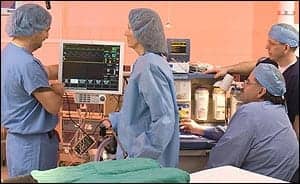
Clinical engineers should acquire the skills and responsibility to be the nerve center of the telehealth team
At Stanford University Medical Center in Palo Alto, Calif, the clinical engineering department pioneered the organization’s path into telehealth, demonstrating it as a viable option. The facility now takes a multi-pronged approach, using telecommunications technology to provide and take advantage of a number of services spanning all disciplines and aspects of medicine.
 At Stanford, Purna Prasad, MS, CCE, director, department of clinical technology and biomedical engineering, works on a system capable of remotely receiving EEGs and corresponding full-motion videos of patients.
At Stanford, Purna Prasad, MS, CCE, director, department of clinical technology and biomedical engineering, works on a system capable of remotely receiving EEGs and corresponding full-motion videos of patients.
When the program was first started, Stanford’s clinical engineers (CEs) had to select and connect the equipment, developing their own systems. Now, as the technology has become more popular, off-the-shelf applications are available. But as new uses evolve, customized devices, connectivity, and/or networking designs may still be necessary. The experts that 24×7 spoke with agreed that CEs should be responsible for the development, operation, and advancement—as well as the care and maintenance—of these systems.
“CEs are telehealth’s nerve center, providing the technology, setting up the interfaces, and making sure the transmission is flawless,” says Purna Prasad, MS, CCE, director, department of clinical technology and biomedical engineering, at Stanford. But to fill that role, CEs will need to expand their skill sets and become a part of the telemedicine health team.
CEs Enable Telehealth Applications
Going beyond telemedicine to encompass aspects such as tele-education and store and forward (see sidebar for definitions), telehealth offers a wealth of applications. At Stanford, telehealth is used to offer monthly expert presentations on the latest advances in various disciplines to areas as far away as Hong Kong, Singapore, and the Philippines; to hold teleconferences where experts share information, whether consulting over a patient’s images and records or transmitting a live surgery; to simulate training remotely, providing direct feeds from equipment, such as endoscopes; and to debrief health care teams on specific treatments.
Telehealth is used in cardiology, dermatology, disease management, electronic medical records for rural health systems, HIV/AIDS, home care, mental health, pharmacy, rehabilitation, school-based services, trauma and emergency care, and radiology, according to Paul Ostrowski, PhD, CCE, chief, biomedical engineering, John D. Dingell VA Medical Center, Detroit.
Yadin David, EdD, PE, CCE, director of the biomedical engineering department at Texas Children’s Hospital, Houston, breaks down telehealth’s applications another way. “Current practices focus on three main areas: patient consultations, for instance second opinions; education, particularly staff but also patient; and administrative activities, such as videoconferencing between remote hospitals.”
New uses are constantly being developed. For instance, Texas Children’s Hospital serves sick children but does not have a delivery suite on-site. The facility wanted to provide a way for mothers, who are patients elsewhere, to see, hear, and speak to their premature or otherwise sick newborns. “A typical telehealth conferencing suite would require too much space and create too much stimulation for premature infants, so we created a mobile unit that rolls to the incubator, uses a camera that works in low light settings, includes a headset and speakers, and is very nurse-friendly,” David says.
To bring the new service online, the team first had to complete device design, device integration, simulated runs to test the equipment, and network monitoring to ensure patient privacy. David’s department managed the process.
CEs Create Telehealth Infrastructure
The devices are often common, such as medical instruments, video cameras, scanners and printers, video displays, interactive audio and video, and interconnecting devices, according to David. But devices are merely one component.
Following device design, there is integration of multiple instruments into a single platform. The whole system must then be tested and validated. The network and platform must be sufficiently robust for the task. Users must be trained. Performance, calibration, and quality need to be ensured, and privacy and confidentiality must be maintained. “How do you do that with multiple devices?” David asks.
David predicts that the integration and closer relationship between the CE and the information technology departments is going to continue. Hospitals can use the various telecommunications methods that are available to them, whether satellite dish, broadband, or phone lines, or some combination of the three. “Most hospitals have the basic infrastructure for telehealth, but they also need to make the right decisions about the equipment,” Ostrowski says. System integration and telecommunications’ ability to link the systems are areas where CEs should play a role, according to David.
CEs on the Telehealth Team
CEs can provide the level of decision-making needed to offer telemedicine. “Much of the cited literature references clinical engineering in an offhand way, often in relation to equipment maintenance. The only concerns seem to be, who will fix it, and within what time frame?” Ostrowski notes. He believes it is a primary mistake of hospitals to not involve CEs at the front end.
 Before putting an independently designed mobile televisitation system to use, Texas Children’s Hospital’s Yadin David, PE, CCE, director of biomedical engineering, thoroughly tests it.
Before putting an independently designed mobile televisitation system to use, Texas Children’s Hospital’s Yadin David, PE, CCE, director of biomedical engineering, thoroughly tests it.
