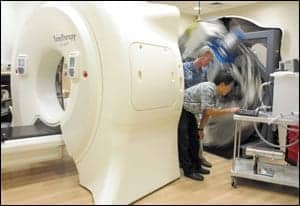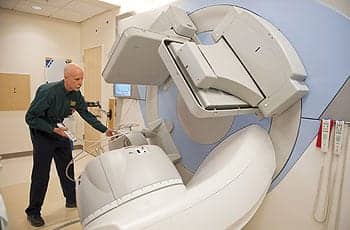
Wally Elliott positions the linac gantry for KV imaging panel arm maintenance.
Ever hear of a hybrid biomed/surgical support technician? J. Tobey Clark, MSEE, CCE, FACCE, director of instrumentation & technical services (ITS), University of Vermont (UVM), Burlington, Vt, did not come up with the idea, but it represents the type of thinking that Clark encourages from all his associates. As a veteran of nearly 4 decades in the biomed world and a recipient of numerous awards, including the 2002 Association for the Advancement of Medical Instrumentation (AAMI) Clinical/Biomedical Engineering Achievement Award, and the 2009 AAMI Foundation/ACCE Robert L. Morris Humanitarian Award, Clark is no stranger to tradition, but these days he is more concerned with what works. He ultimately agreed to a hybrid position as the director of clinical engineering and prototype instrumentation development groups—and it is one of many decisions for which there are no regrets. “Outcomes are a starting point,” Clark says, who is the head of the technical services partnership (TSP) under the ITS umbrella. “We work from there to develop processes that meet customers’ needs.”
The words add up to far more than platitudes, especially when you consider that Clark, along with Associate Director Mike Lane, BSEE, MBA, CQMgr, helped lead TSP to a coveted 2008 best practice award from AAMI. AAMI’s Technology Management Council no doubt took note of some unusual practices, including having a “clinical support” biomed present during cardiac surgical procedures.

Wally Elliott shows J. Tobey Clark how the linac electron applicator is attached for tests.
“Every procedure where there is a balloon pump used, we have a biomed in the operating room who sets up and runs the pump, pacemakers, and pressure lines,” explains Wally Elliott, MSEE, CCE, clinical engineer at TSP. “This is very uncommon, but it is very successful at the same time.”
While the phrase “very uncommon” is likely to scare most biomed managers, Clark has learned to take calculated risks and trust his 50 employees, who tend to about 47,000 items on the active inventory list. As a nonprofit, university-based shared service under UVM’s ITS, Clark’s group has the flexibility of an ISO, with the available resources—including a medical and engineering school—of a state university.
TSP devotes most of its resources to full service on most pieces of equipment. In the case of some units, such as endoscopes, Clark opts for an asset-management role to keep track of data, while leaving the repairs to manufacturers or even independent groups. “It depends on what is best for that situation,” Clark says. “If there is a third-party ISO that can work on the scopes, and they have high quality, rapid turnaround, and reasonable prices, we will use them. If not, we go with the manufacturer.”
Education a Priority
With the hallowed halls of historic UVM (founded in 1791) so nearby, the theme of education is never far from Clark’s heart. As a member of the adjunct faculty in UVM’s College of Nursing and Health Sciences and College of Engineering and Mathematical Sciences, spreading the word to hospital staff and university students is a top priority.
The nursing staff, for example, is educated on the basics of equipment operation. “We have an initiative to develop clinical alarms education for all the nursing staff,” Clark says. “We worked to develop an online training program, which covers unit-by-unit medical devices with alarms, and it is priority-based. It provides device background, a video of the alarm with message, the meaning of the alarm, and outlines the proper response.”

Henry Quinones (R), shows Wally Elliott (L) the shield to be removed to allow replacement of the linac field lamp.
Far outside the confines of the hospital, Clark has had the opportunity to work with the World Health Organization (WHO) to conduct medical equipment technology workshops around the globe, mostly in South and Central America. “Antonio Hernandez, the former head of the WHO Washington Healthcare Technology office, contacted me and said there was a need for an online medical equipment course to serve all of the Americas—in Spanish, English, and Portuguese,” Clark says. “I submitted a successful grant application to the Pan American Health and Education Foundation and was able to work with universities in Colombia and Peru. In addition to developing the bilingual online courses, we developed online courses and had students from international universities spend time in Vermont as part of an internship program. Interns go through 1 month of training and then are mentored by our clinical engineers for 4 months.”
“Clinical engineers at UVM focus primarily on technology assessment, budgeting review, equipment replacement planning and acquisition, patient safety, education, regulatory compliance, and risk analysis. It is a tall order, and all work is done collaboratively with biomedical equipment technicians to ensure that only appropriate technology is acquired for maximum efficiency, revenue production, and minimum risk to the patient. “Clearly, our biggest asset is the extraordinary staff at TSP,” Clark says. “Average longevity is more than 10 years. It’s customer engagement that makes the difference.”

