 |
Three times in as many months, the computerized systems at the heart of Stanford University Medical Center’s cardiac catheterization labs froze, locking up tighter than a plaque-clogged artery. Mark Addis, CBET, of the clinical technology and biomedical engineering department needed to figure out the reason why.
Soon enough, he had his answer: the information technology (IT) department had been loading third-party anti-virus software at a data center server farm, and this software was incompatible with the proprietary programming package running on the networked systems in the cardiac cath labs. “Every time IT did this, it chewed up nearly all the RAM in my systems’ CPUs, which disrupted all 12 of the labs at the same time,” Addis says, whose main responsibility at the Palo Alto, Calif, hospital is the care and feeding of those rooms.
The first step Addis took to solve the problem was convince hospital decision-makers to give the cath labs a network domain of their own, one that he would control despite it still being on the IT department’s network. Equally important, he created a five-page document containing spreadsheets and schematics of the network interfaces with his systems. “I’ve got all the static addresses, including port locations and individual serial numbers,” he says. “So, now, if I am unable to ping any system on the cath lab network or if a networked system is running slow, I look up the name of the most appropriate IT person and give him or her the IP address of the system that’s in trouble, then ask if they can help me diagnose and repair the network problem.”
Addis says his solution has dramatically reduced system downtime involving network problems. Also, it has simplified his life “because I can basically now handle these problems from my desk with a quick phone call.”
Sophisticated Systems
Cardiac cath labs have been around since at least the 1960s, and there is not a major hospital anywhere in the nation without one—or two, or three, or more. Still, some institutions are only now getting around to bringing them aboard. “Mostly these are smaller facilities where this is happening,” says Craig Williams, CRES, recently retired senior field service specialist at Centura Health St Anthony’s Hospital in Denver and Westminster, Colo.
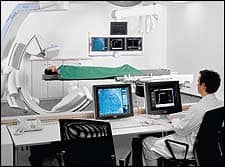
A cardiac catheterization laboratory is a room designed for the diagnosis and treatment of various conditions of the human cardiovascular system. For example, cardiac catheterization is considered the definitive test for the detection of coronary artery disease, the leading killer of adults of both sexes in the United States. Procedures almost invariably involve the insertion of a catheter into an artery of the patient’s arm or leg. The catheter is then guided along the artery until it reaches the heart. A variety of instruments—probes, cameras, wires, borers, cutters, or balloons—can be passed through the catheter to access whatever lies on the opposite end. All of this is accomplished using some rather sophisticated systems, starting with a hemodynamic monitor to keep tabs on the patient’s blood pressure and electrocardiogram data during procedures.
“Here at Stanford Hospital, each of our 12 rooms has hemodynamics equipment, primarily the MACLAB IT from GE,” Addis says. “Each hemodynamic unit consists of a computer, an integrated electronic box providing power and video to multiple monitors, and a TRAM module for collecting patient ECG, NIBP, invasive blood pressure, temperature, and SP02 data. There is also an EtC02 module for collecting patient C02 and respiratory rate data, a real-time display monitor and a review display monitor at the control workstation, and a real-time monitor at the procedure table.”
Equipment-Rich Environment
Some cath labs augment hemodynamic monitoring by adding an electrophysiologic monitor to look at patient intracardiac electrical activity and surface ECGs. “The electrophysiology system we’ve installed in four of our cath labs receives NIBP, SP02, EtC02, and temperature from the hemodynamics system, but adds a CardioLab amplifier to collect patient ECGs, invasive pressures, intercardiac signals, and cardiac stims,” Addis says. “The addition of electrophysiology capability also adds a third monitor at the workstation to collect fluoroscopy images and a review monitor at the procedure table.”
The fluoroscopy images to which he refers are generated by the single-plane or biplane x-ray system that every cardiac cath lab must install in order to safely guide the catheter on its journey through the artery. “The imaging systems in our cath labs are mostly Siemens, but we also have one from Philips and two, soon to be three, from GE,” Addis offers. It is not uncommon to find alongside the x-ray system an ultrasound scanner. This is typically employed to locate peripheral arteries. Nor is it unusual to find a more specialized ultrasound unit called an intravascular ultrasound system that produces images from inside the artery or heart rather than from outside.
Lasers too show up in cardiac cath labs. “We have a Spectranetics CVX-300 for, among other things, peripheral atherectomy and coronary atherectomy, and an AngioDynamics ELVS for treatment of severe varicose veins,” Addis says. “Our equipment complement is rounded out by a device called a Rotablator from Heart Technology that removes coronary artery blockages. It does this with a diamond-coated burr that spins up to 190,000 RPM inside the artery, converting plaque into particles smaller than red blood cells so that the body can remove the plaque as normal waste.”
Send in the Clones
Service issues associated with these various pieces of equipment run the gamut from simple to the vexing. For Williams, whose responsibilities at the two Colorado hospitals where he worked were three cath labs, an electrophysiology lab, a room for the programming of pacemakers, and nine prep suites, it was the hemodynamic systems that consumed the largest share of his time, but not due to equipment reliability.
“The problem was we had nontechnical personnel interfacing with a highly technical application,” Williams says. “The users of the hemodynamic system sometimes had difficulty understanding its capabilities and limitations, so a big part of my job was providing guidance to the clinical staff. For example, I would get a call for help from the electrophysiology lab; I would show up, ask what seemed to be the trouble, and the staff would spell out how this or that was all out of whack. I would then ask a few pointed questions, the invisible light bulb would turn on over their heads, and it would dawn on them what they needed to do in order to fix it themselves.”
