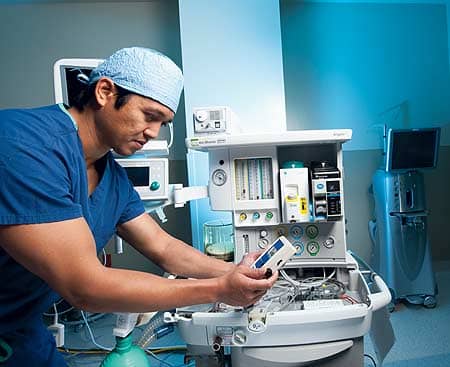
Jeff Leonzon measures oxygen flow in anesthesia equipment.
Technology is ubiquitous—from the nomad’s cell phone in the Sahara to the c-suite of Apple to the OR-suite of today’s hospitals in the United States. And as time marches on, the world finds that it wants many of these devices to communicate, intelligently. This means the biomedical/clinical engineer’s job is no longer about repairing a “box.” In fact, the biomed’s role has expanded far outside of the “box” in many US hospitals.
Clinical engineering departments have taken on responsibilities in acquisition selection, equipment replacement strategy, construction planning, user education, auditing, risk management, and cost reduction, all while continuing to manage conventional preventive and active maintenance programs. And even these old-school duties of equipment management have become more complex.
Many clinical engineering departments have expanded their inventories, both in numbers and device type. Radiology equipment is no longer off limits, and some biomeds are even beginning to enter the clinical laboratory. As their equipment knowledge expands, so too must their information technology (IT) skills, because today’s medical devices have to do more too, including communicate with other systems, such as alert notification programs, PACS, and the electronic medical record.
This means that clinical engineering departments have to learn to work with yet another hospital group—IT. And many have found that the best model is not to “beat them” but to “join them.” United, the two departments often enhance customer service along with patient care, the hospital’s ultimate goal.
As clinical engineering conquers more frontiers and wins over the hearts, minds, and wallets of administrators, clinicians, and IT, the profession is changing—has changed. Nowhere is this more evident then at the Olathe Medical Center in Olathe, Kansas. In the past 4 years, the clinical engineering department has transitioned from reporting to plant/building services to working under the chief information officer (CIO). As this change occurred, the department also expanded its responsibilities and inventory, bringing additional equipment service in-house through the elimination or alteration of contracts (ie, shared service agreements) where possible.
And, to make sure everyone noticed, Dan DeMaria, manager of Olathe’s biomedical engineering department, asked the team to dress the part. Although not required to “suit up,” the department’s members stay out of scrubs unless they actually need to scrub. “Perception is reality,” DeMaria says. “If our customers believe we’re doing a good job, then we are doing a good job. So we did a little to change the perception: We changed our attire, we changed the way we speak to people, and we worked from the bottom up to alter our customer relationships.”
Though this growth and the transition to IT were separate initiatives, together, the changes have combined to enhance both the actual and perceived value of the clinical engineering department. Customers are happy, administration is happy, and the team is happy. “[Our biomeds] are professionals, and they’re integral to taking care of our patients,” DeMaria says.
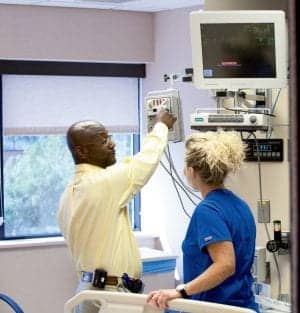
L-R: Lawrence Countee instructs nurse Erica Duffle on the differences between various types of SPO2 connectors.
Seen and Heard
The transition to the IT group helped to facilitate that ability along with the department’s enhanced perception in a variety of ways, with a major one including the ability to complete tasks more quickly and smoothly. “We maintained equipment as we always had, but we had more ready access at the operational level to resources, particularly expertise, such as with networking, desktop support, and clinical application specialists,” DeMaria says.
The streamlined workflow meant jobs could be completed more quickly and with less opportunity for unforeseen problems. Clinical engineering adopted the IT department’s model of change management, which brings in relevant experts to ensure there are no unexpected consequences. For instance, if a change is to be made to an IP address on a monitor, the biomed does not simply assign a new address. Rather, he consults with others to determine whether any software will be affected and if anyone else is already using the desired IP. When a change is made, everyone is officially informed. “So the whole process is well-defined, well-thought-out, and documented,” DeMaria says.
The new processes meant the biomed team was seen and heard in a more positive way, contributing to the new perception. “Under building services, we were the department that completed PMs and got to work on boxes,” says Brent Dawson, a BMET at the hospital. “Now, we still do those things, but we’ve expanded our work to include technical systems we could not touch before.”
New Hosiptal Order
From the biomed perspective, the integration of clinical engineering and IT has become an evolutionary necessity. “As a road warrior working on equipment, such as lasers and heart-lung machines, it became very obvious that computer technology was the way things were going to go when I opened up a laser and there was a PC built into it—a full PC box—that was controlling the laser with a communication card,” says Robin Faut, a BMET and a CE-IT hybrid.
