such as in-house skill or uptime. “Keeping the equipment healthy and available for use by the customer is the primary goal. The second is to determine the most financially advantageous way to maximize equipment performance,” Haralson says.
Devices that are critical for care or impractical to service (such as those that require special test equipment) are kept on contract, either full or shared. Whenever possible, the team takes on at least first-call responsibility. “We do have some contracts on high-end lab and radiology equipment as well as a couple of other equipment types,” Haralson says.
Extrapolation
The bigger challenge in procurement is associated with long-term planning. Moving forward, ACH clinical engineering plans to implement an annual review of the facility’s equipment inventory so there is always a current list to refer to throughout a project, particularly one involving construction.
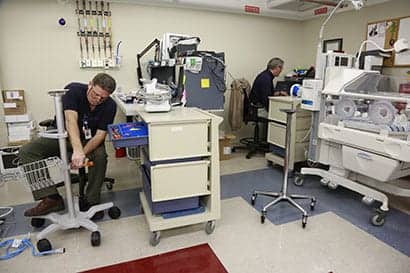 |
|
Bill Adney, left, repairs a noninvasive blood pressure stand while Bill Zilk |
Last summer, ACH opened a new patient tower that added 54 beds, 56 exam rooms, and 19 procedural/diagnostics rooms. Planning for that tower began 5 years earlier. In between, a lot of new devices were released.
“Things change so fast that what was planned 6 years ago may not be the same as what would be planned today,” Haralson says. Because equipment isn’t actually ordered until roughly 3 months before patients are moved in, the organization avoided having to forgo technological advances or lose money on new-but-antiquated equipment, but they did encounter other snags.
For instance, when the planned monitoring technology changed, it was not a problem acquisitions-wise as nothing had been purchased yet. However, the team had planned for one network drop and would instead need two, which they discovered too late to solve with a design change. “It was a little impactful, but we found a solution,” Haralson says.
The team was able to obtain an extra drop from IT, who donated one of theirs. The two departments share a network closet, making the exchange easy. “We were able to gain a drop without having to run more wire,” Haralson says.
Biomed also worked with IT to determine why their redundant pathway connecting the new patient tower’s monitoring network was not functioning properly. “We learned that we shouldn’t have two pathways to the new tower active at the same time, and with that lesson, we learned about ‘network storms.’ We also learned that we needed to start getting educated about networks,” Crider says.
Fortunately, administration strongly supports education, and the team is slowly acquiring knowledge through coursework and certifications. Aaronda McNair, biomed/radiology technician III, is the first in the department to become A+ Certified and has found the result to be well worth the effort. “Today’s equipment is mostly computer-based, and IT staff have their own language. The course definitely helped me understand the lingo and acronyms so I can speak to them and understand what they are saying,” McNair says.
The knowledge is especially useful as the ACH clinical engineering team is currently tackling not one, not two, but three EMR projects. One targets the enterprise EMR, the second impacts anesthesiology, and the third is in alarm management. The work is an intricate process involving multiple devices, connections, formats, and teams, but the clinical engineering department will likely implement a few innovative solutions.
Exponential Effort
In general, they take on a can-do attitude, a particular benefit for any pediatric facility. Author Fran Lebowitz said, “Even when freshly washed and relieved of all obvious confections, children tend to be sticky.” Similarly, even when they want to cooperate, things can get, well, sticky.
Young children can’t sit still, they often can’t understand direction, and sometimes, they haven’t yet learned how to speak. Plus, they are small, and most medical equipment is designed for adults. So, occasionally, clinical engineering is called upon to “make something work.”
For instance, in audiology, clinicians are challenged to find a way for infants and small children to identify that they are hearing a noise. (Adults are simply asked to raise their corresponding hand.) As a solution, the industry developed visual reinforcement audiology (VRA), which incorporates corresponding lights, toys, and/or images to train the pediatric patient to respond (much like Pavlov’s dogs, Crider suggests). But the ACH audiology department wasn’t happy with the commercial options and turned to clinical engineering instead.
Welcoming the challenge, the biomed department developed a custom VRA box that worked so well, when the audiology department expanded, it opted to have clinical engineering develop more of the devices in-house rather than purchase them from an outside vendor. The decision was motivated in part by the fact that peer references (who had rotated through the hospital) felt ACH already had a solution superior to other options.
In radiology/cardiology, clinical engineering developed a solution for the cath lab’s common cabling problem: “As anyone who has been in an EP [electrophysiology] cath lab knows, there are cables running all over the floor. It’s hazardous and leads to more damage when clinicians step on or trip over them,” Crider says.
So biomed developed a customized connection or control box that sits close to the table and brings together all of the cables that have been run under the floor. “The new design has eliminated a lot of the problems we had been having in those rooms,” Crider says, noting the covered cables improve safety, quality, and cost.
The team has also been asked to develop enterprise-wide solutions and “police” them when necessary. When the pharmacy department sought a solution to ensure that all weights were recorded in kilograms, clinical engineering resolved to purchase kilogram-only scales. Because of clinical engineering’s involvement in acquisitions, this standardization is possible; before their involvement became standard, the occasional improper scale would be ordered and caught upon arrival. (New equipment has always been checked in through biomed.)
“There were some instances where we needed to make some modifications to ensure the scale would not produce any results in pounds, but now we are able to catch it before the purchase is made and explain to the clinician why there are restrictions on certain scales,” Crider says.
Once presented with the facts, few clinicians argue—again, they are all united in their mission to care for pediatric patients. “We are recognized as part of the clinical team, and there is a lot of mutual respect between departments,” says Bill Zilk, CBET, biomed/radiology III.
Respect plays a role in the equation that has yielded such success for the ACH clinical engineering team at the same time that it is one of the intangible and positive by-products of the focus on numbers. In general, the decision to “do the math” has been a boon, helping to improve service, quality, and performance—and giving the department an x-factor. 24×7
Renee Diiulio is a contributing writer for 24×7. For more information, contact [email protected].




