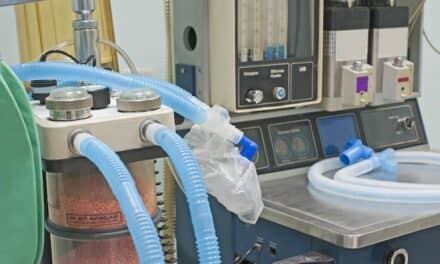
Ventilators are reliable machines, but routinely testing them and following strict maintenance schedules make them more so.
Using a squeeze bag with a mask attached to manually ventilate patients who cannot breathe on their own is an extremely rare occurrence. But for Don Allen, BMET, a single experience of it underscores how important it is that he and biomedical equipment technicians (BMETs) like him take their jobs servicing ventilators seriously.
“A facility’s backup generator failed, which meant that all 16 patients on ventilators had to be manually bagged for 4 hours until the power came back on,” Allen says. “In a situation like that, there’s not a whole lot you can do.”
If a ventilator goes down, the option of last resort is hand bagging, which means a one-on-one effort between attendant and patient. It’s a staffing nightmare for hospitals. And it’s exhausting for the respiratory technician or nurse who may have to do it, Allen says.
Trial and Error
Modern ventilator manufacturers have helped prevent many emergencies by making the machines reliable. “A lot of the problems tend to be the operators,” Allen says. “True hardware failures, we don’t have a lot.”
Like nearly everything else, modern ventilators have developed through a lot of trial and error.
In the earliest days of mechanical ventilation, the devices were sometimes called “death machines,” Allen says, because patients on ventilators long-term wasted away because they expended more energy undergoing ventilation than they could replace with the calories they were taking in. “It takes more energy to breathe on a ventilator than it does to breathe normally,” Allen says. “Try breathing through a straw; it’s hard to do.”
Allen, who is team leader in the biomedical engineering department at Charlton Methodist Medical Center in Dallas, is in charge of servicing about 20 ventilators that the 200-bed hospital owns. Nowadays, he says, the hospital adheres to a strict preventive maintenance (PM) program, which includes a full functional performance certification checkout every 6 months. Additionally, each machine undergoes a periodic extended self-test (EST).
The machine is programmed by the manufacturer to perform the EST. “The self-test checks all the components of the system except the power supply—basically, that’s every pneumatic system that it has—and it calibrates the circuit,” Allen says.
Also, before any ventilator is put on a patient, it goes through a checkout to make sure that it’s functioning and not leaking, Allen says. If a leak alarm goes off and the respiratory technician cannot find the source of the leak, the machine is sent to Allen for a full EST and repair.
Cause for Alarm?
All ventilators have alarms, but some alarm systems are more sophisticated than others and can assign a priority to the emergency. It may be a leak, which could be dangerous, or it may be only that a patient who’s coughing has set off a pressure alarm, which might not be of much consequence, Allen says. “But you can’t tell from across the room,” he says.
Because ventilation is critical, the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) has issued a set of standards for ventilator alarms. Part of a PM, Allen says, is to make sure that the machines comply with these standards.
But, he adds, the problem isn’t with the machines. The problem, he says, is that so many alarms go off in the wards of a busy hospital that the staff often can’t respond to them all. “There are so many other alarms, from infusion pump monitors, for instance. How can you tell that it’s a ventilator alarm?”
Newer ventilators use systems of flashing lights in conjunction with audible alarms, and sometimes rank alarm severity with different colored lights so that busy nurses or respiratory therapists (RTs) know if they need to interrupt what they’re doing to attend to that ventilated patient, Allen says. Additionally, Charlton Methodist Medical Center has hooked all its ventilators in use to a central monitoring system, so that attendants can watch for alarms and then call on staff to deal with emergencies.
Still, industrywide, Allen says, responsiveness to alarms remains a problem. “You’re dealing with nurse apathy or therapist apathy,” he says. “You try to develop standards, but you’re dealing with nurses who have a very high workload.”
Allen isn’t the only one to recognize a problem with alarms. Bill Rice is manager of clinical engineering at Baptist St Anthony’s Health System in Amarillo, Tex.
He says Baptist St Anthony’s flagship hospital, of the same name, and five other facilities in the system are planning to implement a patient information and communication system (PICS) over the next 5 years that will do away with the present pager-based alarm-response system.
“Now, the alarms are being monitored in many locations,” he says, “but we are looking to integrate all of that into one system that will include not only respiratory but will extend to diet and even to clergy for patient-family consults. We think it will be 5 years to full implementation, and 2 years to take the present pagers with a human interface and integrate that into one pipeline, streamlined system.”
Testing Lungs
Testing lungs, or test/training lungs, as they’re often called, are a critical component in the servicing and evaluation of ventilators. These lung simulators take the place of a patient when a ventilator is being tested for leaks, for example. The test/training lungs are hefty machines that can be programmed to mimic different patient diseases.
