Ultrasound, a noninvasive, nonionizing diagnostic and therapeutic tool that uses sound waves to generate an image, is widely used in today’s hospital environment in such disciplines as OB/GYN and cardiology to detect heart and valve deficiencies; when coupled with Doppler mode for vascular diagnosis; and in general to detect liver, pancreas, kidney, and gallbladder conditions.
The ever-increasing demand for higher-quality imaging from ultrasound scanners with 3D/4D imaging has meant more complex circuitry and software in the scanners. The result is increased purchase costs and financial burdens on institutions’ operating and maintenance budgets. The problem is how to maximize the investment in these devices, and especially how to ensure that they run efficiently and smoothly with a minimum of costly service interruptions.
Today, when hospitals make ultrasound purchasing decisions they look at the total cost of ownership, including parts and service and license fees, according to Tom Stanfield, BBA, CRES, director of clinical engineering, Parkland Health & Hospital System, Dallas.
Minimizing service costs on any medical device is particularly important because the cost—or savings—of servicing is eventually passed on to patients, according to Mark Waeltermann, senior diagnostic imaging engineer specializing in ultrasound for SSM Integrated Health Technologies, St Louis.
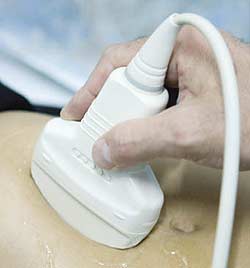
Transducers, which are easily damaged, can cost $50,000 apiece and are the components that most often need replacement.
A well-run in-house service department plays a vital role in controlling service costs, and utilizing a blend of service options may best meet a facility’s needs. Approaches include full service contracts with original equipment manufacturers (OEMs), the use of third-party vendors, and/or the use of in-house technicians.
Service Options
The kind of service arrangement a hospital makes for ultrasound equipment service depends on the type and the amount of equipment it owns, according to Ben Benesby, director, biomedical engineering department, Cooper University Hospital, Camden, NJ. There is not a one-size-fits-all solution; it has to be tailored to the particular situation.
“Cooper owns about 70 systems made by multiple OEMs,” Benesby says. “Often, our physicians will buy what they feel comfortable with, and they don’t always get our blessings.”
According to Zhan Kiselev, senior technician, Cooper University Hospital, ultrasound machines typically cost around $60,000, with high-end machines costing as much as $250,000. Choosing whether or not to purchase a service contract can be a gamble on whether a hospital will save money or end up paying above the service contract cost, and sometimes you can get burned.
Benesby says that happened recently with one of their ultrasound machines where service ended up costing more than $40,000 for a service call. In that case, a contract would have cost $15,000 or $16,000 and would have been preferable. Overall, he says that in-house servicing still provides a large savings, especially when multiple systems are involved. He advises that you can always change plans, constantly question, and readjust whether you made the right call. He advises that the key to making educated decisions is to keep a good record of repairs, which enables a department to pick and choose the plan for each machine based on the individual repair history.
In general, ultrasound equipment is expected to last 5 to 7 years before problems set in. Plus, the computer is obsolete within about 3 years and must be regularly updated.
Equipment longevity, as well as where a product is in its life span, varies from one OEM to another, according to Chris Porath, radiological service engineer for ultrasound at Parkland Hospital. For instance, a 4-year-old model will have had revisions and should have no major service issues, while newer models can have manufacturing or repair issues until any bugs are worked out.
Under Contract
If there is only one piece of equipment, it may be best to put it under a service contract, according to Stanfield. For years, Parkland did not have enough equipment to bring service in-house, but since Parkland now uses upward of 75 ultrasound units, it became more cost-effective to send its techs to OEM training.
In a recent scenario, Benesby shares that based on one physician’s choice the hospital purchased two ultrasound machines of a certain brand that were fairly new on the market and the only ones of that make in Cooper’s system. “We bought a service contract because the machines were not user-friendly for servicing and, according to the service manual, the whole system had to be taken apart for even a simple thing like cleaning the air filters,” he says.
As it turns out, the service contract was well worth it because the systems had multiple failures during the first year of the warranty. Having a service contract enabled Cooper to negotiate for two new replacement ultrasound machines, since the OEM realized that the existing ones were requiring too many costly repairs.
In general, Benesby recommends against buying service contracts from OEMs, which can cost between $12,000 and $20,000 per machine, because the equipment is relatively reliable. But probes, which are easily damaged, can cost between $4,000 and about $90,000 each. Not buying a service contract does carry risks, but many third-party vendors will service ultrasound probes for as much as 50% less than OEMs.
Porath has found that, “OEMs are recognizing that they’re losing revenue to third-party providers, so their pricing is becoming more competitive.”