With the advent of network communication in the 1990s, Faut notes, even troubleshooting seemed to require IT skills. So Faut left the biomed field for a short while and pursued IT training and employment. This unique background, which allows him to be comfortable in both worlds, made him perfect for the recently developed CE-IT hybrid position at Olathe.
DeMaria has been actively involved in the creation of this new position, participating in industry association efforts to make sense of the new “hospital order.” Organizations involved include the Association for the Advancement of Medical Instrumentation, the Healthcare Information and Management Systems Society, and the American College of Clinical Engineering. Though no formal statements or guidelines have been produced, hospitals are beginning to develop official CE-IT liaison positions more frequently (though no one has quite yet settled on a name).
At Olathe, the role is titled CE-IT specialist, and both DeMaria and Faut operate in this context though at different levels. DeMaria handles management issues, frequently working with interdisciplinary colleagues and teams, interacting with managers and directors, and guiding related projects. Faut, who is considered the CE-IT on the front line, combines his clinical engineering and IT skills to make sure equipment is properly and efficiently serviced and maintained.
“Even the simplest blood pressure machine integrates into the network, communicating and transmitting directly into the electronic medical record, sometimes wirelessly,” DeMaria says. This means that to repair a malfunction, someone is needed to fix the blood pressure machine, someone is needed to understand the networking aspect, someone is needed who comprehends security (HIPAA regulations always apply), and someone is needed who can work with the electronic medical record. “So this simple act of getting a blood pressure reading into a patient’s record now goes across many disciplines in the industry,” DeMaria says.

Mike Cain, CBET, diagnoses an anesthesia problem.
Knowledge is Opportunity
Therefore, biomeds who can expand their skill sets to improve their technical skills in any and, ideally, all of these areas, improve their ability to perform their job and grow their career. “The model of biomed techs working at a bench on a stand-alone box is rapidly changing, and so we’ve needed some additional skill sets,” DeMaria says.
DeMaria successfully lobbied hospital administration to exempt clinical engineering from budget restrictions on training expenses (the organization had decided to minimize its education budget in response to financial concerns). Where possible, educational opportunities are built into new contracts during the acquisition negotiations, and DeMaria continuously encourages the team to seek outside coursework and certification. The entire team has attended a basic networking course taught by a vendor.
DeMaria and Faut are both currently working on IT certifications; BMET Mike Cain, a 20-year industry veteran, just completed his CBET.
Team Mind Meld
While IT education can be extremely valuable, however, the learning is not one-way. At the same time that biomeds have to learn more IT skills, they have to teach their IT counterparts new service models. Both the customer and technician mind-set vary depending on whether the device is a true medical instrument or an IT issue, such as nonfunctioning e-mail.
DeMaria illustrates the difference by comparing the way an emergency department operates to clinical engineering (fluid workflow, rapid diagnosis of the problem, and an urgent response) and contrasting that with a surgical department, which he likens more to IT (scheduled work, refined resources, and well-defined processes). The differences are reflected in the expectations of the user and the technician.
“When an IT user encounters a problem, the user often doesn’t want to know what is going on. They just want the problem fixed,” Faut says. IT has often obliged, sometimes even fixing problems remotely. However, the speed with which these issues are addressed can vary based on the perceived importance of the system.
“IT is very, traditionally at least, business- and rules-set driven,” DeMaria says. “One of the common questions asked when you call an IT help desk is, ‘How many users are affected?’ That’s not a question we would ever ask in clinical engineering.”
The answer could be just a few users, with those individuals including a patient on a surgery table undergoing open-heart surgery and the operating team. Though the users are few, the need is urgent, and clinical engineering must respond quickly.
When a biomed comes in to affect a repair, he/she must be sensitive to both patient and user concerns and will often have to engage in discussion with the user. “We have to speak with the clinicians to get information and make sure we know that what we’re doing isn’t going to create another problem,” Faut says.
To align the two teams together, the senior managers in Olathe’s IT department meet weekly to discuss projects in the pipeline and any related problems. “Through these meetings, we’ve really begun to get an understanding of the unique challenges in each department, and the other IT managers have begun to understand that clinical engineering issues are much more time sensitive than ‘one user’s e-mail isn’t working,’ for instance,” DeMaria says.

CE-IT specialist Robin Faut (foreground) discusses the status of a patient monitoring alarm notification server with Dan DeMaria, manager, biomedical engineering, Olathe Medical Center.
As IT has begun to accept the urgent need for attention to biomed calls, they’ve also begun to feel more a part of the patient care team—as opposed to merely supporting a network. And now, when Faut approaches them with a network issue, he finds them much more likely to drop what they’re doing to fix the problem. “We work as a team to solve the issue,” Faut says.
