Cardiac output is a simple term for a parameter that is also described as ejection fraction. In the intensive care unit (ICU) setting, cardiac outputs are generally determined by a technique called thermal dilution. This technique was introduced in the mid-1970s, became common in most ICUs in the 1980s, but is used less in 2007 than in the past. Part of the reason for doing fewer cardiac outputs is that other techniques, such as ultrasound and, to some extent, pulse oximetery, provide good indications noninvasively. The key term is “indication,” which is very different from an exact number.
For many years, the only method of getting a cardiac output reading was through the use of the dye dilution technique, also called the Fick method. This involved injecting a dye at an exact rate into a vein using a syringe pump, and then withdrawing blood and the dye from another vein with the other side of the syringe pump. The specially designed syringe pump had two syringes, with one syringe infusing the dye and the other withdrawing the blood mixed with the dye. The amount of dye in the withdrawn sample was measured, and a cardiac output was determined. This could take hours and required a person very good at math, because most of the work was done with a slide rule. Once calculators were introduced in the 1960s, the time required to make the calculations was greatly reduced, but it still took hours.
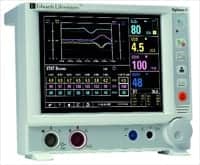 |
| Some monitors present complex hemodynamic data in a simplified way, providing a clearer picture of the patient’s hemodynamic status. |
In the early 1970s, a technique called thermal dilution was introduced. This system used a catheter, inserted into the pulmonary artery, with a thermistor on its tip. Ice water was injected into a port of the catheter that opened in the right ventricle. The temperature change of the blood, measured by the thermistor in the pulmonary artery, determined the cardiac output. Since the body is a closed system, what is pumped by the right heart reflects what is pumped by the left heart. Some engineers were able to come up with the algorithm, and it is still used to derive the liters-per-minute output. If the output is 80cc per contraction, and the heart rate is 72 beats per minute, the cardiac output would be 5.76 liters per minute. This number/method should not be confused with the ejection fraction number discussed later in this article.
For many years, there were problems with keeping the injection water cold, and as computing power increased, with size decreasing, engineers were able to develop measurements that did not require ice water. This technology advance increased the usage of cardiac output in ICU settings.
Service Tips
- In most cases the cardiac output computer is a module in the patient monitor, not a separate box.
- Before doing a cardiac output, flush the pulmonary artery pressure line to make sure the tip is open and there are no obstructions in the line. If the waveform is severely damped, it is an indication of a blockage in the line.
- Injecting water at room temperature into the line must be done quickly and smoothly to get a good reading. If injected too slowly, the cardiac output reading will be low. If it is not a smooth injection, the computer may flash an error code.
- Most suppliers of cardiac output catheters provide the hospital with a little test fixture to check the computer/module. Make sure you have one. To use the test fixture, disconnect the connector from the cable and plug the test fixture into the cable, then hit the switch on the test fixture and the computer/module will give you a reading.
- Sometimes, even if the pulmonary artery pressure line is properly positioned, a reading may be inaccurate. Usually, an indication of position problems is a wide variance in the numbers.
- If you are getting catheter faults, it is usually a problem with the catheter, and the physician should replace it.
Ejection Fraction
The output of the left ventricle is generally referred to as the ejection fraction. An ejection fraction of 55% to 75% is considered normal, meaning that with each contraction, the left ventricle pushes out 55% to 75% of the blood it contains. The lower the ejection fraction, the greater the patient’s problems become—shortness of breath, enlarged heart, and fluid retention—which represent significant risk factors for a heart attack. In some cases, pacers or pacer/defibrillators are implanted to keep the patient alive. Higher than normal ejection fractions may indicate hypertrophic cardiomyopathy, which is basically the narrowing of the left ventricle due to increased muscle or stiffening of the muscle. Strange as it may seem, the symptoms for both high and low ejection fractions are the same: shortness of breath, fatigue, and fluid retention.
Ejection fraction diagnostics is usually done using ultrasound, but other methods can be used, including multiple gated acquisition scan, cardiac catheterization, single photon emission computed tomography, and MRI.
In clinical settings it is not uncommon for pulse oximeter readings to be used as an indicator that there is a problem with either the cardiac output of the right ventricle or the ejection fraction of the left ventricle. If the numbers are consistently low, physicians will generally order more specific tests such as ultrasound. (As a side note, the pulse oximeter was originally developed and tested as a noninvasive method of determining cardiac output. Sometimes, the unintended or side effect of a product eventually becomes its prime purpose. This is much less common with medical equipment than with drugs, because device engineers design specific functions, but drug developers work by asking themselves, “What happens when we do this?” Others might describe it as the “oops” method of product creation.)
You may have noticed that this column has been missing for a few issues, which is because I had some cardiac problems and was laid up for several months. Now I am back, and more columns will follow.
David Harrington, PhD, is director of staff development and training at Technology in Medicine (TiM), Holliston, Mass, and a member of 24×7’s editorial advisory board. Richard Lee is account manager, TiM, MetroWest Medical Center, Framingham and Natick, Mass. For more information, contact .