A new negative pressure ventilator which could provide additional treatment options for patients with respiratory failure, including those with COVID-19—and whose design can be easily adapted to developing countries—has been created by a team that includes anaesthetists, nurses, and engineers. Details on the new exovent system—which is similar in design but much smaller in scale and easier to use than the devices used to help treat polio patients during the 1950s—are published in Anaesthesia.
Use of this system would offer more comfort to patients, who would not need to be asleep or have an artificial airway in place, although the authors make it clear that a clinical trial is required to fully test it. After monitoring patients closely at first, the system would also mean less nursing care and could be used anywhere in the hospital, and even potentially at home. Staffing requirements for the new system would be typically much lower than for today’s typical intensive care unit ventilators, and lower than other non-intensive positive pressure systems for the equivalent severity of illness.
Negative pressure devices lower the pressure outside the body to allow lung tissue to expand and function in a way that is like normal breathing, while positive pressure devices such as the conventional ventilators and continuous positive airway pressure (CPAP) systems in current use push air into the lungs under positive pressure. Research into negative pressure devices had been mostly abandoned since the 1950s, since positive pressure devices had become much smaller, cheaper, and more convenient.
The exovent task force formed in March 2020 in response to the COVID-19 crisis, inspired by calls from the UK Government for rapid innovation to combat the challenge presented by SARS-CoV-2. The team is composed of anaesthetists, critical care consultants, nurses, medical clinicians, engineers, academics, scientists, and manufacturers. This initiative was not part of the UK’s ‘Ventilator Challenge,’ because that project encouraged innovation for positive pressure devices only.
“The exovent team focused on exploring the benefits of negative pressure ventilation, founded upon lessons learned from nearly 100 years of using negative pressure ventilation, most memorably during the polio epidemic of the 1950s,” explains co-author Dr Malcolm Coulthard, BSc, MB BS, DCH, FRCP, FRCPCH, PhD, of the Translational and Clinical Research Institute, Newcastle University, UK.
Use of negative pressure is far less intrusive and much more like normal breathing than either positive pressure ventilation through a tube inserted into the windpipe, or delivering CPAP via a tightly fitting face mask. The exovent system is non-invasive, which means that patients do not need to have their windpipes intubated, so they don’t need to be anaesthetised and oxygen can be delivered in the form of a normal oxygen mask or nasal prongs rather than through a high-flow oxygen device that puts hospital oxygen supplies under pressure. Patients remain conscious, and can take food and medication by mouth, and talk to loved ones on the phone.
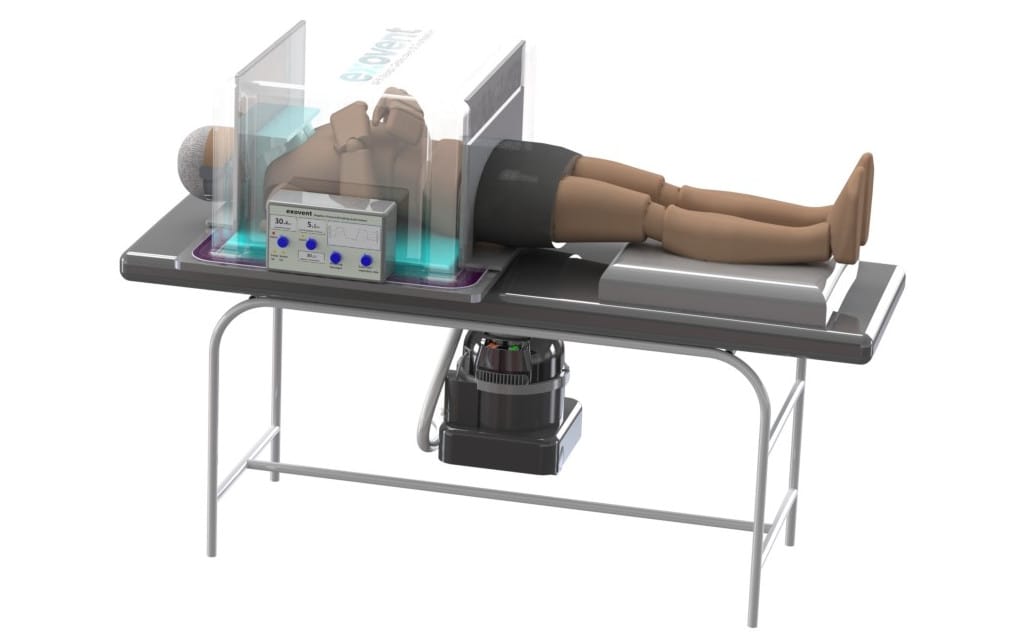
The exovent chamber consists of a base fitted onto a standard hospital bed that contains its own section of mattress and a removable top that fits over the torso with neck and hip seals. A free-standing pump unit is connected to the base by flexible hoses and a control unit allows adjustment of pressure around the torso. The subject’s torso can be observed through a window and accessed through portholes that seal around the healthcare provider’s arms. The thin neoprene neck and hip seals are fitted loosely onto the person before the chamber being put in place, and then adjusted.
