Growing use of image guidance and stereotactic techniques represent major clinical trends
By Elaine Sanchez Wilson
When 24×7 Magazine sat down with the leading manufacturers of linear accelerators (linacs), the panel of experts left no shortage of words in describing how the cutting-edge technology is shaping radiation therapy offerings and improving outcomes for cancer patients worldwide.
Roundtable participants included David Famorca, head of global marketing for Linac RT (including TPS), global marketing and strategy at Elekta in Sweden; Corey Lawson, vice president of product strategy at Accuray Inc., of Sunnyvale, Calif.; and Ed Vertatschitsch, vice president of global portfolio solutions at Palo Alto, Calif.-based Varian Medical Systems.
24×7 Magazine: What are the top two or three trends in the radiation therapy field today, and how are they influencing the design and development of linac technologies?
David Famorca: Advances in image guidance technology and artificial intelligence, the availability of big (and actionable) data and ubiquitous cloud computing are key drivers of innovation in the field of radiation therapy and, more broadly, the medical device industry.
Improvements in imaging technology that now allow clear differentiation between tumor tissue and surrounding tissues and structures have been a significant catalyst for allowing clinicians to learn more about the behavior of certain tumors at the time of treatment. This knowledge has empowered them to re-think the way radiation dose objectives are approached and improved their ability to effectively target the tumor while minimizing damage to healthy tissue.
When Elekta first launched volumetric cone-based CT (CBCT) imaging in the early 2000s, many customers said it would be a niche technology that only academic centers would adopt. Some 10 years later, CBCT is now a standard of care in radiation therapy. Importantly, integration of imaging technology has transformed radiation therapy from a treatment used as a last resort primarily for palliative care to an accepted alternative to surgery for several indications. This has been particularly beneficial for inoperable patients, who previously had few treatment options. Many of the advanced stereotactic techniques that are now considered routine practice were enabled by image guidance.
Continued advances in imaging technology will also catalyze truly personalized cancer treatments. Elekta’s MR-linac, for instance, has extraordinary potential to unlock critical insights into how to optimize care for each patient. It will enable clinicians to not only better understand the biology of a patient’s cancer, but also to measure functional and many other critical parameters of tumor targets.
MRI at the time of treatment will allow clinicians to mitigate motion and escalate doses, helping to improve efficacy and safety. Perhaps most importantly, the integration of MRI with radiation therapy allows rapid adaptation of the treatment plan based on real-time evaluation and response to changes that occur during the course of treatment. This helps to ensure treatment optimization.
The continued role of advanced imaging during diagnosis, treatment, follow-up, and re-treatment will create more data in the patient’s electronic record. Such data is crucial and will be used at multiple decision points throughout the treatment continuum and patient journey story-boarded by clinicians through the electronic medical record.
Large amounts of data—not only clinical, but also economic—become powerful only when they lead to actionable insights. As more data parameters are collected and required for making complex decisions, computing algorithms will become more complex and self-teaching.
Corey Lawson: Adaptive therapy is an innovative concept whereby the user of a linear accelerator detects changes in patients and the characteristics of their treated region, and adapts the radiation therapy plan to account for the changes. Between the first fraction to the last, a patient may gain or lose weight, and the target may shrink or change shape. As a result, normal radiosensitive anatomy may shift location within the body.
In order to remain true to the original treatment objectives, while protecting normal radiosensitive structures from receiving too much dose, many plans must be adapted to account for such anatomic change. Accuray’s PreciseART Adaptive Therapy, for instance, is a new clinical tool that automatically monitors for changes that can happen while a patient is undergoing treatment, compares the current state to the original treatment plan, and enables plans to be adapted when necessary. This new technology makes it easy for clinicians to routinely incorporate adjustments to the treatment planning and delivery process.
Motion compensation is the next step in managing moving targets that are undergoing treatment. Legacy technologies typically relied upon turning the radiation beam on when the target came into a predefined window within the path of movement, and turning the beam off when the target moved outside of that window. Delivering in this way was time-consuming and impractical for many clinics to integrate into daily practice.
