|
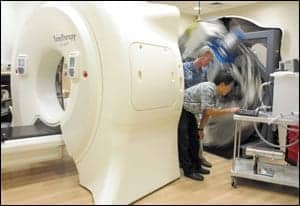
| CCUs have much of the same equipment as general ICUs, in addition to a few more cardiac-centered devices. |
When BMET Steve Erdosy, technical site leader, clinical engineering, Indiana Hospital Community Health Network, Indianapolis, has to troubleshoot something in the hospital’s cardiac intensive care unit, also known as the CCU or CICU, he keeps in mind that the nurses yelling for his attention are not thinking about the electrocardiogram (EKG) or blood pump as much as they are thinking about the patients attached to those devices.
“You have to try to look at it from the nurse or staff perspective,” Erdosy says. “If you’re able to spend time with the staff in their environment, watching them take care of patients and asking them questions, it gives a greater understanding of what they’re thinking and what their workflows are. That helps us to better serve them and, ultimately, the patient.”
For Carol L. Wyatt, CBET, manager for the Heart Hospital Baylor Plano, biomedical technology services at Baylor Health Care Systems, Dallas, the most difficult part of maintaining the CCU equipment can be getting access to the equipment. “It’s the communication and teamwork between the biomed department and the nursing staff that helps with a successful maintenance program,” Wyatt says.
Consequently, the day in the life of a biomed assigned to the CCU involves maintaining not only equipment, but also maintaining good communication with clinicians and fellow IT personnel.
Today’s Cardiac ICUs
Modern cardiac CCUs are isolated rooms rather than multibed wards. George E. Gladding, CBET, at St Francis Hospital and Healthcare Centers, Indianapolis, says, “Today, because of the major risk of disease and infection, hospitals have learned to keep the more critical patients in an isolated room that has a laminar flow system that can control the environment, almost like a bubble. So it keeps everything sterile and the noise down to keep the patient calm and quiet.”
In terms of devices in a typical CCU, biomeds will see much of the same equipment as a general ICU, although with a few more cardiac-centered devices.
“There are a lot of similarities between a normal ICU and a cardiac ICU,” Erdosy says. “In a cardiac ICU, you would typically have intra-aorta balloon pumps, defibrillators, external pacemakers, ventilators, and a continuous cardiac output monitor instead of a cardiac output unit that gives cardiac outputs every once in a while.”
Erdosy also sees critical care devices such as left ventricular assist devices, which some patients may need to partially or completely replace the function of a failing heart.
In both the normal ICU and the cardiac unit, biomeds have responsibilities for many of the same physiological bedside heart monitoring and vital sign monitors that are often integrated into a single display monitor and central processing unit.
Biomeds will also service common portable devices, such as EKGs to measure heart rhythm, intravenous (IV) infusion pumps to administer antibiotics and pain medications, as well as defibrillators that may also be on standby in or near the patient’s ICU room.
Additionally, the patient will generally have a critical care bed equipped with a scale to monitor weight gain or loss, as well as a hypo/hyperthermia blanket to keep body temperature at a steady level.
Aside from equipment itself, biomeds also need to keep an eye on the equipment’s required cables, leads, and communication lines for the various monitoring alarm systems. Ventilator and cardiac alarms link directly to the nurse call systems via phone jacks. Checking these cables for wear and tear constitutes one of the many duties of biomeds on their daily CCU rounds.
Day in the Life of a CCU
While biomeds are responsible for making sure CCU equipment is working and ready to go, performing those regular tasks can be challenging with a busy cardiac unit.
“The difficulty isn’t the maintenance or PM of the equipment, but getting access to the equipment,” Wyatt says. “The biomed department must work with the nursing staff to get access to the equipment. This requires some flexibility by the biomed department.”
“You can’t check every device in every room,” Gladding adds. “When you go into this critical care unit, you’re going to have several rooms that are isolated. That patient is either susceptible to our germs or we’re susceptible to their germs. The only times that you would go into those rooms is when it’s critically needed and the nurses need you in there right away to take a look at something.”