The In-House Option
For some clinical/biomedical engineering departments, in-house service has become an option to help contain costs by limiting the use of OEMs, not only in ultrasound but also in other modalities.
“Rarely do we call the manufacturer for service,” Waeltermann says. “Last year I saved $400,000 in parts alone in comparison to manufacturer pricing, and I only service roughly 70% of our equipment. Ten to 15 years ago, end users thought they had to have manufacturers service the equipment they made, but end users are more educated now and third-party vendors fix manufacturers’ parts themselves. We have the ability to respond faster and dedicate more time to our customers because we are on-site.”
According to Benesby, in-house repair will result in an increase in the uptime of the machines as it may take an OEM a full day to respond for service. In-house biomeds may initially feel apprehensive about the technology, which is becoming more complex, Benesby notes, but with training and as they become familiar with the devices the apprehension gradually goes away and efficiency increases.
Even if a facility has a service contract for the equipment, it still helps to have an in-house biomed perform a first call or work with the vendor on a service call. According to Benesby, taking the first call—having clinical/biomedical engineering respond first to a service call—is a good cost-cutting measure. At Cooper, Kiselev has become more independent and now rarely needs to call a vendor for help. Kiselev also works closely with clinicians on the floor, which contributes to understanding the clinical side of medical ultrasound.
Gene Amodei, senior technician, Cooper University Hospital, has been called in many times for problems as simple as replacing power plugs or resetting breakers, so taking the first call is vital for saving time and money. “And in case we are unable to address the problem, we always have vendors for backup if we need them,” he says.
Password Protection
Another problem presented in deciding on a service option concerns proprietary codes. While some manufacturers do provide the necessary software or free access to the service codes that enable third-party vendors or in-house techs access to the equipment in order to service it, others make it available for a price and others do not provide access.
For Cory Schissel, senior diagnostic imaging engineer, SSM Health Care’s St Mary’s Hospital, Madison, Wis, who works on all imaging equipment including ultrasound, CT, and x-ray as well as medical film printers, most ultrasound service challenges involve access to the machines’ diagnostics because most, if not all, machines have some sort of self-testing that is password-protected.
“We have access to basic functions, like changes to the network information for sending images (such as printers), but the useful tools that test the circuit boards and power supplies are not generally accessible to the in-house service technician,” Schissel says.
Waeltermann agrees that because some OEMs lock their customers out of servicing equipment unless the customer buys a contract and the manufacturers’ service codes, buyers should ask about service when purchasing the equipment. Otherwise, it can get very expensive and often, he says, problems do not occur until the warranty runs out.
Waeltermann finds it ironic that in his experience the one manufacturer that does not make its operating software available to the end user also has the most unreliable equipment. He compares manufacturers that lock customers out of servicing their own equipment to auto manufacturers locking the hoods of their cars and not allowing owners to change their own oil. And, as third-party vendors grow, manufacturers are trying harder to keep their arms around their own equipment servicing.
Porath says that one OEM he has dealt with has no restrictions on others servicing its equipment. “But that’s not standard, which is why hospitals have to address the service issue,” he says. “Hospitals must have qualified technicians who are trained to service their ultrasound equipment.”
Standardizing Troubleshooting
When it comes to repairs, Schissel also services other hospitals and clinics in the area, some with only one ultrasound, so timely and complete repair is crucial. When facilities have to cancel and reschedule patients, it reflects negatively on them and on Schissel. “I want them to have confidence in the repair I just made,” he says.
Schissel says the idea that more difficult-to-service units are more unreliable is a judgment call stemming from unfamiliarity with the units. “Each style of ultrasound has its own little difficulties,” Schissel says. “If you are familiar and comfortable with them, they don’t seem as bad.”
“Troubleshooting is a process of elimination,” Waeltermann says. Breaking the system down into major subassemblies and identifying which subassembly is at fault makes the troubleshooting process much easier.
To Waeltermann, all ultrasound equipment is basically the same and troubleshooting is fairly standardized. All devices consist of a few major assemblies:
- Front end (scanner) components (transmitter and receiver), which transmit and receive ultrasound at various frequencies;
- Back end (scan converter), which enhances the images with color, pulse wave, continuous wave, and other image enhancements using the raw data received from the front end;
- A transducer, or probe, which is key; its crystals are rung at a predetermined frequency depending on the application it is used for, and it is the “eyes and ears” of the ultrasound system. It is also the most likely component to fail, typically due to damage;
- The power supply;
- The hard drive, which holds the software;
- A monitor; and
- The user interface (controls, keyboard).
Sometimes, diagnostics will identify the problem. Certain problems display particular characteristics that make it easier to find the source of the problem. The key is narrowing the problem down, and sometimes swapping parts out within the system can help accomplish that. For instance, Waeltermann suggests if the sector image is faulty on the left side, there may be an opportunity to swap board locations in the front end (scanner) to see if the problem moves with the boards and help isolate it.
