 |
| Cameras and video have become surgical tools in the operating room, educational tools in the classroom, and diagnostic tools just about everywhere else. |
Just as televisions have become ubiquitous in the home, video systems have become commonplace in medical facilities. But unlike a television, medical cameras and displays are not intended for entertainment. Cameras and video have become surgical tools in the operating room, educational tools in the classroom, and diagnostic tools just about everywhere else.
Subsequently, when a system is not working properly, there is more at stake than a missed episode. A surgical team with a patient on the table cannot wait for a rerun but will often require an immediate fix. Enter the biomedical technician.
“It would be wise to understand and analyze the system before pointing to any particular device because it is a component-driven system,” says Farid Eslami, CCE, CBET, an independent clinical engineer based in Southern California. Many times, Eslami notes, the inexperienced biomed assumes the problem is the camera and proceeds on that presumption.
“They order a camera for $1,000 or $1,500, and it comes 1, 2, or 3 weeks later, and when the biomed puts it in, the system still doesn’t work,” Eslami says. The time and money have been wasted, and the equipment is still not available. “So it’s wise to look at all the components of a system because everything needs to work,” he says.
In some instances, there may not even be a legitimate equipment problem. “You have to be able to determine if you’re having a problem with the video system or if the user is having a problem,” says Thomas Saylor, a biomed technician II with Orlando Health in Orlando, Fla. “A lot of times we find that it is a user problem. They’ll have it on the wrong setting or mode.”
The most efficient troubleshooters will know how the system is used, understand how the components relate to performance, and keep a mental (or written) checklist that helps to narrow the source of the problem.
The Big Picture
Today, video systems are deployed throughout the hospital. “Any department that ends with ‘-ology’ uses digital imaging that requires capture, processing, monitoring, and storage,” Eslami says. Surgical teams, cath labs, and endoscopic suites are increasingly relying on cameras, which can be used to complete the procedure (as in a laparoscopy) or simply to capture it (often for educational purposes).
In some facilities, video has become routine for colonoscopies, bronchial exams, and orthopedic laparoscopic procedures; new applications are constantly in development. At Orlando Health, “they are starting to get into doing bladder and abdominal surgeries and even some hearts,” Saylor says.
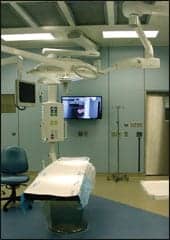 |
| In surgical suites, the cameras are often attached to a scope or controller that may include a zoom. |
Eric Steinbrecher, a biomed technician at St Luke’s Medical Center of Aurora Health Care in Milwaukee, notes that the 50 different operating rooms in the facility have some sort of video system present, and the rooms are in constant use. “As soon as one case ends, they put in another,” Steinbrecher says. This makes swapping systems an ineffective solution when problems arise and puts pressure on the biomed to act quickly.
Those who are most successful at troubleshooting will understand how the system is used. To achieve this, Saylor recommends biomeds sit in on a few of the surgeries, as well as participate in the equipment in-service. His team takes advantage of the hospital’s surgical viewing room to witness operations. “It’s good to watch when things are going smoothly so when we do go in to troubleshoot, we can identify anything out of the ordinary,” Saylor says.
Formal education helps too. Manufacturers may offer training courses, but many biomeds find they teach themselves. Saylor picked up much of his knowledge from the Internet, including information about connectors, cables, and costs.
Get the Picture?
Although analog video systems are gradually being replaced by digital, both are still in use, and biomeds need to know how to troubleshoot the two technologies. Fortunately, the components are the same.
Video systems are typically comprised of a camera, its controller, a light source, digital processor, monitor, recording and storage equipment, output devices (such as a printer), and cables and connectors.
“The workflow of an image goes from the image to the camera to the processing application, where it is processed and then stored on some storage device,” Eslami says.
Today, that storage is often integrated with the hospital database. “Most of these information images will be captured and stored simultaneously by the data in the medical record of each individual,” Eslami says.
In surgical suites, the cameras are often attached to some sort of scope or controller that may include features such as zoom, a manual shutter control option, and settings designed to match use. “These slightly change the color, the light intensity, and the speed of the camera,” Saylor says.
The controller is interfaced with other components through cables and connectors. These need to match the technology within the devices to successfully transmit data in a clear format, but the alphabet soup of technological acronyms can be confusing. “It depends on the application. If you’re using a high-tech video feed, you will tell the difference between VGA and DVI, which is like comparing analog TV to HDTV,” Steinbrecher says.
VGA, or video graphics array, is the old graphics standard for the analog transmission of data from the processor to the monitor. Graphics standards impact the colors and resolution seen on the display; over time, the capabilities in both areas have improved.
“VGA is basically not used anymore unless you have a really old computer,” Saylor says.
VGA was replaced by SVGA, or super video graphics array—also known as UVGA or ultra video graphics array—which supports a minimum resolution of 800 x 600 pixels (VGA supported 640 x 480 pixels). XGA, or extended graphics array, allows screen resolutions of 1024 x 768 pixels or higher; SXGA, or super extended graphics array, permits resolutions of 1280 x 1024 pixels and up; UXGA offers resolutions of 1600 x 1200 pixels or better; and QXGA, or quantum extended graphics array—the most recent improvement—increases resolution to 2048 x 1536 pixels.