The result has commonly been to deliver radiation to the full path of motion, regardless of target location, with the result that more normal tissues than necessary may be irradiated, and high doses of radiation are potentially delivered to organs at risk. Adjusting the beam in real time along the full motion path of the moving target, while avoiding normal health tissue, was the desired implementation that has only recently been made possible with Accuray’s Synchrony respiratory tracking technology.
Synchrony is able to track and adjust the radiation beam automatically in real time to the moving target—supporting high precision dose delivery to moving targets while reducing dose to normal healthy tissue and overall treatment time.
Ed Vertatschitsch: The biggest trend we’re seeing, in the United States and around the globe, has to do with a drive toward greater cost effectiveness in healthcare. In the U.S., this takes the form of a movement toward bundled reimbursement for treating specific conditions, requiring treatment providers to be more cost effective in how they provide care. Although radiation therapy has long been a very cost-effective approach to treating cancer, it can always be improved.
Varian, for instance, has been designing platforms like the new Halcyon system, which enables clinicians to deliver very high-quality care quickly and with reduced burden on infrastructure and resources. Halcyon, along with the latest release of our Eclipse treatment planning system, offers the promise of improved tumor coverage and minimized exposure of normal healthy tissues for some disease sites.
New Varian solutions also automate and expedite treatment planning, machine performance QA, imaging for patient positioning, intensity modulation, and RapidArc therapy for delivering highly conformal dose distributions quickly. Speeding up treatment offers additional benefits beyond cost efficiency. Patients have the potential to receive a more accurate treatment since faster treatments leave less time for tumor “drift” or patient motion.
A second trend—related to the first—is the move toward hypofactionated treatment approaches, which prescribe fewer treatment sessions than conventionally fractionated treatments. These more cost-effective approaches also have the potential for improved outcomes. Varian’s new HyperArc high-definition radiotherapy enables clinicians to plan and deliver non-coplanar treatments that offer extremely high conformal tumor dose and lower doses to healthy tissues.
The next release of Varian’s Eclipse software, which is pending U.S. FDA 510(k) clearance, will facilitate the planning of HyperArc treatments for delivery on the TrueBeam platform, with enhanced safety features such as preplanned imaging waypoints and collision avoidance designed into the treatment plan automatically. The treatments are then delivered with a single button push. HyperArc will enable clinics to more easily adopt highly non-coplanar treatment strategies in the delivery of stereotactic radiosurgery while significantly reducing the time required to plan and to deliver such treatments.
A third global trend that bears mentioning has to do with addressing parts of the world where access to radiotherapy is very limited. In many of these regions, the cancer burden is accelerating because significant progress has been made in the management of communicable diseases, and people are living longer.
These cancer patients expect and deserve the same standard of care available to patients in other parts of the world, but they live in places that are sensitive to capital acquisition costs and challenged by insufficiently qualified personnel and insufficient infrastructure to serve the burgeoning cancer population. This is another factor fueling the impetus to find ever-more-cost-effective solutions that are world-class in their functionality yet simple to operate and maintain.
24×7: What are the needs of your particular customers, and how do your product offerings meet these demands?
Vertatschitsch: Varian has a diverse customer base, but there are a few themes that all have in common. All of our customers expect the highest level of safety, delivering the most advanced therapies with highly reliable technology. That’s important to everyone, from large hospital systems that cross regional boundaries to local, single-vault centers that can ill afford any downtime.
All Varian products are designed for maximum clinical availability, and the latest systems—like TrueBeam and Halcyon—ensure the availability will be maintained even as customers treat more and more patients every day. What’s more, these systems offer SmartConnect remote servicing. This allows Varian personnel to perform diagnostic and support services remotely, via a secure network connection. For issues that require a service visit, Varian maintains service personnel and regional parts banks around the world to enable fast response everywhere.