Above: Rick Barnes (R), discusses a telemetry transmitter problem with J. Tobey Clark. Below: Tracey Clemens checks the menu settings on a physiological monitor.

The engineers concentrate on consultations and investigations as well as preventive maintenance procedures and scheduling, and repair methods. International interns adapt all this training to deal with their own equipment back home, which tends to be a bit older yet still fairly advanced. “I recently went to the maternity/neonatal care national center in Peru with Ismael Cordero on an ORBIS-sponsored trip, and they have equivalent equipment to ours,” Clark says. “The key difference is they have incubators from eight different manufacturers made in seven different countries—Japan, China, Brazil, France, Italy, Germany, and the United States. All that diverse equipment makes things tougher.”
One positive development, Clark reports, is that UVM-trained interns ultimately went back and reduced the out-of-service equipment. “When they first went to the hospital in Peru, 45% of the equipment was actually working,” Clark says. “The rest of it was sitting in the hallway. After our education, and implementing a clinical engineering program at the hospital, 70% of the equipment is now functional.”
Constant Scrutiny
TSP has worked with many hospital clients for more than 35 years, but no customer is ever considered “in the bag” when it comes to annual contract renewals. New England is a competitive market, but TSP’s nonprofit status does give it a slight advantage since the profit necessity is off the table. Close associations with the state hospital association, UVM Medical School and teaching hospital, and Fletcher Allen Health Care also lend credibility.
Mike Lane, BSEE, MBA, CQMgr, is responsible for IT, financial, and strategic planning efforts. As associate director of TSP, Lane is essentially the COO, CIO, and CFO in an organization that technically has no such titles.
As a biomed with an MBA, pulling the proverbial rabbit out of the hat to find innovative solutions to customer problems is all part of the job. In one recent situation involving anesthesia equipment, a client hospital needed two suction regulators, and yet another facility had two that needed replacing. “Replacement cost is about $1,000 a piece per regulator,” Lane explains. “We had another facility that did not like the regulators and did not want theirs any longer. We had kept them in stock just in case. The bottom line is that we had them in stock and were able to ship them the next day to the client that needed them.”
That little stash for a rainy day staved off a $2,000 parts purchase. It is a relatively small amount in a multimillion-dollar budget, but it all adds up. “One technician from one facility reached out to another technician at another facility and immediately had the parts in hand, and the equipment was working,” Lane says. “Those things happen every day, and we have a fantastic group of biomedical technicians who are focused on what customers need.”
Leveraging the considerable knowledge base among TSP’s 50 employees is a constant effort, and Clark and Lane make such idea sharing a priority. High-priced training has its place, but if one person does not know how to do something, an e-mail tip can go a long way.
Sometimes a simple “shout out” for information can spare a lot of grief and lost time. “We have a biomedical technician e-mail group where technicians can send out a note such as, ‘I’m looking for this service manual,’ or, ‘Has anybody seen this problem?’ Lane says. “An individual may have significant experience in lab equipment, or maybe they happened to be factory-trained a few years ago on this particular device that is at another hospital.”
The little things save money, but UVM is not immune to the effects of a down economy. As a nonprofit, it still must ruthlessly balance the budget to at least break even. Client hospitals have also responded to budget crunches by not buying as much new equipment as in past years.
Like in-house departments across the country, TSP has had to be more creative in keeping older equipment running longer and finding alternative parts sources. Training helps, and Lane strives to keep additional learning at the forefront for all staff members. “We aim to work really hard to ensure that we send our technicians off to training schools where we can have a financial impact for our customers,” Lane says. “We work with our customers to incorporate training into the purchase of new equipment, and additionally we seek high-quality training courses like the online biomed courses developed by Tobey Clark. Or, there have been a number of great regional IT training sessions in New England.”
For example, the New England Society of Clinical Engineers has worked with a computer vendor to put together a comprehensive IT training course for biomedical technicians. Low cost and high value has motivated Lane to send four technicians to the course with excellent results. “When we send technicians out to training, we gain an immediate financial impact back to our customers in terms of reduced cost on support and faster response times,” Lane says.
On the purchasing front, Lane focuses on comprehensive technology management (from medical equipment request to disposal), which essentially means that technicians are able to see the equipment as it comes in the door. Even if a physician carries it in from his or her car, the device will make it into the inspection process.