Wyatt cautions biomeds to remember patient contact protocols during those critical situations and to also have consideration for the patient’s family members. “It’s already a stressful situation, and malfunctioning equipment can add to the stress if not handled correctly,” she says. “Common courtesy and respect go a long way in getting the malfunctioning equipment functioning correctly or re-moved from the room.”
Emergencies aside, when Gladding does his regular daily rounds of his CCU, he purposely stops at the nurse’s station. This stop not only allows him to find out what rooms are available, but it also lets clinicians know that he is on the floor and he can find out about any issues. Gladding says he usually goes into two empty rooms per day to perform any scheduled PMs and to check for hints of other problems.
“I’ll look to see if there’s dust building up on something that needs to be looked at,” Gladding says. “I’ll check the modules that go into a rack of connections to the walls, like the alarm connections from the ventilators to the wall connections that go to the nursing stations. I might even hit the alarm buttons and watch the visual alarms, listen for the nurse call—and then walk outside the room to tell the nurses it was me.”
He is also sure to inspect the power cords and cables of all the equipment, especially any bedside cables, where chaotic emergency situations will make clinicians pull the bed away from the wall and break cables that are yanked out of the wall.
Similarly, Gladding sees broken cables from EKG carts that travel from room to room, getting thrown and pushed around, which often pinches cables. When checking an EKG device, Gladding will not only check the battery and make sure the machine powers on, but he will also simulate a test in order to make sure the EKG’s feeding its paper straight and printing correctly. Before ending his rounds, he checks back with the nurses on duty to make sure they do not have any questions about a particular piece of equipment.
“It seems like there’s always a couple of questions on a parameter on how they want to set up their patient monitors,” Gladding says. “That’s another expertise that we’re very good at, because we work with these devices on a daily basis, so we can help them.”
Communicating and Troubleshooting
When troubleshooting failures, both clinicians and biomeds need to effectively talk to one another in order to solve the problem as quickly as possible. From the nurse’s perspective, the equipment is not performing as advertised and she/he just wants it to work or get quickly replaced. From the biomed’s perspective, seemingly simple questions must be asked, such as when the clinician noticed the malfunction, what she/he was doing, and the current setting. Not asking these questions can lead to a full PM and perhaps a half day of work—only to discover that replacing a cable or changing a setting was all that was needed.
Whenever he is speaking over the phone, Erdosy says he tries to be sensitive to what he is hearing in the background to better judge if he is needed immediately. “I can hear what’s going on in the background—a whole bunch of alarms and noise going off—and that lets me judge the stress in a person’s voice if they’re cordial or direct and to the point.”
When Gladding realizes that the problem cannot be solved over the phone, he always grabs the relevant device assimilator and some replacement gear, such as EKG cables, pressure cables, and lead wires. “They just want it fixed, so I’m going to go up there with everything that I have that I know could fix the problem right away,” he says.
Whether an emergency or for a PM visit to the CCU floor, Gladding says it is important to keep the situation calm and to walk in concerned, not only about the equipment, but also about the nurse’s social concern as well.
He says, “I find it a whole lot easier to work in the ICU settings by being their friends. So, every once in a while, I attend their functions outside of work. Even if you show up there for a few minutes, it gives them a sense of friendship and makes it so much easier when I come in there. Then, when the situation is critical, they’re less likely to tense up and not talk to me when I have to ask them questions.”
Erdosy also believes that a biomed’s choice of words is very important. “If there was a switch in the wrong position or a setting that was incorrect, I wouldn’t typically say, ‘Well, you had it in the wrong mode.’ Instead, I would say that the monitor was in the incorrect mode and this is how to change it. So, rather than say ‘you’ to them, putting them on the defensive, it helps them relax a little, and then you can help them understand how to go through and adjust it properly.”
Gladding says that biomeds training in school would greatly benefit from taking some kind of communication class. “Communication is a big thing. Otherwise, you’re going to struggle a lot.”
Tor Valenza is a staff writer for 24×7. For more information, contact .