Varian customers also need the ability to deliver the latest therapies efficiently, and at a high level of quality. For example, Varian’s HyperArc high-definition radiotherapy solution offers clinicians a practical way of delivering non-coplanar stereotactic radiosurgery (SRS) treatments on the TrueBeam system—something many customers will now be able to offer patients while avoiding complex and resource intensive manual approaches to delivering sophisticated treatments. Varian’s RapidPlan knowledge-based treatment planning has similarly “upped the game” in the realm of radiotherapy treatment planning.
RapidPlan helps clinicians use models (their own or others’) as starting points for taking treatment planning to new levels of consistency and quality and breaking through productivity barriers in the treatment planning process. RapidPlan makes it easier for new treatment planners to produce quality treatment plans and enables all planners to spend more time on the most difficult patient cases. So RapidPlan has an important role to play, both in places where experienced planners are working and in places where experience is being developed.
Lawson: In a phrase, precise delivery. Accuray customers require technology, which enables them to provide precise, high-quality radiation delivery to any patient needing treatment. The span of patient cases is very broad, with more common cases at one end of the spectrum and extremely complex cases at the other. Some cases may be traditionally fractionated, while others hypofractionated. [Fortunately,] Accuray has a diverse product portfolio able to treat the full range of clinical cases efficiently, with precision and accuracy.
Further, seamless integration of best-of-breed technologies is becoming more prominent as departments continue to optimize clinical capabilities, without impeding workflow efficiency. Accuray’s new iDMS data management system enables a high degree of interoperability within and outside of the Accuray ecosystem. It enables connectivity to a variety of oncology information systems, treatment planning systems, simulation systems, and other products that conform to common DICOM standards.
And finally, [customers demand a] future-friendly investment. Customers rightfully have the need to ensure success in today’s fee-for-service reimbursement environment, while also setting themselves up to thrive in a value-based reimbursement environment in the years ahead. The products within Accuray’s portfolio enable highly efficient patient treatments in support of the throughput necessary for success in a volume-based reimbursement model. These same technologies provide high-precision, high-quality treatments that can reduce costly side effects common with legacy technologies, while also improving outcomes, thus enabling significant advantages in a value-based reimbursement future.
Famorca: There are two words in ‘image guidance.’ Customers will not only need sophisticated imaging tools but, equally as important, sophisticated, and automated guidance and decision support tools. The goal is to develop powerful solutions that provide unsurpassed accuracy and efficiency in a highly cost-effective manner. There is an anticipated explosion of new patients accessing cancer care from the emerging and frontier markets.
Additionally, cancer patients in mature markets are living longer. These trends are contributing to an increase in the per capita utilization of linac systems. These systems will need to be robust, clinically flexible, and operationally efficient to serve a very high throughput of patients.
Still, no amount of system design or artificial intelligence will replace human intelligence. The development of advanced and accessible education and training programs is equally a priority for our company, particularly for emerging and frontier markets. It is our obligation as solution providers to ensure that we do our part and utilize our resources and professional networks to maximize knowledge and skill development for our customers—not only to enable them to be proficient with our products, but to contribute in their professional development and progression in general.
This will ultimately—and most importantly—translate into better treatment administration for patients. Augmented and virtual reality technology will be key enablers in facilitating rapid learning and will bring the deployment of more advanced treatment techniques available to patients faster.
Elekta is a pioneer in image guidance. With the upcoming release of our high-field MR-linac, we will enable clinicians to raise the standard, and hopefully outcomes, of treatment once again.
We are continuing to invest in advancing our leading image guidance tools, making them more sophisticated while utilizing automation and intelligence to simplify their operation and make them more accessible for clinicians and radiation therapy staff. Integration of the oncology information system, treatment planning software and delivery device will also be critical in facilitating a truly online and real-time adaptive treatment workflow. We are constantly advancing new approaches to integrating these major software and hardware components to drive higher efficiency and safety.
24×7: What special considerations or best practices should be considered in the servicing, maintenance, handling, and repair of linear accelerators?
Lawson: Technically speaking, service of linear accelerators is not too dissimilar from service of other large complex medical devices like those that you might find in radiology, for example. An important distinction for linear accelerators is how they are used clinically.
