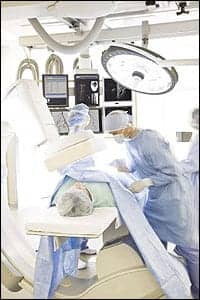
Hybrid rooms can vary significantly in design based on the specific clinical and economic objectives at each facility.
Biomedical professionals need to be aware of the latest trend in OR design: the hybrid surgical suite. The term “hybrid” is a word that has become increasingly popular in reference to automobiles that can operate on more than one kind of propulsion system—either independently or at the same time. And when it comes to a recent trend in operating room (OR) design, no other word would be more appropriate.
Modern hybrid ORs have been around for close to a decade, but as with many medical innovations in the acute care setting, they are only now being adopted on a wider scale. As the trend gains acceptance, it is in the best interest of today’s clinical/biomedical engineer to understand what hybrid ORs are, why they are becoming so popular, and why clinical/biomedical engineers need to be involved in the development and operation of hybrid ORs.
What Is a Hybrid?
The broadest definition of a modern hybrid OR is a dedicated room containing both imaging equipment and devices for surgical applications. Combining this equipment allows clinicians to diagnose and operate on a patient under a single anesthesia event. The result is often better economics for the facility and better clinical outcomes for the patient. Economic because more procedures can be done in a shorter period of time, and clinical because being anesthetized once in lieu of multiple times is less risky, although there can be other clinical benefits as well.
Bruce Landau, a radiographer in the vascular surgery imaging department of the Hospital of the University of Pennsylvania in Philadelphia, has been involved with implementing two hybrid OR suites. He says, “Most of the patients that come into the [hybrid] OR end up having an endovascular procedure that requires a postop CT. If the surgeon feels he has an endo leak he’d like to treat, we can do a scan right there in the OR and effect the repair immediately.”
In practice, hybrid rooms can vary significantly in design based on specific clinical and economic objectives set forth by the clinicians, administrators, and support staff at each facility. While in principle hybrid rooms can be used by many different clinical specialties, in practice the most popular application is cardiology.
Part of the reason is that hybrid rooms cost more money to build than traditional ORs, and diagnostic and interventional cardiology are some of the few specialties that can bring in enough dollars to justify such an investment. According to The Advisory Board Company, a think tank specializing in performance improvement for health care facilities, the procedures most likely to benefit from hybrid rooms are high-end vascular procedures (abdominal aortic aneurysm repairs, carotid stenting), percutaneous valve procedures, and hybrid cardiac procedures involving both minimally invasive CABG and stenting.
Some biomeds may have heard or used the term “hybrid cath lab” as well as “hybrid OR.” In truth, the differences are somewhat semantic.
“It’s a hybrid cath lab if it’s used as a cath lab 51% of the time,” says Jack Kerr, AIA, a senior health care architect and planner with Array Healthcare Facilities Solutions, in King of Prussia, Pa. “But if it’s used as an OR 51% of the time, it will be called a hybrid OR. In reality, they’re both the same kind of hybrid setup.”
Different Setups for Different Needs
Kerr and his firm have helped design many different types of hybrid ORs for different applications. He says that there can be significant differences in the types of imaging equipment. “Adult hybrid rooms are single-plane, but in pediatrics they need the biplane because pushing a cath is so much more finite—the vessels are so much smaller with peds.”
In addition, the imaging technology itself has changed in order to better meet the design requirements of hybrid rooms.
Landau helped design and incorporate the imaging equipment in two hybrid rooms—one opened about 5 years ago, and another opened less than a year ago. “The older room has a floor mount (imaging unit); the newer one has a ceiling mount, which is more flexible for different kinds of imaging,” he says. “When set up for imaging, the rooms are mostly set up for vascular, but when imaging isn’t involved, they can be set up for many different kinds of procedures.”
Kerr has also seen the shift from floor- to ceiling-mounted imaging hardware, admitting that designing a room for conventional surgery was difficult when floor-mounted imaging equipment was required. “Subsequent to that, I’ve seen a number of things where all the imaging companies are doing extended ceiling-mounted rails for their lateral image, with extended cables so it can be pushed out of the sterile field for general surgical cases.”
There can be other equipment differences as well. At the University of Pennsylvania, “the older room has a cardiac package to do cardiothoracic procedures,” Landau says. “The biggest are percutaneously placed heart valves, which require a very high frame rate in order to visualize heart motion without blur. In the newer room, we’re capable of doing CT scans in-room as well as angiographic kinds of studies.”
It’s All Connected
In addition to the unique requirements placed on imaging equipment, hybrid rooms also bring data-management technologies to new levels, since information for multiple clinical teams must be efficiently and accurately captured, displayed, stored, and often transmitted outside the room.
According to Kerr, “the things that take a hybrid beyond just an OR with imaging in it is the incredible amount of specialized IT communications—having a number of large monitors on the walls that allow not only different data displays, but also video connection from there to a conference room or other facility. There may often be cameras built into the OR lights and additional monitor booms hanging from the ceiling that allow the image to be brought in close to the physicians.”
Landau agrees that information technologies are central to any hybrid installation and present some unique challenges. “Of course, a lot of the imaging is recorded, and there are many, many different kinds of formats to take the images and convert them into the appropriate format for everything from presentations, to magazine articles, and newspapers, so that information can be used to educate other people.”
Naturally, Landau’s biggest concern during procedures is making sure the clinicians have the information they need, when they need it. “I can route images from any device to any monitor in the room,” Landau says. “I can also pull up images from storage servers if they want to view past x-rays or ultrasounds and route them to the AV system so they can see them tableside. So the displays can be used to give doctors real-time information as well as stored information during a particular procedure. I can also pull images from other rooms, if necessary, even if they’re on another floor.”
