
John Noblitt, MAEd, CBET
This article will continue the discussion on infusion management devices and the knowledge base that test takers should possess to do well on the CBET exam. You can read the first installment in the “ICC Prep” column in the August 2012 issue of 24×7.
Different pump manufacturers can use different pumping mechanisms to achieve the delivery of fluid to the patient with a specific type of infusion “set.” These “sets,” or patient tubing and cassettes, will differ by each manufacturer to some extent, but all deliver controlled amounts of fluid when activated by the pumping mechanism. These tubing “sets” are specific to each unit as they are manufactured to tight tolerances to ensure alarms will activate at proper levels, such as occlusion alarms or air-in-line alarms.
Improper tubing, such as tubing with a smaller internal diameter than it was engineered for, can result in underinfusion. Tubing that is too rigid or has a larger outside diameter can result in a condition known as free flow, which is an overinfusion state. Air-in-line detectors ensure no air embolus can be delivered to the patient. This alarm will usually use ultrasound or optics to detect large air bubbles. Without the proper tubing, this alarm may be compromised. These simple facts about tubing may very well be asked on the CBET exam, as the exam seems to be leaning more toward questions about the practical applications of medical devices.
Occlusion Alarms
Occlusion alarms are designed to alert the medical staff the solution is not being delivered to the patient. This alarm is activated once a predetermined pumping pressure is reached and the pump mechanism is shut off. This usually happens when the patient’s catheter/cannula comes out of the infusing vein and the unit continues to pump solution into the site until the pump senses pressure in the tubing set. This occlusion pressure is generally different from one manufacturer to another. Different pumps may also have occlusion pressure alarms, which can be reprogrammed into the unit to adjust for different types of patients, such as neonatal, pediatric, or adult. Occlusion pressure alarm testing needs to include distal and proximal testing. For example: the older Plum XL units have a distal occlusion pressure alarm set at 10 psi +/- 1.8 psi (1 psi = 51.7148 mm/Hg), and the proximal occlusion alarm should activate within three pumping cycles after the tubing has been pinched off or occluded. Neonatal pumps may have an occlusion pressure set as low as 50 mm/Hg.
When considering occlusion alarms one must consider the pressure that is inherent to the tubing system and the human body. For example: To deliver an electrolyte solution to an adult through a 16G, 9 cm cannula at 100 mL/hr, the pressure the pump must overcome is approximately 141 mm/Hg. This number comes from the inline filter, which creates 10 mm/Hg, the cannula produces 100 mm/Hg, administration set 1 mm/Hg, and the maximum adult venous pressure of 30 mm/Hg. In contrast, a pump set up for neonatal operation has to overcome a much lower inherent pressure such as 22 mm/Hg. This comes from the maximum venous pressure of 10 mm/Hg, filter 1 mm/Hg, cannula 10 mm/Hg, and administration set 1 mm/Hg for the total of 22 mm/Hg.
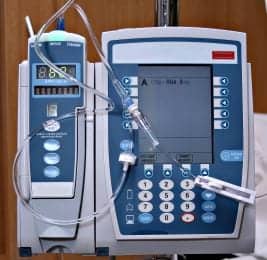
Delivering Solutions
Many of today’s pumps have an ability to deliver solutions from two bags, which is referred to as “piggyback” infusion. This type of infusion allows one pump to deliver solutions from the piggyback bag. Once that solution has been administered, the pump will begin infusing the primary solution. Care should be taken when this procedure is implemented, as the piggyback solution must be estimated as to the volume to be infused—or VTBI. Once the VTBI is reached, the unit begins administering from the primary solution bag.
Feeding pumps are used to administer nutrition to the patient when they are unable to feed themselves or tolerate food. Feeding pumps, which administer nutrition to the stomach via tubing inserted into the nasal cavity, are common in long-term care facilities. Many of these types of units use the rotary peristaltic delivery method. The other type of feeding pump is a standard infusion pump, but a PICC—an abbreviation for peripherally inserted central catheter—line is inserted into a major blood vessel and is usually performed on patients with extended stays in an intensive care unit. Clinicians deliver nutrition through the PICC line.
PCA pumps, or patient controlled analgesic pumps, allow the patient to determine the amount of pain relief medication administered. However, the amount of each dose and the time between each dose is programmed into the unit by the clinical staff so the patient cannot overmedicate. These syringe-type pumps have a locking mechanism (usually a door), which will not allow patients or visitors to access the solution being administered. PCA pumps will have a memory log to document how often the patient calls for medication. If the patient still complains of pain, the clinical staff can review the memory log and adjust delivery amount or time between doses allowed. Clinicians can program PCAs for continuous infusion, known as basal rate, or a basal rate and a bolus on-demand amount.
I hope you find this information useful, and best of luck on your certification journey.
John Noblitt, MAEd, CBET, is the BMET program director at Caldwell Community College and Technical Institute, Hudson, NC. For more information, contact .
Review Questions:
- While performing output verification tests on infusion management devices, you notice each unit is underinfusing. What is your most likely problem?
- Tubing is too long.
- Tubing is too rigid.
- Tubing diameter is too small.
- Tubing diameter is too large.
- When piggyback administration is being used with infusion devices, the most critical programming of the device is the_______________?
- Basal rate
- Occlusion pressure
- VTBI
- PICC
- What type of infusion management devices allow the patient to control the delivery of their solution?
- A feeding pump
- A PCA pump
- A piggyback pump
- A rotary peristaltic pump
- Occlusion pressure alarm measurements are made where, in relationship to the pump?
- Distal
- Proximal
- Internally
- No such measurement exists
See the answer
See the answer
See the answer
See the answer