“Sometimes, you have problems with ventilators that are difficult to duplicate without a patient being on them,” Allen says. “Most ventilators have gone to a system of measuring what’s released and what comes back from the patient (during a respiration cycle). If it doesn’t get a return, then it alarms.”
To simulate return exhalation to check a ventilator alarm system, for example, Allen says, he hooks the ventilator to a test lung. He also uses the test lung after the installation of some PM kits. “We let it run for an hour or so, just to make sure the installation was right.”
Bill Sovitsky, CBET, CRES, a biomedical equipment specialist for the Air Force Medical Evaluation Support Activity (AFMESA) at Fort Detrick, Md, is using test lungs for comparative evaluations of ventilatory resuscitators powered by compressed gas and transport ventilators (see sidebar, page 29). “I like the test lung even for a battery test,” Sovitsky says, “because it gives you a similar load to real resistances.”
The Cost Factor
During comparative evaluations, Sovitsky is free to concentrate on the various pieces of equipment instead of focusing on price. “I just want to test. In the testing arena, price is not a prime consideration, although it comes into play later during the acquisition process.”
Elsewhere, clinical engineers and service engineers see a role for themselves in saving their institutions money, if and when they can.
“Saving money, that’s why we’re here,” Rice says. “We treat clinical engineering as a business. Our budget includes the parts and maintenance for all of biomed and radiology.”
Rice says the hospital already has a preimplementation review procedure in place for all new equipment and that clinical engineering (CE) has a role in that. If equipment problems show up, then those vendors will be flagged for financial review, he adds. CE also reviews all purchase requests for equipment it services, he says.
Seasonal Demand
Don Ast, BMET, is senior technician at Baptist St Anthony’s. He says the demand for ventilators varies with the patient load but also varies seasonally, with allergy and flu seasons increasing demand. During flu and allergy season, Baptist St Anthony’s does what most hospitals do when they run short of ventilators: They rent more.
At Charlton Methodist, Allen says that if he can’t get ventilators from rental companies, he’ll do whatever he can to find them, calling other hospitals, even begging vendors for them. “The vendors do try to help out,” he says.
During heavy demand times, he says, PM schedules are pushed back until the demand goes down.
“The biggest problem most biomeds have with ventilators is just getting a hold of them,” he says. “It’s not repairs, it’s accessibility. In the winter when it’s flu time, you have a ventilator come off the floor, you get it cleaned up and run a quick EST, so the downtime is an hour instead of a day.”
Patients are never put at risk to do PMs on ventilators.
Instead, scheduling concessions are made. “You have to work with each department,” Allen concludes.
George Wiley is a contributing writer for 24×7.
| Front-Line Equipment: Comparative Evaluations Now available for emergency, short-term use are small resuscitators and portable ventilators that run on pressurized gas or batteries and can be used in place of hand bagging. While they can be used in any emergency setting, they are particularly critical for use in military field hospitals and by medics on the front lines in a conflict.
Bill Sovitsky, CBET, CRES, is a biomedical equipment specialist for the Air Force Medical Evaluation Support Activity (AFMESA) at Fort Detrick, Md. He has been doing comparative evaluations of ventilatory resuscitators powered by compressed gas, and he is in the middle of a similar evaluation of small transport ventilators whose compressors run on batteries. In both evaluations, he has used test/training lungs to compare the equipment of different vendors. Resuscitators “We brought in six devices, and we have now down-selected to three; and some lab and field tests and reports are being generated,” he says. Using the test lungs, they were able to differentiate between resuscitators that would respond (stop cycling) if the patient began to breathe spontaneously and those that just kept going whether the patient started breathing or not. “Those that wouldn’t react to spontaneous breathing, that was a down-select criteria,” Sovitsky says. “Those manufacturers said that if the patient started breathing to just take them off. We wanted something that would react to spontaneous breathing.” After being differentiated on the test lungs, the resuscitators were sent to RTs and anesthesiologists to work with on patient simulators, Sovitsky says. Transport Ventilators The transport ventilators, although bigger than the resuscitators, are still small devices—maybe 6 inches long and wide and 3 inches high—that are designed to ventilate for several hours on battery power. He says test/training lungs were key to the evaluation of these small units. “You get a more realistic trend on how your battery is going to deplete and what happens to the unit as your battery goes out. You might lose tidal volume because the pump becomes less efficient, even though breaths per minute may not change.” Sovitsky also used the test lung to mimic various respiratory conditions—emphysema, acute asthma, and pneumothorax—to see how the transport ventilators would respond. “With changing compliances, you can get pressure rate changes—is your per-minute volume changing, for instance? You can see how changes in the physiological condition change the ventilator rate,” he says. Sovitsky says he and his team also consider the “effectiveness and suitability” features of each machine and look at the manufacturers’ maintenance and PM specifications. When the comparative evaluations are finished, he says, the results will be forwarded up the Air Force command ladder, where the decision to purchase a unit—if there is one—will be made. “I’d be confident with what I’ve done that we provide valuable information to the chain of command,” he says, “that we’re getting the right thing to the war fighter, facilitated by the test lung.” —GW |