Claire Powers, clinical engineering OR specialist at Beth Israel Deaconess Medical Center in Boston, oversees two hybrid rooms built at different times for different purposes. The first room, built in 2006, was designed for cardiac catheterization and bypass procedures.
“That room has a CT scanner in it,” she says. “The room is larger than a standard OR and has a video routing system with about 18 or so monitors for displaying hemodynamic images, along with two separate endoscopic cameras.” As a teaching hospital, she says that the room is often used to record procedures for teaching purposes.
She agrees that data management is critical. “Clinicians want to be able to take data and put it anywhere they want—wherever it needs to go,” she says.
For Biomeds, Some of the Same
On the other hand, Powers says that from a clinical/biomedical engineer’s perspective, her day-to-day responsibilities for hybrid rooms are very similar to standard OR suites—except that there is simply more equipment to service. “We have three other minimally invasive suites on the West campus, along with five in the East campus,” she says. “Thy hybrid rooms are very similar from my point of view to those. The only difference is that the hybrid rooms have more monitors, as well as the cardiac equipment, that I’ll service. So it is more work.”
As with any imaging equipment, the role of clinical engineering will vary depending upon any service agreements that may be in place with vendors. “I service all of the monitoring equipment—light source, insufflator, camera controllers, and video router,” Powers says, adding that the hybrid OR table is part of the imaging system and is therefore covered by the vendor’s service agreement.
Some of the New
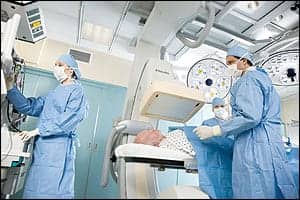
Hybrid rooms bring data management technologies to new levels, since information for multiple clinical teams must be efficiently and accurately captured.
Powers views the planning process, as well as equipment upgrades, as more of a challenge than ongoing maintenance for hybrid rooms. “You need to know how long things will be serviceable, what the estimated replacement date would be,” she says. “You need to know what type of signals will be routed, any other ancillary equipment that might be needed, while also planning for possible future needs.” It’s a difficult balancing act for clinical/biomedical engineers, who need to help harmonize many different clinical, economic, and technical needs.
As Powers puts it, “There may be certain limitations with Brand A that are not compatible with Brand B, so that needs to be harmonized within the room—or even with other rooms. Obviously, the manufacturers should be involved, but be sure to get clear specifications from them so those kinds of compatibility issues can be solved up front. I’ve had other hospitals call me to ask about hybrid rooms. I just tell them to get as much in writing as possible from manufacturers.”
Specifically, Powers recommends that manufacturers provide concise wiring diagrams—not just block diagrams—and that they label all wiring clearly so that clinical engineering can review the diagrams with other experts, like electricians, before anything is installed.
It has also been her experience that establishing clear areas of responsibility can prevent frustration down the road when multiple vendors are working together. “For example, if we need to route wire for a Brand A video system through a Brand B boom, who is going to actually pull wires? That’s why it’s important to get in writing who’s going to take care of what. Otherwise, you might hear, ‘Well, I’m not touching that; it’s another vendor.’ You can go around in circles if project management isn’t very clear.”
Get In Early
BJ Cumbie, corporate manager, clinical engineering at Aurora Healthcare in Milwaukee, oversees 14 different hospitals. He was part of a large team who investigated the implementation of hybrid OR rooms at two of Aurora’s facilities, and although the projects did not move forward due to budgetary reasons, Cumbie learned a great deal about hybrid rooms and the challenges associated with them.
Cumbie was involved from the beginning—even in the early conceptual stages. The cross-functional team looked at multiple specialties, including cardiology and neurology, when analyzing the hybridization process. “What we tried to do is make the rooms available for a broad spectrum of different utilization in order to get a good return on investment,” he says.
In order to do that, they took a hard look at integrating MRI into the surgical suite, but that appears to be one area where technology has yet to catch up. “There were some significant technology barriers,” Cumbie says. “For example, trying to find an OR table that was MRI compatible was impossible—it doesn’t exist. There were all kinds of issues related to the magnetic field, like surgical instruments that needed to be MRI compatible. Often there was simply no solution.”
|
Do you need surgical equipment? Check out our Buyer’s Guide. |
Eventually, the team took a step back and looked at more conventional imaging technologies for the hybrid areas, like CT scanners. “We looked at the idea of a single CT unit feeding multiple surgical rooms,” Cumbie says. “There was a lot of discussion about what you would actually need to do to prep the patient to go in there. So we didn’t just address the equipment itself. It was a much broader approach that involved physicians, anesthesiologists, biomed, radiology, nursing, and others.”
For Cumbie, that multifunctional approach yielded fruit beyond just the hybrid project itself. “Being from biomed, my focus has always been on the equipment, but this process expanded my view,” he says. “I developed a very good relationship with our OR director, and we really gained a lot of respect for each other’s experiences and knowledge. That respect is still in place long after the project itself is over. The relationships are still there, the mutual respect is still there. The different relationships show you so many different aspects to a problem. Although we have a tendency to get so secularized, when you work closely together with professionals from many different functions, it gives you an idea of what a real problem-solving team is all about.”
Kerr agrees that biomeds should be involved in hybrid planning from the earliest stages. “If the facility is even thinking about a hybrid, someone from clinical engineering should try to get onto that committee as early as possible, because a lot of the decisions are made up front,” he says. “It’s critical for biomed to be involved, because they’ll take the needs of the users and make sure that any new solution out there will work with other devices. It’s incredibly important for clinical engineering to be involved in early stages to make sure it will all work.”
Kent Lupino is a contributing writer for 24×7. For more information, contact .