“The CE department can provide a consistent institutional approach to decision-making and instrument acquisition,” Ostrowski says. CEs know the availability and suitability of equipment throughout the facility. And this is not limited to just the computers, monitors, or picture archiving and communication systems (PACS); it also typically includes the end-to-end technology that will be used to transmit data.
Because the technology is new and evolving, clinical engineering’s role has not yet been clearly defined throughout the medical community. At Stanford, where the department has taken a lead role, CEs are part of the telemedicine health care team. The engineer plays as key a role as the physician and nurse. “Technology today is so sophisticated that you need a good engineer to maintain the interfaces and assure continuous data transmission,” Prasad says.
This represents the tremendous opportunity facing CEs today. “CEs need to evolve and lead the change. We need to be involved in creating standards and guidelines. We need to understand the components, including audiovisual and telecommunication system design. We need to capitalize on our ability to work directly with other disciplines around patients,” David says.
| Tele-Semantics “Telemedicine and telehealth are terms being used somewhat interchangeably, but telehealth is more appropriate nomenclature for applications and functions beyond telemedicine,” says Paul Ostrowski, PhD, CCE, chief, biomedical engineering, John D. Dingell VA Medical Center in Detroit. Ostrowski culled the following definitions from the Office for the Advancement of Telehealth, part of the US Department of Health and Human Services, for a 2005 presentation.1
• Telehealth is defined as the use of electronic information and telecommunications technologies to support long-distance clinical health care, patient and professional health-related education, public health, and health administration. Remote training, involving real-time audio, video, and instrument feeds, falls in this category. • Store and forward (S&F) is a type of telehealth encounter or consultation that uses still digital images of a patient for the purpose of rendering a medical opinion or diagnosis. Common types of S&F services include radiology, pathology, dermatology, and wound care. S&F also includes the asynchronous transmission of clinical data, such as blood glucose levels and electrocardiogram measurements, from one site (for example, a patient’s home) to another site (for example, a home health agency, hospital, or clinic). —RD Reference |
CE Telehealth Skill Set
CEs lacking skills in these areas should seek to acquire them, even if they must do so on their own, David stresses. To succeed at telehealth efforts, a CE will need knowledge about the equipment, systems, interconnections, maintenance requirements, risk assessments, care protocols, and provider communications. They will need to take a multidisciplinary approach. And they will need to translate information into layman’s terms to communicate with staff and eliminate patient fears.
“There is a generational difference in reactions to telehealth. Children are generally excited about it, but parents are less comfortable in front of big cameras, lights, microphones, and screens. CEs should be able to alleviate their concerns,” David says.
Other challenges include getting up to speed on telecommunications systems and terminology. “There is a lot of terminology with imaging and telecommunications. CEs should be able to distinguish between, for example, a full T1 line and a half T1 line,” David says.
How do you broadcast from point A to point B? How about point A to multiple points? How do you connect and manage more than four hospitals together at a time? How do you minimize downtime? How do you ensure security? These are all questions that David proposes CEs will have to help answer.
David suggests that CEs—particularly the first wave of practitioners—may need to obtain these skills on their own. Unfortunately, few telemedicine educational opportunities are geared specifically to clinical engineering, so CEs may have to demand workshops while obtaining the necessary information independently, as well as be willing to share their knowledge.
Prasad agrees that telemedicine demands new skills. “Basic CE skills focus on the interface between patient and doctor, bringing the inside of the patient body outside—making it visible to the doctor so a diagnosis can be made,” he says. “Now, we are doing it from a distance.”
“Telemedicine is an important component of the future of medicine, and it can be the answer to many problems that are facing health care today,” Ostrowski says.1 “The practice of telemedicine utilizes technology for many reasons, including increased cost efficiency, reduced transportation expenses, improved patient access to specialists and mental health providers, improved quality of care, and better communication among providers.”
With these benefits, telehealth applications are only expected to expand. Remote surgery lies on the horizon. And on the “bleeding edge,” according to Prasad, are systems that will allow a remote clinician to actually feel a patient. Now that takes nerve. 24×7
Renee Diiulio is a contributing writer for 24×7.
Reference
1. Ostrowski P. Clinical engineering challenges in telemedicine and telehealth. American College of Clinical Engineering teleconference; January 20, 2005.

 • Telemedicine is the use of electronic communication and information technologies to provide or support clinical care at a distance. An example is the remote viewing and reading of radiographs via a picture archiving and communication system (PACS) network and the Internet or telephone lines. “For instance, a hospital might contract with another in a different time zone to cover immediate radiology-reading needs during off hours,” Ostrowski says.
• Telemedicine is the use of electronic communication and information technologies to provide or support clinical care at a distance. An example is the remote viewing and reading of radiographs via a picture archiving and communication system (PACS) network and the Internet or telephone lines. “For instance, a hospital might contract with another in a different time zone to cover immediate radiology-reading needs during off hours,” Ostrowski says.