 |
Many clinical engineering departments have struggled with determining the appropriate staffing levels for their particular health care facility. Increasingly, hospital administrators prefer to utilize benchmarks when measuring the need to adjust staffing for a clinical department. Unlike our colleagues in the respiratory care and nursing professions, there have been no widely accepted or accurate models to determine appropriate staffing for clinical engineering departments.
There have been a number of rules of thumb or averages that have been reported and used for many years. One such approximation is one BMET per 1,000 pieces of medical equipment. Other approximations include 2.6 full-time employees (FTEs) per 100 beds, as reported in the December 2006 article in 24×7, “Are You Benchmarking Yet?” by Maria Fotopoulos.
From data acquired from 253 hospitals, Binseng Wang1 reported that the average staffing from the surveyed group of facilities was 2.5 biomed FTEs per 100 beds.
These models fall apart when they are applied to individual health care facilities. Some of the problems with these formulas include failing to account for the widely varying support practices of clinical engineering departments. Does your department support imaging, CT, MR, and laboratory systems in addition to the standard biomed equipment?
Does your department support nurse call, patient beds, stretchers, PC and network equipment, telephones, televisions, and sterilizers?
Is your department providing technology assessment services, building equipment planning, product evaluations, incident investigations, and research?
Does your department cover only one facility, or are you responsible for multiple sites, freestanding clinics, and diagnostic centers?
Some clinical engineering departments manage the central equipment distribution departments that distribute IV pumps, etc.
Clearly, each clinical engineering department has unique responsibilities that could lead to different staffing needs. For example, a 500-bed hospital by the above formula should have (500÷100 x 2.5) = 12.5 FTEs. Is this the correct number? Perhaps, but some other variables need to be considered. ICU beds require a much higher level of support than general med/surg units. OR suites do not count in the hospital bed number, but typically have some of the highest support needs. Likewise, the number of devices to tech ratio works only if you are looking at large numbers of similar devices, such as IV pumps and feeding pumps. When systems such as CT scanners, linear accelerators, and catheterization labs are added to the inventory, the old models do not work.
Another variable is freestanding diagnostic centers that may include emergency treatment areas as well as diagnostic imaging, outpatient surgery, and laboratory services. By the bed-to-FTE model, these locations contain no “beds” and therefore do not add to the FTE count.
One solution is to consider “care delivery locations” rather than licensed beds. Emergency-department treatment stations, ORs, imaging suites, observation beds, and dialysis stations can all be equipment intensive locations. Adding these locations to the licensed bed count may be one technique to equalize the FTE calculation. (See the chart below, column 1. You can download an editable copy of this MS Excel spreadsheet here.)
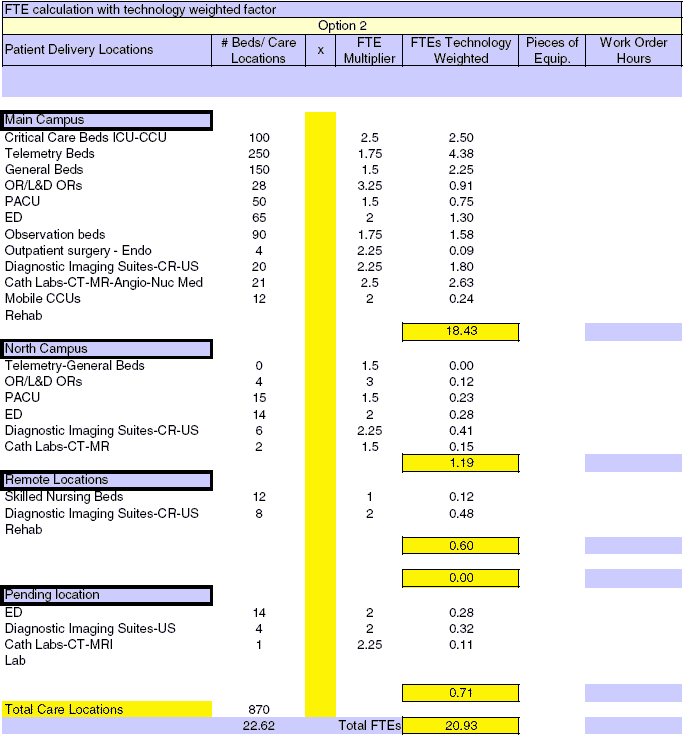 |
| You can download an editable copy of this MS Excel spreadsheet here. |
Another option to further refine the updated model is to adjust the FTE multiplier based on the care area. This allows a higher weight for an OR or ICU location as compared to a med/surg bed. The chart/spreadsheet allows the FTE multiplier to be adjusted from 0 to 4, depending on the level of involvement of the clinical engineering staff.
The included chart shows an example of how this formula may work. The multiplier can be adjusted based on the level of service provided. For example, a first call contract for ultrasound equipment would utilize a lower number than if your department provides complete service. The model allows clinical engineering management to tailor the staffing needs based on equipment-specific support levels. In addition, the model gives clinical engineering management an easier method to calculate the additional FTEs for new locations, or as equipment transitions from warranty to other support modes.
Perhaps if a number of clinical engineering departments would compare the model to their current staffing, some norms could be developed for the FTE multiplier. An accurate FTE staffing tool that allows clinical engineering departments to account for the unique services that their department provides would be beneficial to every facility.
Gary A. Evans, MS, CCE, is director of clinical engineering, WakeMed Health & Hospitals, Raleigh, NC. For more information, contact .
Reference
- Wang B. Clinical engineering benchmarking: An analysis of american acute care hospitals. J Clin Eng. 2008;33(1):24-27.
What’s on Your Mind?Got a gripe? A recommendation? Does someone or something deserve praise? Share your opinions and insights with your peers. Soapbox columns should be 700 to 750 words in length and can be e-mailed to . |