That is not to suggest that cath lab systems are themselves trouble-free. Take hard drives. They, of course, sometimes go down. To minimize the effects of failed storage devices, Williams made a point of cloning each hemodynamic system’s computer hard drive every time he performed preventive maintenance (PM). “If a system died and the cath lab was down because of it, rather than spend 2 or 3 days replacing the computer, I simply grabbed the clone of its hard drive from where it was kept in my office, plugged it in, and could have the system booted back up in minutes,” he says.
Being a former factory field engineer and the beneficiary of extensive subsequent training, Williams was able to fully service his hospital’s hemodynamic systems on his own. Only the lab’s x-ray systems were under service contract—and a shared one, at that. “The reason for the shared arrangement was to ensure that we could quickly obtain the parts we needed,” he says. “That was important because these x-ray systems are so parts-intensive. Also, the service contract guaranteed coverage during the times I was off on vacation or out due to illness.”
Stop That Noise
The PM process at St Anthony’s entailed twice-annual inspections of the x-ray and hemodynamic systems, a process that consumed 1 full day per piece of equipment. Says Williams, “With the x-ray system, we conducted basic checks for radiation safety, calibration, and image quality. For the hemodynamic system, we confirmed that all ports were reading, that all displays were proper, and that pressures were accurately calibrated.” Tools Williams carted in on PM day included a laptop computer, a memory stick, a dosimetry gauge, and the usual assortment of screwdrivers, sockets, wrenches, and the like. The amount of time needed to PM each system necessitated careful coordination with the cath lab staff. “If a room was to be PM’ed, we had to schedule it well in advance,” Williams recounts. However, scheduling was no guarantee the room would be available to him for the full day. “I had to be ready to clear out at a moment’s notice and restore the room to full functioning. That’s because you can’t tell the cardiologist, sorry, but your emergency patient who’s dying can’t be in the room because I’ve scheduled it for PM.”
In the event Williams had to halt a PM in midcourse, he rescheduled it for another day. “The challenge in that was the cath labs were my highest priority, so any other work calendared for the same day of the rescheduled cath lab PM had to itself be rescheduled.” The resultant ripple effect could prove maddening.
Electronic noise is a big issue for biomeds in their care and feeding of cardiac cath labs. “Sixty-cycle noise interferes with the ability of the lab team in the electrophysiology rooms to detect certain heart conditions, such as tachycardia and other arrhythmia,” Addis says. “As a result, a signal must be as clean as possible, which means monitor cables have to be properly maintained. If I find frayed, worn, or broken cables, I replace them immediately.” And wear out they do, especially ECG surface lead cables. “These are radiotranslucent, so that they do not appear on the fluoro images, but their phenolic grabbers deteriorate quickly. I make it a point to change these radiotranslucent leads approximately every 3 months. The hemodynamic systems also have them, but don’t wear out as fast, so I space the replacement frequency to once a year.”
Addis finds that some seemingly minor PM chores can in reality be mission-critical. Checking the computer cooling fan grilles on the hemodynamic systems is a good illustration of how this is so. “Patient linen is washed and sterilized after each use, which gives off lint in the lab,” he says. “Enough lint is given off that the fan grilles can become completely clogged with it. As a result, when I perform my PM on the systems, I bring a HEPA-filter vacuum to give the computer a really thorough cleanout.”
In a sense, that is much akin to what transpires in the lab itself when patients are present. Making sure the equipment is able to clean out the arteries when the physicians and nurses go to use those systems is what the biomed contribution to the cardiac catheterization lab is all about.
Rich Smith is a contributing writer for 24×7. For more information, contact .
Clearing the Cath/Vascular Confusion
The term “catheterization lab” is sometimes used when referring to a similar but not entirely identical room known as a “vascular lab.” As a result, each can be confused with the other.
“Technically, a cardiac cath lab is a vascular lab, and they both do the same kind of work with many of the same kinds of systems and devices, but the difference is that the vascular lab does not concern itself with the heart, while the cardiac cath lab does,” says Craig Williams, CRES, recently retired senior field service specialist for Centura Health St Anthony’s Hospital in Denver and Westminster, Colo.
Contributing to the confusion is a blurring of turf barriers. “The cardiac cath lab is operated by the department of cardiology, while the vascular lab is operated by the department of radiology,” Williams indicates. This division seems straightforward enough, until the cardiologist brings in a patient with vascular disease of the heart. “If the patient has vascular disease in the heart, it’s likely he has vascular disease elsewhere in the body, particularly the legs,” Williams continues. “The cardiologist says he can handle the whole case himself in his cardiac cath lab, so why bother sending the patient to the vascular lab? And the opposite is true of radiologists with their vascular patients.”
What is beginning to happen as a result is a tight pairing of the two fields within the confines of the cath lab. Case in point: at St Anthony’s, the three newest cath labs are all dual-purpose rooms, able to handle both coronary and vascular cases.
“And when the hospital soon moves into a new building, the vascular and cardiovascular departments are going to be in a single location and will share all equipment,” Williams adds.
Long ago, cardiac cath labs and vascular labs were easier to tell apart by the equipment they utilized. “Vascular labs had film changers along with photo-spot cameras that could run to four or six frames per second, while the cardiac cath lab utilized cameras capable of speeds of 30 and 60 frames per second,” Williams says. “Today, the systems employed in the cardiac and vascular labs are different only in detector size and software features.”
—RS