Testing was performed on six healthy adult volunteer members of the development team in the presence of three senior anaesthetists. All of the subjects were tested in the supine position (facing up) and slightly tilted up, while three were also tested in the prone (facing down) position. Various negative pressure settings were tested and spirometry (lung performance) readings recorded. These showed that the exovent was able to deliver both an increased lung expansion to people breathing spontaneously, and powerful ventilation to take over people’s breathing entirely, using only moderate negative pressures.
Nurses reported that the exovent chamber could be positioned and removed quickly by two people. They noted that the window and portholes would allow them to monitor and look after their patients safely, despite the inevitably reduced direct access to their torsos. When supine, the subjects’ heads could be positioned easily to allow view of the larynx for tracheal intubation, should that become necessary, without needing to remove or adjust the neck seal. For patients that progress to needing intubation, it would probably not be necessary to keep them in the exovent (though it would be easy and safe to do so)—and in the event of an emergency intubation, there would be no need to delay while the exovent was removed.
The volunteers all found the chamber comfortable, and in particular reported that the neck and hip seals were soft and easy to adjust, and that they could voluntarily breach them to stretch their arms or touch their faces without this significantly affecting the stability of the chamber pressure.
Importantly, all the test subjects felt ‘in control’ knowing that they could immediately release the vacuum by opening a wide gap under one of the seals if they wished. When the ventilation mode was used, the subjects all allowed the exovent to take over their breathing without feeling any desire to ‘fight it’ or that it felt unnatural or uncomfortable, and described the sensation as relaxing; one participant fell asleep within minutes.
“We are really excited to be unveiling this life-saving system which is a cutting-edge reinvention of pre-existing technology,” says exovent CEO and article co-author Ian Joesbury. “As the patient does not need to be sedated it opens up alternative treatment options that may allow more patients with COVID-19 to be treated outside of intensive care.”
It is estimated that the UK version of the exovent will cost approximately £8000 GBP (US $10,496, €8856), which is considerably cheaper than existing positive-pressure devices, which cost around £15,000 GBP for CPAP and over £30,000 GBP for intensive care ventilators. It is also estimated that a lower-cost global version of the exovent could be produced for less than £500 (US$652, €550).
The authors add: “Anticipated advantages of the exovent over positive-pressure ventilators, which may be especially relevant in low- and middle-income countries, include the lower resources required to ventilate conscious patients, and the potential for greater oxygen conservation, since oxygen would only need to be supplied to the patients directly via a facemask or nasal prongs when required, rather than the continuous oxygen supply needed for positive pressure systems.”
They explain that because it is so much less invasive and so much easier to do than PPV, the threshold for using exovent when available will be much lower, and many more patients will be eligible for therapy. Even if hospitals in low- and middle-income countries have conventional intensive care ventilator hardware available, the resources required to (a) intubate, paralyse, and sedate them as is necessary, and (b) to manage them whilst unconscious which means intensive nursing, intravenous nutrition or tube nutrition, skin care, etc., are too scarce to make intensive care ventilation available to any but a very few individuals. The authors explain: “It is about staffing more than equipment, and the exovent would be much easier and less expensive to use.”
Thanks to the investment of over £1m of volunteer time from the exovent team, rapid development and prototyping by Marshall ADG, and partnership with Warwick Manufacturing Group (WMG) High Value Manufacturing Catapult, the system is now ready for a formal assessment and approval. The authors plan to submit the design to the Medicines and Healthcare products Regulatory Agency (MHRA) which regulates medical devices in the UK, and hope to receive approval by the middle of 2021.