Stanfield, whose facility is a public hospital with high patient volumes where equipment is heavily utilized, notes that the components that most often need replacement are the transducers, or probes.
For Schissel too, transducers present a problem, and he spends most of his repair money on them. “If a probe is dropped or if there’s normal wear and tear, the probe has to be fixed,” he says. “There is nothing that we can do in-house to repair a damaged probe; it always involves a third party.” Probes, which are easily damaged, can cost $50,000 apiece.
Porath describes portable ultrasound equipment as “no more than specialized laptops with several dedicated circuit boards,” but full-size systems that service entire departments have much more of a hardware component than, say, an emergency department system that deals with “triage and stat look” scenarios.
Hardware-intensive systems include those that require more penetration and greater image quality, detail, and echoing capabilities, according to Stanfield.
Taking Stock
As with any piece of equipment, the more techs work with it, the more problematic parts become evident and can be stocked for quicker repair. Schissel would like to keep more parts on hand but costs limit that, and he notes that a facility might own four of one kind of ultrasound that could include three variations that do not use the same control panel circuit board.
“You can’t have $30,000 in ultrasound parts sitting on a shelf waiting, and you must also weigh the pros and cons of using the OEM or a third party,” Schissel says. “With a third party you run the risk of such defective parts as power supplies and boards; with OEMs you have to pay such a high price for parts that you’re almost embarrassed to pass it on to the customer, and that doesn’t include the hourly rate for service if you have to call the manufacturer in. The rates for service are incredibly high.”
Compatibility of replacement parts can also be an issue, but Waeltermann says quality vendors will ensure compatibility before shipping parts.
When it comes to ultrasound decisions, beginning with the purchase and continuing through to servicing, careful research and attention to the needs of the hospital will guarantee that the demand for high-quality imaging is met at the lowest cost of ownership.
Gary Tufel is a contributing writer for 24×7. For more information, contact .
Considering the Third-Party Option
Finding a quality third-party vendor may take some time, but many biomeds agree that third-party vendors are viable alternatives to OEMs.
“When you compare the cost and quality of the service we provide our customers to that of the manufacturer, my message is to avoid manufacturers,” says Mark Waeltermann, senior diagnostic imaging engineer specializing in ultrasound for SSM Integrated Health Technologies, St Louis. “There are many quality third-party vendors out there. Some vendors won’t even charge if they cannot fix the problem, although that’s rare.”
He advises caution in seeking a third party and suggests turning to clinical engineering departments that have had experience with various third-party vendors and using them as a good referral resource.
Many third-party vendors can provide refurbished or new parts from an OEM at a better price, which can also save money in comparison to the OEM price, according to Ben Benesby, director, biomedical engineering department, Cooper University Hospital, Camden, NJ.
Cory Schissel, senior diagnostic imaging engineer, SSM Health Care’s St Mary’s Hospital, Madison, Wis, suggests finding third parties from co-workers. From there he reviews whether the repair took too long or was overpriced and then makes a judgment call. Schissel has used at least seven or eight different third-party companies in the last few years and has settled on three that he uses regularly—one for most of his transducer repairs, one for circuit boards, and a third in case the first two cannot accommodate him.
Schissel advises biomeds to “know who you’re dealing with, get information about them, and make sure they meet the standards and have the certifications they need to repair parts to industry standards.” He adds that many vendors make it seem as if they are doing in-house repairs and have a stock of parts, but they are really sending equipment elsewhere for repair and charging extra for it.
Schissel suggests using a middleman when searching for a part for an older unit if it may be hard to find. On occasion, he has had to call six or seven third parties to find the part. In these cases he has used a middleman to search, enabling him to continue working on other important projects.
“Be savvy and hook up with good third-party vendors,” Waeltermann says. He does warn that some gouge ultrasound equipment buyers. Waeltermann, who prepares cost-savings reports for SSM on a regular basis, says one such vendor actually charged him more for ultrasound parts than the manufacturer would have.
He adds that when a hospital narrows the source of a problem down to two or three possibilities, some of the better third-party vendors will only charge for the part that solves the problem and will accept a return of the other parts at no charge. Manufacturers also accept returns but charge for restocking. Some third-party service providers charge a flat fee for a repair job no matter how many times they need to come to the facility to work on the problem, but many OEMs charge per trip.
In situations where using a third party seems to be the best service option, Chris Porath, radiological service engineer for ultrasound at Parkland Health & Hospital System, Dallas, recommends using established third-party vendors.
Tom Stanfield, BBA, CRES, director of clinical engineering, Parkland Health & Hospital System, Dallas, suggests that facilities establish a relationship with a vendor and observe that vendor for reliability, quality, and pricing.
—GT





