If one were to ask a clinical/biomedical engineer if ultrasound systems (newer ones, of course) are reliable devices, the reply would typically be yes. “Ultrasound equipment is generally very reliable when it is properly maintained,” says Henry Quinones, senior biomed at the University of Vermont, Instrumentation and Technical Services, Technical Services Partnership, in Burlington, Vt. “I have seen more repairs caused by the user than system malfunctions.”
Quinones stipulates that this does not mean the devices never fail. Sometimes, a clinical/biomedical engineering department can see a spate of issues. But, in general, newer-generation ultrasound systems incorporating advanced motherboards do not experience the same frequency of problems, such as system crashes and lost data, that were seen in older models.
Today, some of the more common, more easily resolved, and more inexpensive issues seen on ultrasound machines involve the moving parts—wheels, brakes, and steering equipment. Cosmetic issues, such as the front panel, can also require regular upkeep. Abhijeet Bhat, MS, CRES, clinical engineering supervisor/project manager in the department of clinical engineering at the UMass Memorial Medical Center in Worcester, Mass, notes it is typical to replace the front panel on one of the facility’s 52 units every year. According to a study completed at UMass Memorial Medical Center, however, these problems are not the biggest issue.
Approximately one-third or about 30% of ultrasound-related problems seen at the center during its study were related to the device itself. “The motherboard was defective, the power supply had gone bad, or the software had crashed,” Bhat says. Though easily fixed, often in-house, these problems can be expensive; power supplies can cost as much as $10,000, Bhat notes.
Probes, however, have both categories outnumbered, outcomplicated, and outpriced. Bhat’s team found that probes alone were responsible for about one-third of the ultrasound-related calls at UMass Memorial; repairs are rarely handled in-house; and to have them completed elsewhere can cost as much as $30,000. “It’s $27,000 to get a 3D TEE [transesophageal] probe repaired,” Bhat says.
Probing Answers
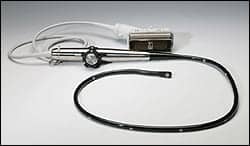
Damage to TEE probes includes bite marks on the probes and lens scratches.
Photo courtesy of MEDRAD
Murphy’s Constant—which states that matter will be damaged in direct proportion to its value—applies, and TEE probes tend to be the most problematic of all the ultrasound probes. This is in part because they are difficult to carry. Other types of probes are usually designed to plug into and be transported on the instrument.
“Some might disagree, yet the type of probe that tends to be more problematic in my case is the TEE probe,” Quinones says. “The endo, liner arrays, etc, have not been troublesome.” Typically, the issues are tied to misuse and tend to fluctuate over time and with turnover.
Many biomed departments can track use failure through their clinical equipment management systems to monitor behavior and develop educational strategies. When Bhat noticed that use failures related to TEE probes were starting to climb at his facility, the department began an initiative to correct the trend.
The first step was to shadow a tech throughout the entire process, from picking up the probe, through the exam, and back to the utility room. The goal was to identify areas where education, process modification, and/or new equipment might prove valuable and reduce probe problems. The result was a four-point plan addressing issues commonly seen and often addressed by other biomed departments that have examined this process.
After Each Use
“The most frequent problem we have with the TEE probes is the doctor or technician not using the bite guards, which causes bite marks in the probes,” says Dennis S. Vowels, imaging support specialist at Baylor Health Care System in Dallas. Other damage caused from improperly followed procedures can include scratches on the lenses and puncture marks on the sleeve.
These openings can permit liquid, often corrosive, to get into the mechanics of the device, interfering with its performance and requiring expensive repair or replacement. “Flooding the probe is perhaps the most expensive issue to tackle,” Quinones says.
Of course, the best way to prevent the issue is to perform the ultrasound procedure properly and to always use the bite guard. “But sometimes they don’t,” Vowels says. So many biomeds implement an alternate strategy.
Bhat’s team decided that requiring an electrical safety test after each patient use and before disinfection would not only help to eliminate damage through leakage but also improve patient safety and care quality.
A Clean Break
Newer generation systems are generally reliable.
Photo courtesy of Siemens
Standardizing the disinfection process can also help to reduce damage by leakage as well as mitigate wear and tear. Alcohol-based cleaning fluids should be avoided. “These tend to deteriorate the membranes of the probes and introduce problems,” Vowels says, noting probes experiencing this damage would not pass an electrical test.
At UMass, it was decided that the fourth campus, which had not yet upgraded to an automated disinfection process, would do so, and it allocated the budget to acquire the same instrument used successfully on the other three campuses. The 15-minute cycle requires 1 minute of operator time, minimizes potential disinfection-related probe damage, and provides a printed report.
Safe Transport
Equally valuable acquisitions were made to improve safety during transport at UMass. During the use study, the clinical engineering department discovered that the ultrasound techs and clinicians were hand carrying the probes from storage to the exam room and on to disinfection. This left the delicate instrument exposed to harm.
“We have had a clinician walking down the hallway drop a probe and break the tip. Bhat says. “Once that happens, it’s about $12,000.” Unfortunately, after trying different methods, there seemed to be no effective way to carry the probes. The best solution was found to be a container, a conclusion many other departments share.
“It keeps them safe so they’re not swinging around, susceptible to banging into things as they’re transported,” Vowels says. The use of canisters can significantly reduce damage during transit. In addition, proper storage when not in use can have similar benefits.
User Training
One of the best, and possibly least expensive ways, to reduce use damage is through user education. “Proper training can reduce recurring issues—training, retraining, and patience,” Quinones says. This training may be delivered during formal sessions or on a less formal, continuing basis.