These devices are programmed to deliver precise doses of radiation for each individual patient that will be administered on a strict schedule over the course of several days or weeks. For this reason, interruptions in equipment availability can impact not only the clinical operation and the business for our customers, but the patients themselves. Items that should be considered in the service and support of linear accelerators include:
- The level of partnership from the service provider and sensitivity toward patient care and experience
- Expertise, availability, and infrastructure of the service team to support the systems
- Availability of tools to monitor, detect, and diagnose issues before they affect patient care
- The ability of field service engineers to efficiently and effectively restore system operation with minimal disruption to schedule and/or departmental workflow when issues do arise
Famorca: Best practices include knowledge transfer, remote monitoring and predictive maintenance, automated machine calibration, and departmental quality assurance (QA) resource management.
Vertatschitsch: In addition to remote servicing, our SmartConnect Plus technology enables Varian to perform predictive assessment and maintenance, so that issues are resolved before they cause any downtime. Varian is also engineering greater integration of diagnostics, quality assurance (QA) tools, and performance indicators within systems, with the goal of minimizing the amount of time the physics team needs to execute their QA program.
Further, the Halcyon system requires less shielding than traditional systems, needs no base frame, fits in smaller vaults, and is faster to commission. All of the ancillary components—the intercom, the solid-state modulator, the camera, lasers, and primary shielding—are integrated and, therefore, can be installed as one unit. Also, a five-minute machine performance check is carried out automatically on a daily basis. These are all innovations that were developed with customer needs in mind.
24×7: Which clinical areas do you expect to see the most growth in the coming years?
Vertatschitsch: As previously suggested, we see hypofractionation, and especially stereotactic approaches to treatment such as SRS and stereotactic body radiation therapy (SBRT), being among the highest-growth clinical areas for reasons articulated above. We also see new studies appearing that demonstrate how the newer, more advanced forms of imaging and radiotherapy might make it possible to successfully address cancers that have traditionally been the most difficult to deal with, such as pancreatic and liver cancer.
Finally, in the longer term, Varian is committed to supporting research into the biology of cancer in order to better understand how the various modes of radiotherapy can be most-effectively applied, particularly in conjunction with emerging forms of chemo- and immunotherapy. Specifically, we are exploring ways to facilitate greater collaboration across medical disciplines in order to arrive at optimal treatments for each cancer patient.
Lawson: There are four areas that represent clear development opportunities in the field—each of which Accuray has long-anticipated:
1. Real-time, automatic image-guided delivery: The goal is for high-quality images to automatically guide the delivery of radiation from moment to moment. In this realm, development seems to be focused more on the imaging portion of the equation (for example, MRI during radiation therapy)—the ability to automatically and immediately change the aim of the radiation beam based on those images is still under investigation.
Accuray, on the other hand, with its CyberKnife system uses high-quality images to alter automatically and in real-time the delivery of the radiation to keep it on target. Many studies have shown this greatly reduces the amount of normal, non-disease tissue that is exposed to radiation, which on average should reduce the frequency and severity of radiation side effects.
2. Continued increase in hypofractionation: Randomized studies of hypofractionated treatment of breast, prostate, etc., have shown that increasing the daily dose above 1.8-2.0 Gy can yield comparable clinical outcomes without excess toxicity. This allows treatment to be completed in less time—three to four weeks versus five to eight weeks, depending on the treatment site—and thus reduces costs and inconvenience to patients.
SBRT, also called stereotactic ablative radiotherapy, and stereotactic radiosurgery are extreme forms of hypofractionation that are becoming more prevalent as data indicating their effectiveness throughout the body accumulate. Lots of data indicate the effectiveness and safety of SBRT for early-stage lung cancer and lung metastases, for example. Recent CyberKnife studies show excellent clinical outcomes with 4- or 5-fraction SBRT for organ-confined prostate cancer.
3. Personalized treatment: As researchers understand more and more about the specific biologies of cancers, they’re able to devise more specific approaches to intervening in a biologically rational way. This will include radiation therapy in at least three ways: First, use of SRS or SBRT in combination with chemotherapies allows a more efficient scheduling of combined therapies, compared to more conventional radiation therapy (RT), which can interrupt systemic therapies for weeks.