Success Breeds Success
The stronger team has helped to facilitate the growth of Olathe’s clinical engineering department. Four years ago, the team consisted of two techs who performed PMs and some emergency repairs. Most work was sent out to vendors via contract.
Today, the team has expanded to five techs and manages a larger portion of the service for an equipment inventory that includes 6,500 devices across two hospitals and which will grow even more once an agreement to service 32 Olathe Health System clinics is concluded. Only a few devices, primarily those with a low inventory (often single items), still remain under vendor service contract.
Each biomed has a specialty area for which they are the primary contact, but they are certainly not restricted to that one field. The team works together and delivers cross training (through team whiteboard sessions) when needed. So, for instance, Dawson handles imaging while BMET I Jeff Leonzon covers surgical equipment (and is subsequently most often still in scrubs), but, if necessary, they will work in each other’s areas.
The transition has occurred gradually, with the team cutting service contracts and increasing shared service arrangements. They found the cost for these was often less than half of the existing contract, and as the team completed a greater number of PMs and additional troubleshooting, they became more comfortable with the equipment and more skilled at its maintenance, allowing them to take on more service and reduce contracts further.
As many clinical engineering departments have done, Olathe’s biomed team moved into radiology and it is now beginning to target the clinical lab. “We brought new talent on board and showed that we can do the job and do it for less money and often better because we can provide an instant response,” DeMaria says.
Cain points out that the improved ability to care for equipment has helped to reduce failure rates. “We had a big problem with surgery table repairs in the OR, but we’ve pretty much eliminated that with regularly scheduled maintenance,” Cain says. “And we’ve been able to reproduce the result over quite a range of equipment.”
Part of that effort involves a thorough examination of equipment undergoing any type of service to fix all problems on failures, even when they fall in-between scheduled maintenance. If the team notices a problem with a particular type or brand of device, it takes a proactive approach. “We look at history and failure rate, and if we see a trend, we address it without necessarily waiting until it’s due in 12 months,” Cain says.
The overall cost savings from the improved uptime and contract reduction have been tremendous—resulting in hundreds of thousands of dollars annually, DeMaria estimates—earning the team the respect and confidence of administration, who is now willing to let them take on even more.
Perception is Reality

Foreground left, Mike Cain, CBET, discusses future education sessions with Robin Faut (L) and Lawrence Countee, while Dan DeMaria (at board) clarifies x-ray tube physics theory questions with Jeff Leonzon.
The Olathe clinical engineering department has also won over clinicians with its improved service and communication skills. Before any changes were made, the department surveyed the various units to discover what the biomed team was doing well and where it could improve. A common constructive criticism targeted communication.
“The guys could fix the equipment—that was the easy part—but it wasn’t evident to our customers that we were supporting them. Things just seemed to get magically fixed,” DeMaria says. So customer engagement became a big focus.
This meant (and continues to mean) regular visits to the floors to check in with customers and ensure their needs are being met. The new style has brought both challenge and opportunity.
Lawrence Countee, another 20-year industry veteran and the fifth and newest BMET on the team, discovered within his first 4 months at Olathe that almost everyone he meets is a customer. “I had to learn to identify and know the customer, and when nearly everyone is a customer, it can be a challenge to know them all,” Countee says.
Done right, however, it can make the job a joy. Dawson has found that the ability to connect with his customers has made his work easier. “Customers begin to call you directly, and it’s easier to deal with issues when you have a good relationship,” Dawson says.
Owning It
It also inspires ownership. If Dawson notices a potential problem, he can proactively work with the unit to prevent any potential failures. And when a problem requires the assistance of another expert, Dawson, or any biomed member, will manage that request himself rather than just refer the customer to another department (IT networking, for example). Once the repair has been made or the request fulfilled, the biomed team will report to the clinical department that the issue has been resolved, including mention of the steps and experts involved. This ownership has also contributed to improving the team’s overall perception as they have become known as a group that will get the job done and done right. The positive opinions have worked their way through the hospital hierarchy.
“As a result, senior and executive management have recognized that we do a lot and are willing to provide more support. Through that process, we’ve more than doubled the size of the department and the amount of equipment we’re working on, and we’ve done so for approximately 35% less budget,” DeMaria says.
Key to the success has been a change in perception, and key to that perception has been exposure—with more impressive attitudes and attire. Dawson recounts how customers would ask if he had changed departments or become a manager when he began to dress in a business-casual style (described as khakis, dress shirts, and comfortable but “good-looking” shoes, no ties required). The response increased his confidence and, in turn, his capabilities. He is now accepting first call on all radiology equipment, which he states he would not have been able to touch 4 years ago when it was still under contract.
Ultimately, it benefits the clinical engineering department to be visible. “Biomeds are going to have to be seen and heard more to be appreciated,” Faut says. And if they are to be seen and heard more, dressing the part doesn’t hurt.
Renee Diiulio is a contributing writer for 24×7. For more information, contact .