“We try to educate the customers as we do our preventive maintenance: discussing what kinds of chemicals they can use on the unit, leaving paperwork with the types of cleaning fluids they can use, showing them how to utilize the tools the vendor manufactures on the unit to hang the probes so they avoid those typical situations,” Vowels says.
Bhat’s team also relies on continuous communication to ensure proper procedure on the part of the users. The group is developing standard work that will become part of the technicians’ competencies. “We want to make them aware of what happens if they don’t use the equipment properly and the costs that are involved. Many times, I don’t think the techs or fellows know how expensive some of these things, and the probes, are,” Bhat says.
Care In the House
In some cases, the biomed department can save further money and improve instrument uptime by bringing ultrasound and probe care maintenance in-house. At UMass, cost savings were projected at 35% with the implementation of an in-house program, and while it is just starting to collect the numbers, uptime has already improved.
“We don’t have to contact a vendor to come in or ship these probes out to have them looked at,” says Jonathan Riscica, a clinical engineer studying at the University of Connecticut clinical engineering program and an intern at UMass Memorial Medical Center. “Where it might take a few days to a week to get one of these probes back, we can now have somebody go in and take less than 10 minutes, an hour max, to look at one of these probes and figure out what’s going on.”
In general, the most benefit associated with an in-house program is seen in hospitals with larger inventories. Smaller hospitals with fewer systems may find that repairs use more funds than a service contract would have cost, whereas a large hospital with a big enough install base of ultrasound systems can mitigate this risk through volume. “Even if half of my ultrasound systems have issues this year and half do not have any issue, my total cost still remains below the cost of a service contract,” Bhat says.
Before such an effort is undertaken, a strict accounting should be taken to determine the potential return on investment. “The facility in question would have to assess the necessary staff, the required amount of training needed, the essential tools for the job, the feasibility to cover cost, effectiveness, time, and the age of equipment in need of repairs,” Quinones says.
“We looked at how much we spend in contracts, and we looked at our histories and determined how many parts we had replaced in last 5 years,” Bhat says. “We averaged the cost and found it would be cheaper to bring all of the service in-house.”
Partners and Personnel
UMass worked with a partner to achieve this most cost effectively. “Ultrasound machines are high-end machines, and you really need to have a strong partner if you want to bring this service in-house,” Bhat says. “That partner should be able to provide training and tools, and as the technology changes, needs to have all the resources to keep up with those changes and get your engineers trained for the new technology.” The right partner can even help to determine the return on investment.
Of course, not all ultrasound device and probe problems can be completely managed in-house or even by a third-party partner. “There are high-end probes, which are manufactured by large manufacturers, and the third-party vendors still do not have the capability to repair those devices,” Bhat says.
However, a good majority of the existing inventory does not share these limitations. “Probably 75% of [our ultrasound-related] calls are handled by biomed and 25% by the vendor, depending on the situation,” Vowels says. The ultrasound inventory at Baylor includes slightly over 200 machines managed by three specialists; Vowels works only on ultrasound devices.
Staffing, in general, depends on the number of units within the facility. It may be possible to launch a new in-house ultrasound service with existing staff, but depending on the individual facility’s situation, additional personnel may be needed to absorb the new burden, particularly if training is required. Bhat estimates a typical class covers 40 hours worth of material.
If a large enough group needs to be trained, and the right partner is selected, a department can bring the trainer to the health care institution and keep costs down by eliminating travel expenses. “All you have to do is make sure [the biomeds] are available for training and somebody else is taking calls,” Bhat says.
Tools and Procedures
Biomed training on ultrasound machines typically involves preventive maintenance, troubleshooting, and some repair, pending the device (eg, the ultrasound machine versus the TEE probe) and the manufacturer. Some companies protect the proprietary information on their newer models.
Typical preventive maintenance (PM) on the probes involves checking the probes, performing leakage tests, and running phantom tests on the probes, running diagnostics on the ultrasound machines, ensuring the system’s motherboards are functioning properly, cleaning the filters, checking the brakes, validating all of the modalities, and verifying that everything works on the unit.
“Inspecting all probes during a PM will help catch potential failures early and minimize lost time, will help reduce repair costs, and will allow the repair to be scheduled at the department’s convenience rather than as an emergency,” Quinones says.
The tools necessary to complete these tests and procedures include phantoms and leakage testing equipment. “Setup cost is on the high end for diagnostic tools, depending on what is acquired. Examples are phantoms, first-call systems, nickel-probe testers, and safety testers,” Quinones says. Partnering can help to reduce the capital needed for the initial investment.
Newer systems may also offer online diagnostics, where preventive and preliminary troubleshooting by the OEM occurs over the Internet. “It gives them an idea of what kind of parts might be needed before anyone is dispatched to the site,” Vowels says. The process can speed repair, increase equipment uptime, and improve technician effectiveness.
The end result is improved patient care, the main goal of any medical facility. As a result, administration buy-in is usually easy to obtain for an in-house effort. “In these difficult times, actually any issue that results in cost savings and an increase in patient safety usually gets buy-in from our administration,” Bhat says. “So our administration was very willing to implement this plan, which would essentially lower the cost of ownership of these probes and, of course, make sure, by implementing electrical safety, that these probes are safe for the patient.” Ask any administrator if improved safety and reduced cost is a reliable strategy, and the reply would typically be yes.
Renee Diiulio is a contributing writer for 24×7. For more information, contact .