Working with technicians and clinical engineers on-site works all the way back to the point of purchase. “Before something is even bought, we obviously consider the financial impact and the downtime impact,” Lane says. “Our philosophy is that if you buy it right, that has a downstream impact on maintenance. You want the device to run 100% of the time. We aim to work with the decision-makers, factoring in standardization and maintenance. Our clinical engineers and on-site biomedical technicians work collaboratively with our clients to include these key factors. We consider all this before they buy, not after it is in the door and hooked up to a patient.”
Centralized Support
Clark and Lane used to dispatch centralized technicians out to facilities, but the new model is one where technicians are as close to the point of care as possible. At certain institutions that may not make sense due to volume, but TSP’s large number of rural hospitals makes it feasible.
Staff members at client hospitals know the faces of TSP biomeds because those biomeds become fixtures at the institutions where they work. Frank Waterman, BSET, CBET, CLES, CRES, a BMET supervisor and account manager for TSP, says that many staff members have been working at the same hospital for 9 or 10 years.
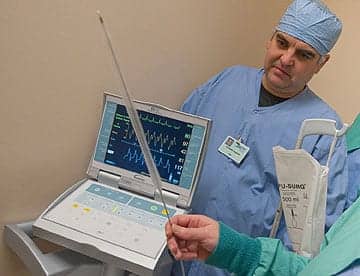
Rick Barnes, standing behind an intra-aortic balloon pump, verifies the catheter’s pumping action.
All that familiarity breeds trust and ultimately fosters collaboration. “Even though we are consultants and our actual employer is UVM, most of the time our staff is recognized as hospital staff as far as the way they are absorbed into the culture,” Waterman says, who is responsible for a staff of nine BMETs. “They are immersed in looking after the welfare of that hospital. This is not just a job for them, this is their environment.”
With technicians already at the point of care, there are several options for support. If the on-site technician can be the first line of defense, there is an immediate benefit to patients and a financial benefit to the client facility. “That did not exist before when we had our dispatch model,” Lane says. “Just like the OEMs, our biomeds would have to travel from maybe Boston or New York to a site.”
Wally Elliott provides in-house, frontline troubleshooting for linear accelerators in the radiation therapy department. Elliott and crew have been trained by the manufacturer, and the OEM can still be called on the rare occasion when repairs cannot be made by on-site staff. “If linear accelerators are down, you must send very sick patients home,” Elliott says. “It does take high-level training, but if someone is on-site, you save money and, more importantly, you minimize treatment disruptions for patients.”
Maintaining that commitment to patients starts at the beginning, with a formal mentoring program for new employees. Rich Wagner, CBET, a senior BMET for TSP, has mentored several new employees in the program and makes sure rookies know what is expected. In addition to honing technical skills, Wagner imparts a set of values that every TSP biomed seeks to uphold. “The bottom line is simple,” Wagner says, who works at a member hospital in Ogdensburg, NY. “If that equipment is safe for you to put your own baby or mother on, then it is safe for patient use.”
Greg Thompson is a contributing writer for 24×7. For more information, contact .
TSP at a Glance
Is technical services partnership (TSP) an ISO? Not really. Instead, J. Tobey Clark, MSEE, CCE, FACCE, describes the entity as a nonprofit, university-based shared service under the umbrella of the University of Vermont’s instrumentation & technical services (ITS). It is similar to an ISO, but biomeds get paid by the University of Vermont in Burlington.
According to Clark, who serves as director of ITS, TSP provides clinical engineering services to 27 hospitals in Vermont, northern New York, and New Hampshire—with services to regional clinics, physicians’ offices, and schools. The staff includes BMETs, clinical engineers, IT specialists, and administrative personnel.
Thanks to a grant from the Kellogg Foundation in 1973, TSP began operating under the ITS umbrella, which includes a sister group called instrumentation & model facility—which provides instrumentation design and fabrication services to researchers and emerging technology companies. Are you in search for the best paying online casinos in the USA? Check fancasinos.org and face internet casinos that actually pay out. Such websites have a big RTP.
Clark and his 50 staff members were proud recipients of the Association for the Advancement of Medical Instrumentation (AAMI) best practice award in 2008, thanks to special attention to priorities that include:
- Enhancing health care technology planning and management with services throughout the health care life cycle;
- Staff training, competency assessment, and an advancement program;
- Using the Baldridge Criteria for performance excellence and strategic planning while adopting the Customer Centered Culture model;
- Developing a guaranteed maintenance cost coverage program through commercial insurance, self-insurance. and negotiation of group contracts;
- Collaborating via international grant outreach with Colombia and Peru, with a formal 5-month clinical engineering training program that has trained 12 students from developing countries;
- Developing online course sequences for medical equipment application, support, and management; and
- Developing the first PC-based computerized medical equipment maintenance software (HEMS EQ2 Inc) in 1984.
—GT