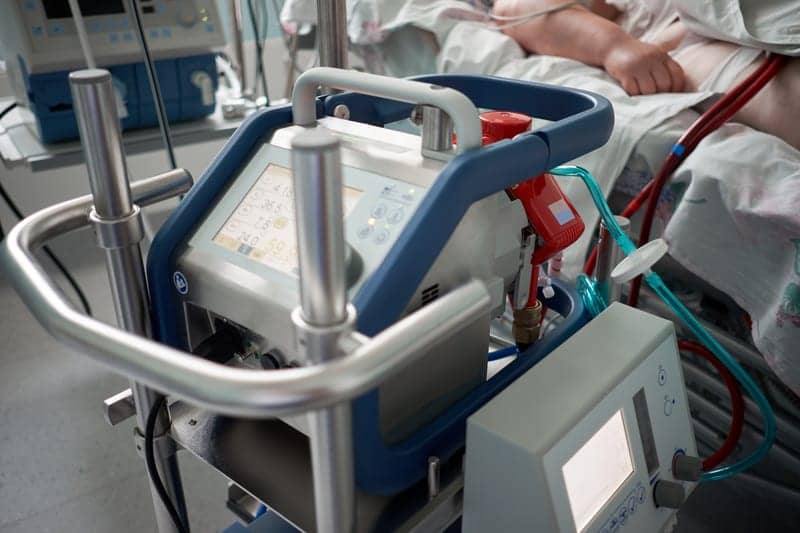
Some patients with severe COVID-19 who are treated with extracorporeal membrane oxygenation (ECMO) may experience significant lung recovery and return to normal lives with “meaningful” long-term outcomes, according to research published in The Annals of Thoracic Surgery.
“Our work suggests that with appropriately selected patients and aggressive management strategies, the use of ECMO support for severe COVID-19 can result in exceptional early survival, and these patients who leave the hospital without the need for oxygen therapy are very likely to remain alive and well one year later,” says Deane E. Smith, MD, from NYU Langone Health in New York City.
Smith and colleagues identified 415 patients who were admitted to the intensive care unit (ICU) of NYU Langone Health from March 10, 2020, through May 1, 2020, with confirmed COVID-19 infection. Of these patients, 30 (7.2%) received venovenous (VV) ECMO—an advanced life support machine that takes over the function of damaged lungs.
Most of the ICU patients—323 (77.8%)—were intubated for mechanical ventilatory support. However, according to Smith, the ventilator may damage the lungs further and “create a vicious cycle” for patients with severe lung disease or damage who are intubated. In some cases, VV-ECMO may result in decreased support from the ventilator, minimizing damage to the lungs and allowing them to begin healing. Thus, 80 patients (19.3%) were evaluated for VV-ECMO, with 30 (7.2%) eventually receiving it.
“These patients received ECMO for severe COVID-19 during the height of the pandemic in New York City—at a time when very little was known about the likelihood for success,” says Smith.
The researchers reported that 28 patients (93.3%) survived VV-ECMO. These patients were hospitalized for a median of 45 days and supported on VV-ECMO for a median of 19 days. Importantly, 27 patients (90%) were discharged home or to acute rehabilitation. No patients left the hospital dependent on a ventilator, and only one patient required supplemental oxygen.
According to Smith, patient selection was a significant factor that impacted the success of VV ECMO. The selection philosophy was that this was not a “bailout” or salvage therapy to be employed in the absence of other options. Instead, VV-ECMO was offered to patients believed to have a reasonable chance for survival with this support.
“We were struck by the number of young, otherwise healthy patients who were dying from the disease. Because of this, we felt patient selection was very important,” he says
Smith further explained that the decision to offer ECMO support also was impacted by the severity of lung disease and potential for survival.
“If there was one theme throughout our experience, it was how we would define success. We did not feel that using ECMO to have patients survive simply to go to long-term facilities debilitated and vent-dependent was successful, or not as successful as it could be. In other words, we began with the end in mind,” Smith says. “If we were going to offer patients ECMO for severe COVID-19, it was because we believed that we could protect the lungs and allow patients to return to their normal lives at the end of it.”
While patient selection was important, a standardized approach to patient management and protecting the lungs was equally valuable. This included: not deviating from lung protective ventilation strategies, early tracheostomy (an opening surgically created through the neck into the trachea) and frequent bronchoscopy (a procedure to look directly at the airways in the lungs using a thin, lighted tube), treatment of coinfection, and standardization of an anticoagulation regimen (to help prevent blood clots).
In addition, to help improve oxygenation, the team frequently positioned patients who were not recovering as quickly as expected on their abdomens, also known as “proning.”
“It’s worth noting that most of these things such as bronchoscopy or tracheostomy were not considered safe in patients with COVID-19 at the start of the pandemic,” says Smith. “Our team was aggressive with these interventions much earlier than most hospitals.”
Importantly, at a median follow-up of 10.8 months since the patients were treated with VV-ECMO, survival was 86.7%, including one patient who underwent lung transplantation. A 6-minute walk test was performed in 16 patients (59.3%) with a median value of 350 meters, which the researchers called “encouraging.”