All photos courtesy of Mark Brideson
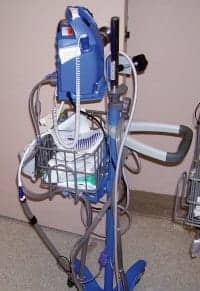
Photo 1. Eliminating tangled cables, hoses, and power cords will enable units to move easily from room to room and will help prevent damage.
In any fast-paced hospital environment, clinicians’ minds often focus on the patient’s care and the time it takes to deal with the care issues for each and every patient. There is little or no time to deal with the technicalities of the equipment involved in the care of that patient. This is especially true when census is high and staffing is low. This dilemma is a common occurrence and can result in equipment getting damaged because of a hectic pace.
As clinical/biomedical engineers, we often have to deal with equipment damage. To some extent, one could call dealing with this damage our job security. It is our job—and not just our job security—to keep equipment in good condition for everyone and ready for use at a moment’s notice. In the fast-paced hospital or medical clinical environment, reporting equipment issues is often vague, it is not passed on to the charge nurse or to the biomed department, or it is not reported at all. Too often, a staff member is embarrassed because an issue was caused by carelessness due to being in too much of a hurry. This hurriedness sometimes leads to creative tape or rubber band jobs on SpO2 sensors. Then, department managers (telemetry, medical surgery, emergency department, etc) wonder why there is a high incidence of smashed or broken pulse oximeters, damaged NIBP tubing or cuffs, or why EKG machine or monitor clip leads are bent or do not have proper contact due to some form of damage. Of course, the clinical staff may say they do these types of quick fixes because they did not have time to pick up the machine off the floor so the gurney would not run over it, or time was an issue.
I have encountered situations when all spare equipment was made useless because of a lack of reporting damage. Consequently, we get called in after hours or into a meeting to explain why few (or all) of a unit’s equipment is not working. My point in writing this is to share a practice I refer to as “the parachute principle.” Good patient outcomes and proper care require reliable, 100% functional equipment, and it is our duty to make this happen. When equipment is grabbed for use, it should function as if a life depended on it—which it often does. Just as if you jump out of a plane wearing a parachute, it should function as it is designed to in every way—whether it’s base jumping, just for fun, or an emergency bailout.
A Safe Holding Pattern
Here we will discuss a good practice to start with: finding out what can be done to ease the time it takes to return accessories back to a “holding pattern” so they are ready for use for the next patient, emergency or not.
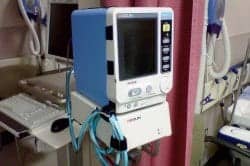
Photo 2. Using zip ties or Velcro can keep cables, hoses, and power cords from getting tangled and will help make the clinician’s job a little easier.
The first thing we can do is to create a habit of making rounds once per day. Larger or smaller departments can divide these rounds, based on staffing time and equipment involved. These rounds also may jog the staff’s memory about the intermittent pulse ox or the defibrillator that is not recharging for its next use, the NIBP unit that sometimes does not take a reading, the battery on a portable monitor that only lasts for two out of the 10 rooms where it is needed for the vital signs intervals, etc. It will also build the clinical staff’s confidence that their biomed staff exists and is willing to take care of any problems or potential ones. This routine will decrease the emergency calls and stress levels, and it will encourage the prompt reporting of issues that could get ugly. Speaking of ugly, the daily rounds will help biomeds spot potential or actual problems, which they can then attend to before they fester.
Untangling for Mobility
Another necessary step relates to portable vital signs units: eliminate the tangled-up SpO2 cable, NIBP hose, and power cord. The unit should be able to easily move from room to room and not be a burden to the staff or the biomed department, or eventually become nonfunctional for the patient. This is not easy when it looks like a “cat’s cradle,” as seen in photo 1. Two methods can help you untangle this. In the first way, use zip ties to lash the SpO2 cable and the NIBP hose together, except for the last 2 or 3 feet (photo 2). Since the clinician always takes these two measurements on the same arm, being tied together to that point will not represent an issue. This reduces the tangling potential quite a bit.
On the joined cable and hose there are two options that I have found work the best: one using Velcro and one with zip ties. Use the one that best suits you.

Photo 3. The Velcro method joins items and can attach to the top of the unit. Make sure cords do not drag on the ground or become a tripping hazard.
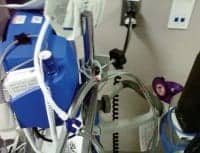
Photo 4. By making a loop with the zip tie method of containment, you can hang the loop from the IV-style pole they might attach to.
The Velcro method uses a cut tab from a roll of Velcro that has an adhesive backing. Place a tab of the soft Velcro around the NIBP hose of the two joined items in two or three evenly spaced areas (also shown in photo 2) so it leaves a “tail” so it can join the bristled Velcro on the side of the unit. Do this by leaving a tab that folds over on itself so it may attach to the bristled Velcro on the side of the unit at three selected areas (photo 3). Then use two bristled Velcro tabs on top of the unit (one for the SpO2 and one for the NIBP cuff and/or end of hose, shown again in photo 3). The spacing should be enough so it does not drag on the ground or become a tripping hazard, but do not use too many tabs. Remember: The easier to use, the better.
Zip Ties
Another method of containment involves using a medium-thick zip tie to make a loop, and placing the chosen method in no more than two or three areas. On this zip tie loop, cut a slight portion of it so it makes a stop (photo 4, page 23), so it won’t fully constrict. Then, attach it to the NIBP hose via a small zip tie. You can hang these loops from the IV-style pole they might attach to, or maybe you can make your own hook (also photo 4). This method also works on the power cord (on a different hook) to keep it out of the way, if desired. In any case, the less tangling the better to enable the easy movement of the device from room to room.
Obtaining Buy-in
One more step, and it may be a difficult one, involves getting the clinical staff used to this new method of operation. Some will take to it just fine, while others may resist it and stay with their own ways and leave it tangled up. However, it is easier to untangle than it was before using these methods. If you do your daily rounds, you will definitely notice this and you will find it is very easy to put the cable and hose back to an organized configuration, now that you have reduced the tangling potential. I personally do this on rounds, and after practicing this for 2 years, most of the long-term staff comply nicely. For those who resist the change, if they see it and try this method, they will find it will make their jobs a little easier.
I hope this concept is helpful to all who read this. I have found it improved staff morale, made them more likely to report issues, and helped them focus more intently on the patient’s care, whether emergency or routine. I have also found environmental services to be a vital part of noticing issues that are not always obvious, due to a busy environment. They might see it in a slightly calmer state. As part of rounds, I often check with them, as I do with the patient care staff, on a daily basis.
Practicing these methods will very likely prevent another principle, known as “the avalanche principle.” As many of us know or have found out, if you do not keep up with your equipment issues, it all will come tumbling down on you. Good luck, and may your parachutes operate properly.
Mark Brideson has been in the biomedical field since 1986. He currently works as a biomedical equipment technician in the Sacramento, Calif, region. For more information, contact .