Second, understanding of differences in radiation sensitivity within tumors and across different tumors may allow creation of RT plans that boost dose to radioresistant regions and may allow chemotherapeutic intervention that makes tumors more sensitive to radiation. Finally, high-dose RT may enhance the effects of some systemic therapies, such as chemotherapy and immunotherapy.
4. Cancer as a chronic disease: The concept of “oligometastasis” implies that some metastatic cancer, occurring after treatment of primary cancer, may be treated locally and aggressively in a manner that confers a long-term disease-free period. In combination with frequent surveillance of cancer recurrence and chemotherapies, local treatment could be an effective approach to continued management of cancer, allowing patients to live with the disease for an extended period of high-quality life. Development of better surveillance, local therapies, and a better understanding of cancer biology will help make this “chronic disease” concept a reality for more patients.
Famorca: Stereotactic treatments will continue to grow, and their adoption will increase as long-term survival data are reported. As this trend continues, radiation therapy will help alleviate the burden currently placed on surgical departments and also address the needs of inoperable patients, who previously had few treatment options. Brain metastasis and oligometastatic incidence will continue to grow as patients live longer and require multiple retreatments throughout their lifetime. The use of SBRT to treat tumors in the lung will continue to grow, and more patients will elect this modality over more invasive treatment approaches. As the body of data on long-term survival grows, prostate SBRT will follow the same adoption and growth path of lung SBRT. The availability of high-field MR imaging at the time of treatment will also unlock radiation therapy as an option for cancers that were typically untreatable or treated sub-optimally with radiation therapy, such as liver and pancreatic cancer.
Elaine Sanchez Wilson is associate editor of 24×7 Magazine. For more information, contact [email protected].
Sidebar: Hand in Hand: MR in the RT Room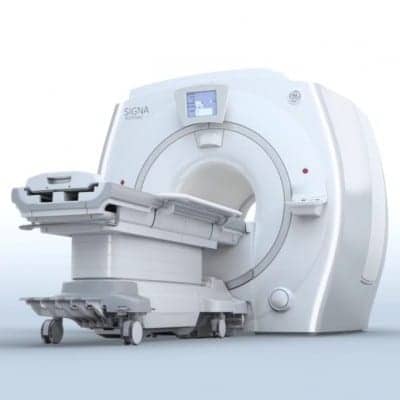
With today’s radiotherapy providers looking for solutions that enable more precise visualization of targets for improved accuracy, clinicians are increasingly incorporating MR during RT procedures to help differentiate tumors from surrounding anatomy.
“MR is the imaging modality of choice when it comes to superior soft-tissue contrast, which makes it a natural fit in radiation therapy treatment planning,” says Baldev Ahluwalia, general manager of the beyond MR business segment at Waukesha, Wis.-based GE Healthcare. “This trend has led to a tighter integration of MR imaging data with therapy devices.”
In fact, Ahluwalia notes that more than 30% of radiation therapy cases around the globe use MR, and GE does not expect this growth to slow down. After all, the modality offers various benefits, such as ensuring the preservation of healthy tissue and facilitating faster dose delivery. Furthermore, MR imaging itself does not emit dose, therefore making it useful in adaptive radiotherapy procedures.
“Adaptive radiotherapy allows clinicians to modify the course of radiation therapy based on the patient’s and tumor’s response to the treatment, as well as account for physical changes such as weight loss, which can sometimes accompany radiation therapy,” Ahluwalia says.
GE’s portfolio of MR systems includes the Signa Architect T and Signa Artist T—3T and 1.5T wide-bore scanners, respectively—that are optimized for radiation oncology. “We are working toward solutions that take patient comfort to the next-level during imaging to further improve the experience,” Ahluwalia continues. “Our solutions provide a way to image the patient in exactly the same position in which they will be treated, therefore allowing for better fusion with other imaging modalities, such as CT, and better reproducibility on the linac couch.”
—E.S.W.