Most systems support the VGA and SVGA standards, and these analog connections can serve as backups when digital interfaces (if available on the device) do not work. Today’s digital interface standards include digital video interface (DVI) and high-definition multimedia interface (HDMI). DVI preceded HDMI and is available in three categories: DVI-A, which supports the transmission of digital data to analog devices and is compatible with standards such as VGA and SVGA; DVI-D, which enables digital-to-digital transmissions; and DVD-I, an integrated version that handles both. HDMI adds an audio component.
Currently in medicine, DVI is more common. “There is no need to have an audio component with your video,” Saylor says.
A Clearer Picture
Many facilities are moving to completely digital environments as budgets allow. The benefits of digital technology, which transmits data as binary codes, include easier and more reliable transfer than that offered by analog signals, which can degrade.
“After so many feeds, you will need a repeater [with a digital signal] because the signal gets lost, as with any sort of cable, but it is still a digital signal,” Steinbrecher says. This means that, generally, distortions introduced during transmission are recognized and not reproduced on the receiving end, eliminating errors on delivery and producing a clearer picture.
The greater resolution and color capabilities allowed by the newer technologies improve the images seen by the clinicians on the displays. “We’re able to get bigger pictures so the surgeons can see more and more clearly,” Steinbrecher says.
To maximize viewing, the display must also be able to support the desired resolution. For instance, in the surgical suite or at the radiology workstation, high-resolution devices enable greater viewing detail and therefore procedure precision; other uses can require less detail. For instance, “if monitoring patient vitals, you don’t need much resolution at all,” Steinbrecher says.
Many facilities have purchased LCD or plasma screens to replace CRT monitors. Flat-screen monitors offer advantages over CRTs that include longer life spans, less power consumption, consistent color, and lighter weight.
 |
| Broken fibers in the fiber optic cable and damaged cables can change the quality of the picture. |
“As CRTs fade, you get color loss, whereas LCD devices are just as bright almost the entire time,” Steinbrecher says. “You can also get larger sizes with digital monitors and throw them on booms where nurses and staff can easily move them around.”
If not on a boom, the monitor is often located at the top of a cart containing the rest of the system as well. “The video tower is a box on wheels with several shelves to hold the equipment,” Saylor says.
Not one of these video system components is more important than the other, in part because if any component is not functioning, the image will not be properly captured, processed, or stored, and therefore will not be available for clinical use. Consequently, the entire system must be addressed when problems arise.
Picture Perfect
Saylor will start troubleshooting a video system at the image. “Just looking at the picture will pretty much determine where you are going to look for the problem,” Saylor says. Is the picture dark? Grainy? Distorted? Dull? “If the picture is dull and doesn’t have any contrast but is a fairly good picture, the system may be on the wrong setting,” he says, noting this is a common problem. “The user will have the system set on RGB [red green blue] video when it should be set on DVI or vice versa. Or they’ll have it on S-video when they need it on another mode.”
If the setting is correct and the picture is still bad, Saylor will inspect the camera. Is the lens scratched? Is the camera iris functioning? Is the camera coupled properly? Is the light source working?
“Broken fiber in the fiber optic cable will reduce the amount of light coming into the rigid scope, and therefore the picture will get darker, but we have to determine if we have a bad cable or if the fiber optics in the rigid scope have gone bad,” Saylor says.
If all is well on the camera end, Saylor works backward. Is the cable that runs from the camera to the controller operational? “If you’re getting a lot of snow in the picture, it may be that this cable has been pulled, tugged, or stressed in some way or is going bad,” he says. Cables can be tested with swapping. Does the system work with a different cable, or does the cable work on another system?
If it is functioning, the next possibility is the controller, and if not the controller, then it might be the cables connecting it to the monitor.
“Sometimes, they’ll have a slave monitor—an extra monitor for the doctor working opposite to the lead surgeon to view—which is usually run on a 25-foot or longer cable that can get run over or tugged on hard, and it starts to go bad,” Saylor says. This can produce graininess or introduce an artifact in the image.
The monitor itself may also have a problem, though rarely is this component the issue. Most often the problem is a cable or connector that has been pulled, tugged, or run over one too many times, causing broken pins and/or wires. As a result, some biomeds will check these before even looking at the camera.
As an example, Steinbrecher says, “Today—I got called into a surgical suite, where they were having intermittent video and found one of the connections on the monitor was broken. But I was able to fix it with needle-nose pliers and make a solid connection.”
Preventive maintenance does not often help to eliminate these problems, although operational checks can verify function and possibly catch an issue early. “There’s not much for the maintenance of the video systems,” Eslami says. “Either they work or they break.”
|
See the Buyer’s Guide for video system vendors. |
When broken, problems are dealt with on the spot, and if a component is bad or needs further analysis, it is replaced with a backup until it can be evaluated and repaired. In busy facilities, or those with low inventory, loaners may be used to avoid downtime. Steinbrecher recommends keeping technical support and sales rep contact numbers handy. “Sales reps can be a great help if something is truly broken,” Steinbrecher says.
Generally, Saylor finds that video systems are reliable across the board. “Especially in the digital video areas, they are pretty much equal with each other,” he says. “They’re basically using the same components and the same standards.”
The similarities among the systems can help a biomed manage them better, since there is typically more than one type of video system in a facility. Saylor notes his facility holds six digital systems and four analog in its surgical inventory. All are valued medical tools, and ideally, provide the picture of perfect health.
Renee Diiulio is a contributing writer for 24×7. For more information, contact .





